NCERT Summary: Summary of Biology- 5
Blood
Blood is a bright red, viscous fluid that circulates through the blood vessels (not through lymphatic vessels) and constitutes about 8% of the total body weight. Blood has two main components:
- Formed elements - cells and cell-like structures (erythrocytes, leukocytes, platelets)
- Plasma - the liquid portion containing dissolved substances
Plasma
Plasma is the liquid component of blood. It makes up about 60% of blood volume; formed elements account for the remaining 40%. Plasma is approximately 90% water and 10% dissolved substances including proteins, glucose, ions, hormones and gases. Plasma:
- Acts as a buffer to maintain blood pH near 7.4
- Transports nutrients, metabolic wastes and dissolved salts
- Contains proteins (albumins, globulins, fibrinogen) that assist in transport of molecules (for example, lipids and cholesterol)
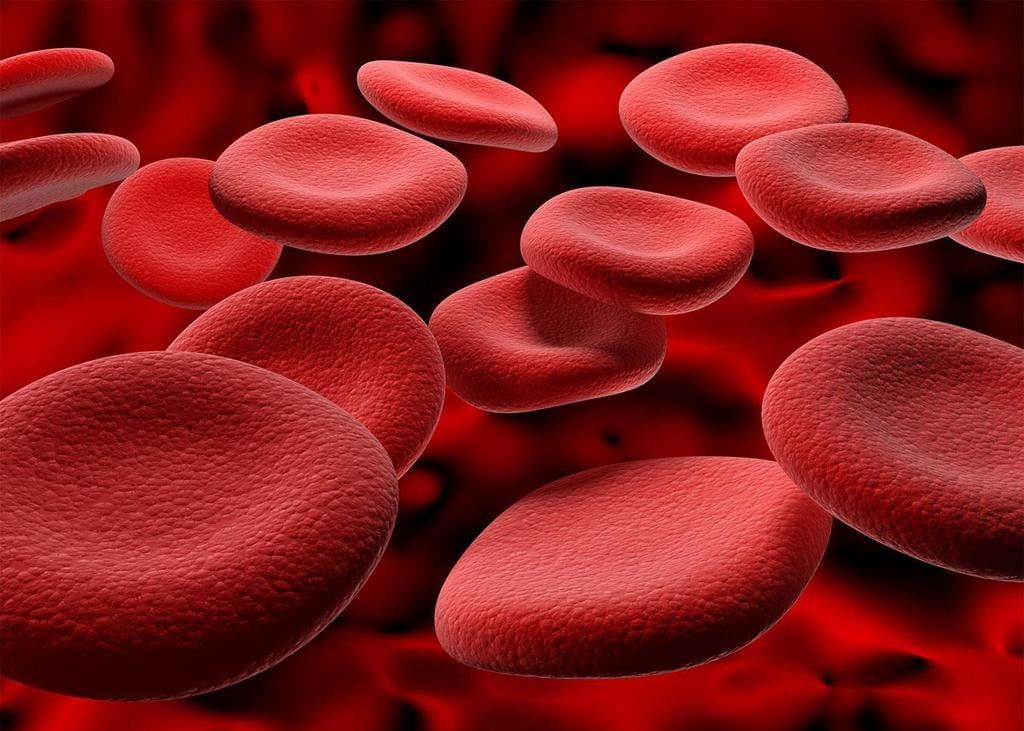 Blood
BloodRed Blood Cells
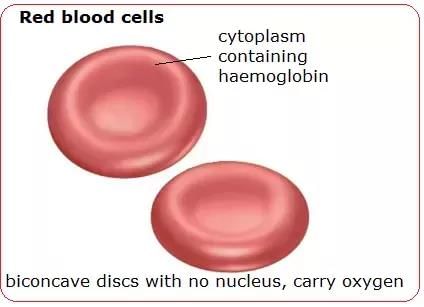
Red blood cells (erythrocytes) are specialised for oxygen transport. Key features:
- Shape: flattened, biconcave discs about 7 μm in diameter, which increases surface area for gas exchange
- Contain hemoglobin, the oxygen-carrying pigment; each erythrocyte contains about 200 million hemoglobin molecules
- Are anucleate (mature erythrocytes lack a nucleus)
- Typical concentration: 4-6 million cells per cubic millimetre of blood
- Approximately 25 trillion red blood cells in the human body (around one third of all body cells)
- Produced continuously in the red marrow of long bones, ribs, skull and vertebrae
- Lifespan is about 120 days; senescent cells are removed by the liver and spleen
- Iron from haemoglobin is recycled by the bone marrow; the degraded heme is excreted as bile pigments and contributes to the colour of faeces
- Production rate: roughly two million erythrocytes are produced each second to replace aged cells
White Blood Cells
White blood cells (leukocytes) function in the immune response. They are larger than erythrocytes, contain a nucleus and do not carry haemoglobin. Leukocytes constitute less than 1% of blood volume and are produced from stem cells in the bone marrow.
