Antibiotics, Painkillers & Development of Drugs
Antibiotics & Painkillers
- When treating a disease there are two types of medication that an individual can take:
- Medicines that treat the cause of the disease - antibiotics
- Medicines which treat the symptoms of the disease - eg. painkillers
- Antibiotics, such as penicillin, are medicines that help to cure bacterial disease by killing infective bacteria inside the body
- The use of antibiotics has greatly reduced the deaths from infections in the last century
- Only certain antibiotics will work on certain diseases, however, so a doctor will prescribe different antibiotics depending on the type of infection (see Culturing Microorganisms)
- It is important that specific bacteria should be treated by specific antibiotics that are known to work against them
- Antibiotics work by stopping bacteria cellular processes such as the production of the cell wall - they affect processes usually only in bacteria so are not harmful to animal cells
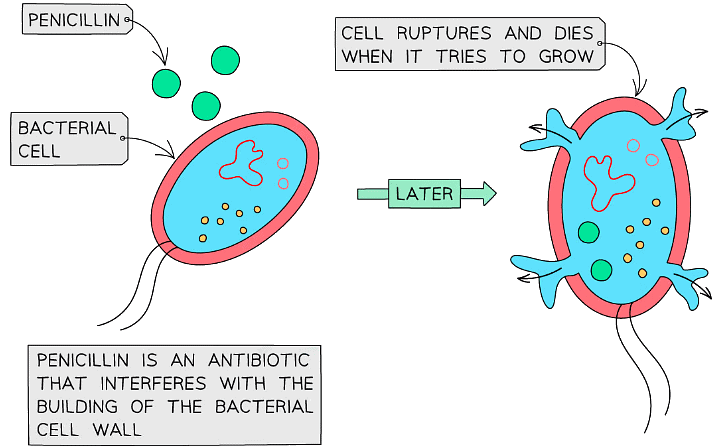 Penicillin was the first antibiotic to be discovered and is widely used, although resistance is a problem
Penicillin was the first antibiotic to be discovered and is widely used, although resistance is a problem - Antibiotics will not work against viruses, as viruses reproduce inside cells. It is difficult to develop drugs that kill viruses without also damaging the body's tissues
- Painkillers and other medicines are used to treat the symptoms of disease but do not kill pathogens (eg. ibuprofen can reduce pain and inflammation)
Antibiotic Resistance
- The use of antibiotics has increased exponentially since they were first introduced in the 1930s
- In that time they have saved millions of lives