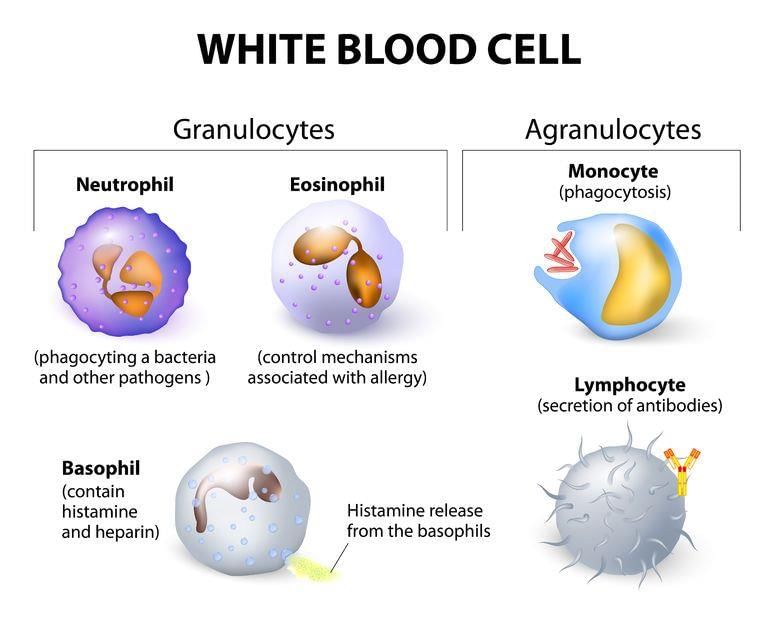
Major types of leukocytes and their primary functions:
- Neutrophils - migrate into tissues by squeezing through capillary walls; phagocytose (engulf) and destroy bacteria and foreign particles
- Macrophages - phagocytic cells derived from monocytes; release growth factors that stimulate white cell production and phagocytose antigen-antibody complexes
- Lymphocytes - key cells of specific immunity; include B-cells and T-cells
- T-cells - attack body cells harbouring viruses or abnormal cells directly
- B-cells - differentiate into plasma cells that secrete antibodies; antigen-antibody complexes are then removed by phagocytes
Platelets
Platelets are small cell fragments important in blood clotting.
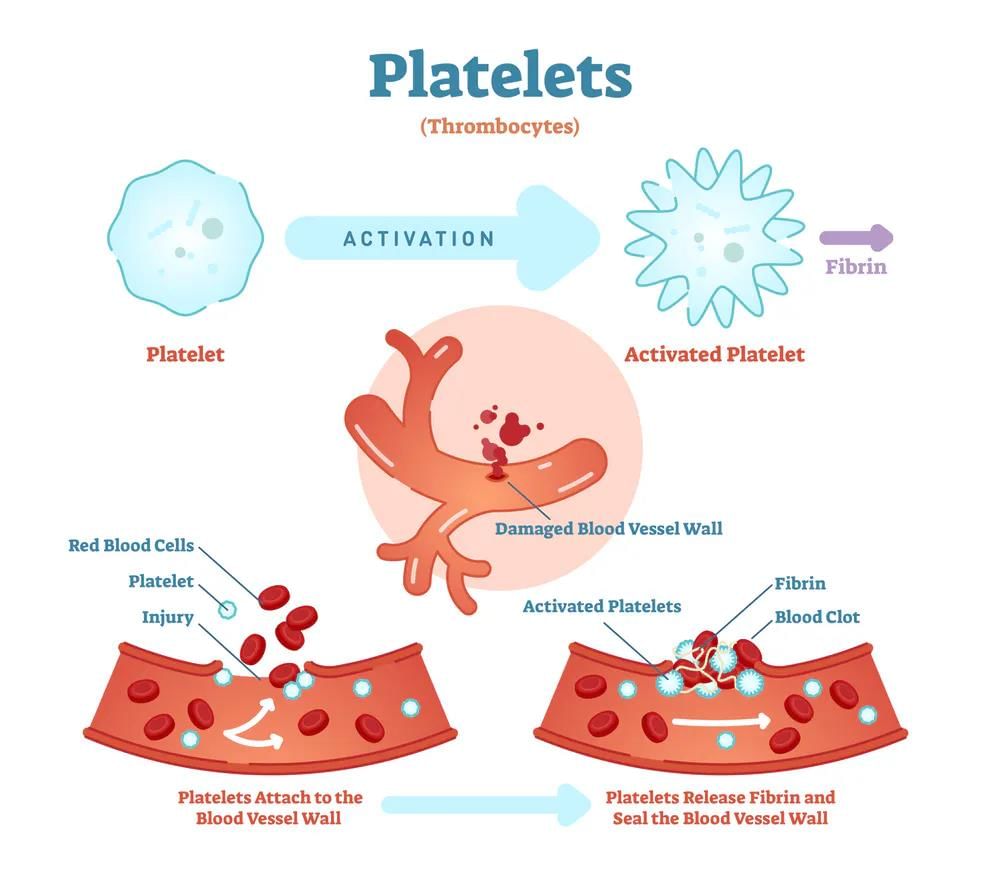
- Derived from fragmentation of megakaryocytes in bone marrow
- Carry chemicals required for the clotting cascade and adhere to damaged vessel walls to form a platelet plug
- Survive for about 10 days before removal by the liver and spleen
- Normal platelet count: approximately 150,000-300,000 per millilitre of blood
- Disorders: haemophilia (deficiency of clotting factors) prevents normal clotting; replacement of clotting proteins has been used in treatment but historically led to infections transmitted by contaminated blood products
The Reproductive System
1. Asexual Reproduction
Asexual reproduction allows organisms to produce many offspring rapidly without mating. It is advantageous when conditions are stable but reduces genetic variation.
- Common mechanisms: fission, budding, fragmentation, and formation of rhizomes and stolons
- Examples: starfish can regenerate a whole body from a fragment; many plants and some animals use vegetative propagation
- Lack of genetic variability in asexual populations can be disadvantageous under rapidly changing environmental conditions
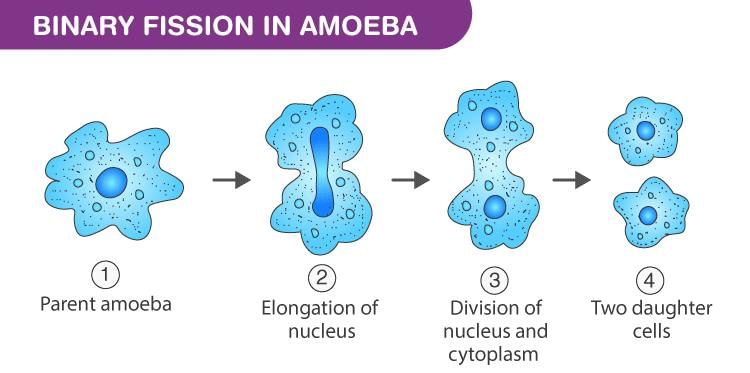
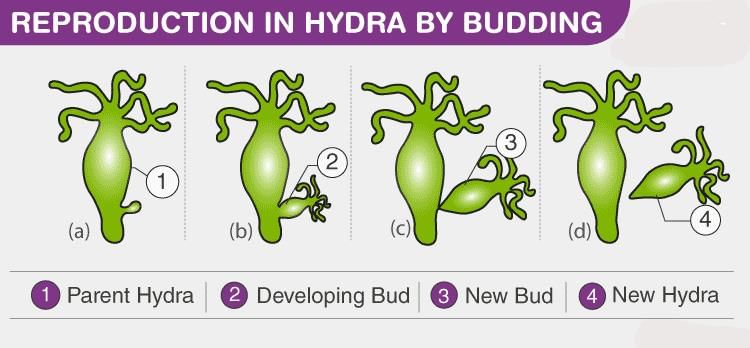
2. Sexual Reproduction
- Sexual reproduction produces new individuals by fusion of haploid gametes to form a diploid zygote
- Sperm are male gametes; ova (eggs) are female gametes
- Meiosis produces genetically distinct gametes; fertilization fuses two distinct haploid cells to restore diploidy
- Some organisms switch reproductive modes depending on conditions; for example rotifers reproduce asexually by mitotic egg production when conditions are favourable and switch to sexual reproduction, producing resistant zygotes, when conditions deteriorate
- Advantages: generates genetic variation that enhances population survival; costs include the requirement for two parents, courtship behaviours and associated energy expenditure
3. Human Reproduction and Development
Human reproduction normally involves internal fertilization and the coordinated action of hormones, the nervous system and the reproductive organs. Gonads produce gametes and sex hormones: testes in males and ovaries in females.
(a) The Male Reproductive System
- Testes are suspended in the scrotum outside the abdominal cavity to maintain an optimal temperature for sperm development
- Each testis contains extensive seminiferous tubules where sperm are formed by meiosis; approximately 250 metres of tubules are packed into each testis
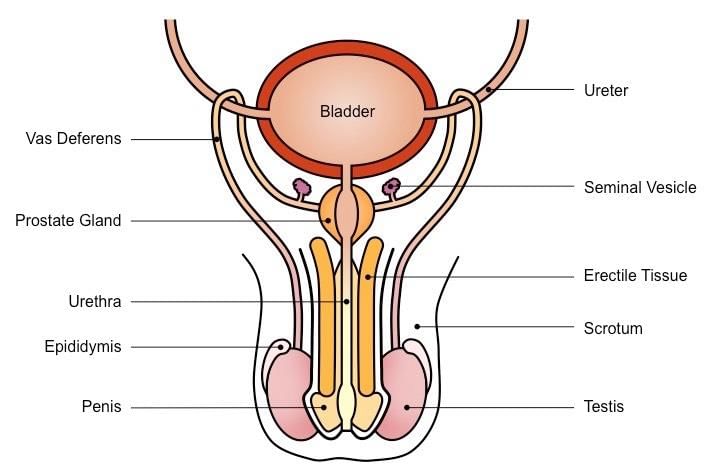
- Spermatocytes within seminiferous tubules undergo meiosis to produce spermatids, which mature into sperm
- Sperm production (spermatogenesis) begins at puberty and continues throughout life; several hundred million sperm can be produced each day
- Mature sperm are stored and further matured in the epididymis
- Endocrine control: the hypothalamus secretes gonadotropin-releasing hormone (GnRH), which stimulates the anterior pituitary to release follicle-stimulating hormone (FSH) and luteinizing hormone (LH)
- LH stimulates testicular cells to secrete testosterone, which is required for spermatogenesis and the development of male secondary sexual characteristics
- FSH supports spermatogenesis and sperm maturation; testosterone exerts negative feedback on GnRH secretion
- Pathway of sperm: seminiferous tubules → epididymis → vas deferens → ejaculatory duct → urethra; accessory glands (seminal vesicles, prostate, bulbourethral glands) add seminal fluid that nourishes and protects sperm
(b) The Female Reproductive System
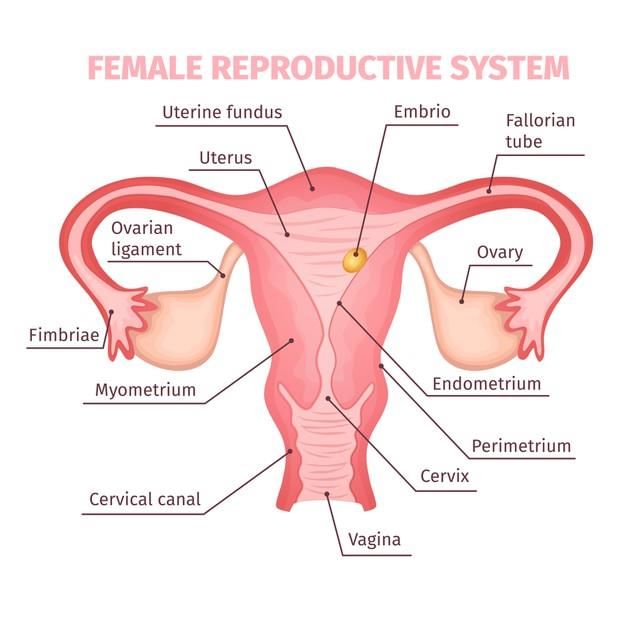
- Ovaries are located within the lower abdominal cavity and contain follicles composed of a developing oocyte surrounded by follicle cells
- At birth each female possesses a lifetime supply of developing oocytes arrested in prophase I of meiosis
- From puberty until menopause, typically one secondary oocyte is released each month; over a lifetime approximately 400-500 oocytes are ovulated
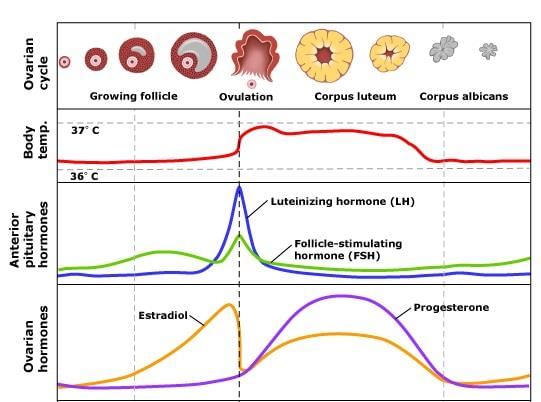
Ovarian Cycle
- The ovary cycles between a follicular phase (maturation of follicles) and a luteal phase (presence of the corpus luteum)
- These cycles are interrupted only by pregnancy and continue until menopause
- The ovarian cycle is usually about 28 days
- Midcycle ovulation (release of the oocyte) typically occurs around day 14; after ovulation the ruptured follicle forms the corpus luteum which secretes hormones to prepare the uterus for possible pregnancy
- The secondary oocyte passes into the oviduct (fallopian tube); fertilisation usually occurs in the upper third of the oviduct
- The uterus has an inner lining, the endometrium, where a fertilised egg implants; the cervix connects the uterus to the vagina, which receives the penis during intercourse and serves as the birth canal
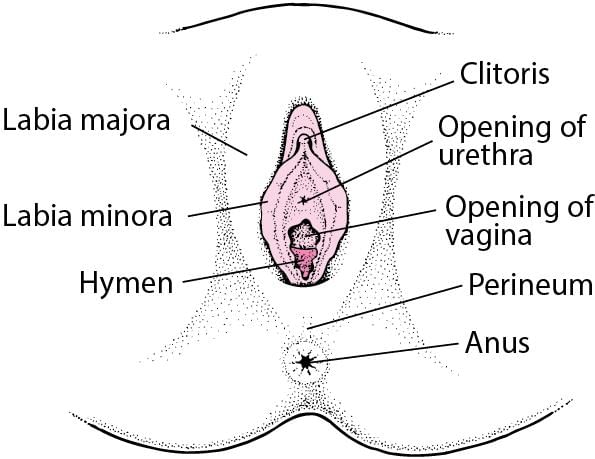
External Genitals
- The female external genitalia are collectively known as the vulva
- Labia minora - thin folds of skin just outside the vaginal opening
- Labia majora - larger folds that protect the genital area
- Clitoris - erectile organ important in sexual arousal; has a sensitive tip covered by a fold of skin
(c) Hormones and Female Cycles
- The ovarian cycle is hormonally regulated in two main phases: the follicle secretes oestrogen before ovulation; the corpus luteum secretes both oestrogen and progesterone after ovulation
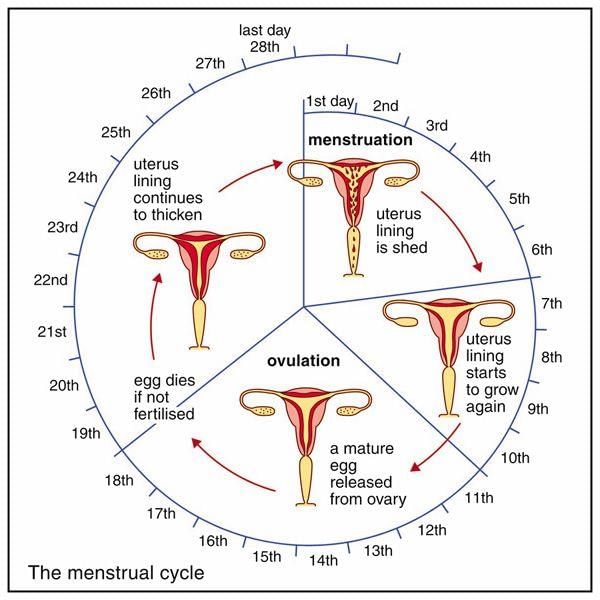
- The hypothalamus and anterior pituitary control the ovarian cycle; the menstrual cycle refers to changes in the uterus that are linked to the ovarian cycle
- Menstrual cycles vary, commonly between 15 and 31 days; the first day of menstrual bleeding is regarded as day 0
- During menstruation the uterine lining is shed as menstrual flow
- FSH and LH secreted on day 0 stimulate maturation of a single follicle and the secretion of oestrogen
- Rising oestrogen levels trigger a surge in LH that stimulates final follicle maturation and ovulation (midcycle)
- After ovulation the corpus luteum produces oestrogen and progesterone, which prepare the endometrium for implantation; if pregnancy does not occur, falling FSH and LH lead to corpus luteum disintegration and menstrual shedding
(d) Sexual Responses
- Humans do not have a fixed mating season; females can be sexually receptive throughout the year
- Four stages of sexual response: arousal, plateau, orgasm, and resolution
- Male arousal: blood flows into three columns of erectile tissue in the penis causing erection; female arousal: swelling around the vagina, erection of the clitoris and nipples, and secretion of vaginal lubricating fluids
- Intercourse and pelvic thrusting stimulate sensory receptors; orgasm involves rhythmic muscular contractions and intense pleasurable sensations
- Resolution: relaxation of muscles, slowing of breathing and return of the penis and other tissues to their non-aroused state
4. Sexually Transmitted Diseases

Sexually transmitted diseases (STDs) can affect sexual partners as well as the fetus and newborn. STDs may be grouped as follows:
- Category One - STDs that produce inflammation of the urethra, epididymis, cervix or oviducts; gonorrhoea and chlamydia are common and are treatable with antibiotics once diagnosed
- Category Two - STDs that produce sores on external genitals; genital herpes is a common example (antiviral drugs treat symptoms but do not cure); syphilis is bacterial and curable with antibiotics but can be fatal if untreated
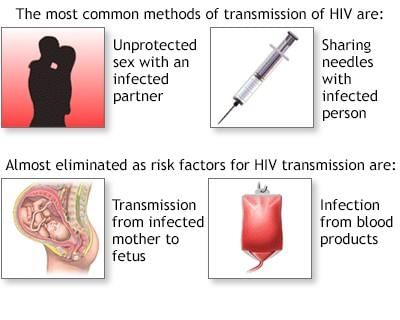
- Category Three - Viral diseases that affect systems beyond the reproductive tract; examples are AIDS (caused by HIV) and hepatitis B. These can be transmitted by sexual contact or blood, and infected individuals may be asymptomatic for years
5. Reproduction: Contraceptive Methods
Modern techniques can either enhance or reduce the chances of conception. Methods block one or more stages of reproduction: release/transport of gametes, fertilization, or implantation.
- Abstinence is the only method that is completely effective at preventing pregnancy and STD transmission
- Physical prevention (permanent surgical methods): vasectomy and tubal ligation
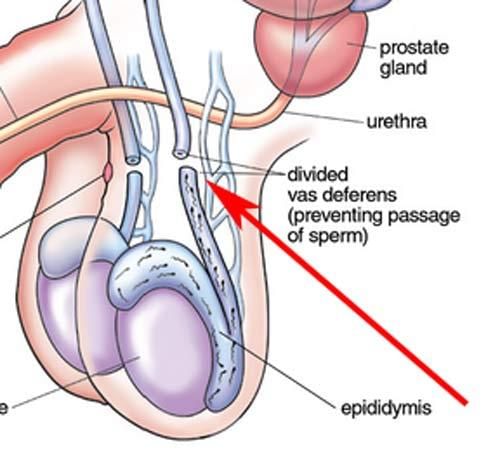
- Vasectomy - the vas deferens is cut and sealed to prevent sperm transport
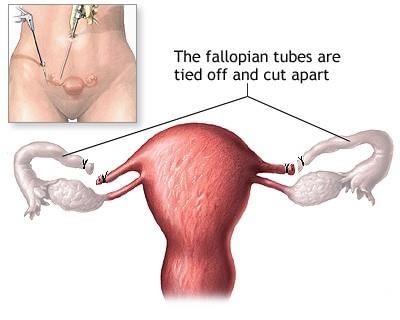
- Tubal ligation - oviducts are cut or tied so eggs cannot reach the uterus
- Oral contraceptives (birth control pills) - usually contain hormones that suppress FSH and LH release, preventing follicle development and ovulation; long-acting implants (e.g. Norplant) release hormones over time
- Emergency contraception (RU-486 / mifepristone) - interferes with implantation and early pregnancy processes; its use is ethically and legally controversial in many jurisdictions
- Barrier methods - condoms (male and female), diaphragms and spermicidal agents separate or destroy sperm; only latex condoms reliably reduce the transmission of STDs
- Diaphragms cap the cervix; spermicidal jellies or foams kill sperm on contact and must be applied before intercourse
6. Infertility
Infertility affects about 1 in 6 couples and may result from problems in gamete production, transport, fertilisation, or implantation.
- Leading causes in females: blocked oviducts (often due to untreated STDs)
- Leading causes in males: low sperm count, poor sperm motility, or blocked ducts
- Treatment options include hormone therapy to stimulate egg production, surgical correction of blocked ducts, and assisted reproductive technologies such as in vitro fertilisation
- Approximately 40% of infertility cases are attributable to male factors, 40% to female factors, and about 20% remain unexplained
7. Fertilization and Early Development
Functions of Fertilization
- Transmission of genes from both parents to the offspring
- Restoration of the diploid chromosome number reduced by meiosis
- Initiation of embryonic development
Steps in Fertilization
- Contact between sperm and egg
- Entry of one sperm into the egg
- Fusion of sperm and egg nuclei
- Activation of embryonic development
Cleavage
Cleavage is the series of rapid mitotic divisions that convert the single-celled zygote into a multicellular embryo. Key points:
- Cleavage partitions the zygote cytoplasm into smaller cells (blastomeres) and produces the blastula, a ball of cells surrounding a fluid-filled cavity called the blastocoel
- Example: frog embryos can divide to produce tens of thousands of cells within about 40 hours
- Smaller cells have a higher surface-to-volume ratio, improving exchange of oxygen and nutrients
- Maternal RNAs and other determinants are distributed among blastomeres, contributing to early cell differentiation
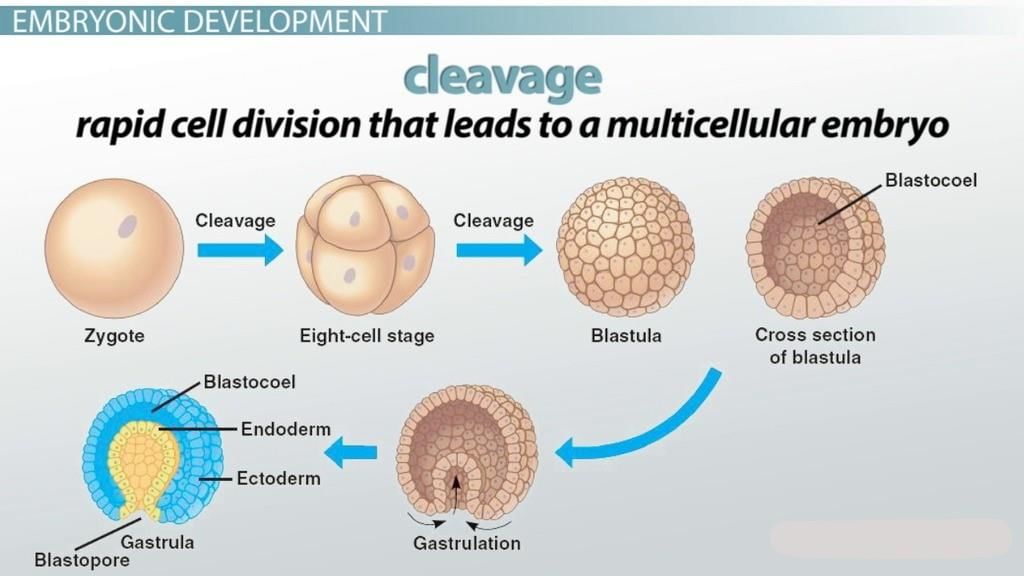
Gastrulation
Gastrulation involves coordinated cell movements that establish the three primary germ layers:
- Ectoderm - forms outer structures such as skin, hair, epithelial linings and the nervous system (brain, spinal cord)
- Mesoderm - forms muscles, bone, blood, connective tissues, kidneys and reproductive organs
- Endoderm - forms the linings of the digestive and respiratory systems and many internal organs (liver, pancreas, gall bladder) and several endocrine glands (thyroid, parathyroids)
Invagination and Body Axis Formation
- After gastrulation the embryo's body axes become apparent; in chordates the neural plate folds to form the neural tube (future central nervous system)
- The notochord (from mesoderm) forms beneath the neural tube and contributes to axial support and signalling for surrounding tissues
- Mesoderm segments into somites that give rise to segmented structures such as body wall muscles and vertebrae
Pattern Formation and Induction
- Pattern formation is the process by which cells acquire positional information and develop structures appropriate to their location
- Gradients of signalling molecules provide positional cues; homeobox (Hox) genes are key patterning genes that work with these gradients to establish body plans and organ identity
- Induction describes how one cell or tissue influences the developmental fate of another via chemical signals or physical contact (the developing vertebrate eye is a classic example)
- As development proceeds, differential gene expression leads to cell differentiation and organ formation
Various Stages of Fertilization
- Fertilisation usually occurs in the upper third of the oviduct. Sperm reach the oviduct within minutes to hours after ejaculation by swimming via their flagella
- Of the hundreds of millions of sperm deposited, only a few thousand reach the egg and typically only one sperm fertilises the oocyte
- Fusion of a sperm with the secondary oocyte triggers chemical changes in the oocyte membrane that prevent polyspermy (entry of additional sperm)
- Entry of the sperm completes meiosis II in the oocyte; fusion of the male and female pronuclei produces the diploid zygote
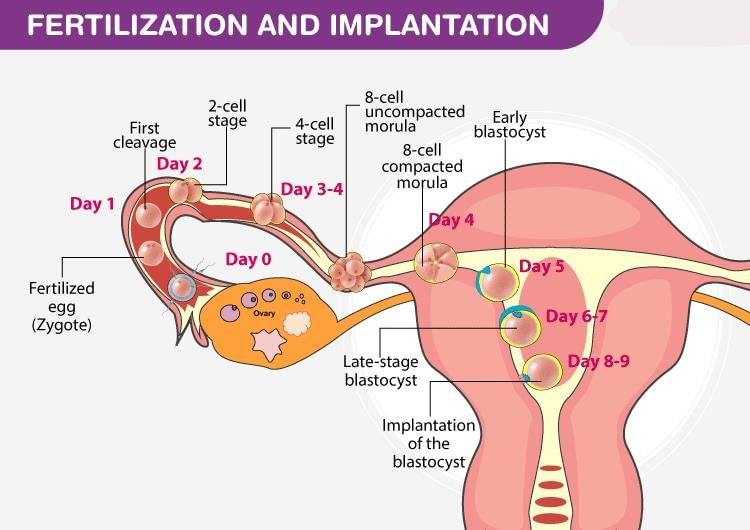
(a) Travels of the Young Zygote
- Cleavage begins while the zygote is still in the oviduct, producing a compact ball of cells called a morula
- The morula enters the uterus and continues dividing to form a blastocyst
(b) Implantation
- The uterine lining (endometrium) becomes receptive and the blastocyst implants via the trophoblast layer
- About twelve days after fertilisation the trophoblast forms a two-layered chorion that contributes to the placenta
- The chorion secretes human chorionic gonadotropin (hCG), which maintains the corpus luteum until the placenta is established and begins producing oestrogen and progesterone
- Home pregnancy tests detect elevated hCG concentrations in urine
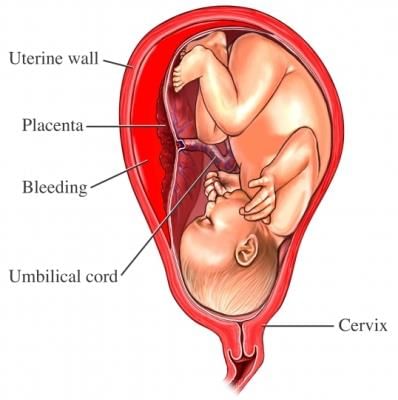
(c) Placenta
- The placenta is a specialised organ in which maternal and embryonic tissues interlock to mediate exchange of gases, nutrients and wastes between mother and embryo
- The umbilical cord connects the embryo/fetus to the placenta and contains vessels that carry oxygenated nutrient-rich blood to the embryo and remove wastes
FAQs on NCERT Summary: Summary of Biology- 5
| 1. What is plasma and what is its role in the blood? |  |
| 2. How is blood plasma different from whole blood? |  |
| 3. What are the proteins present in blood plasma and their functions? |  |
| 4. How is plasma separated from blood for medical purposes? |  |
| 5. Can plasma be used as a treatment for certain medical conditions? |  |





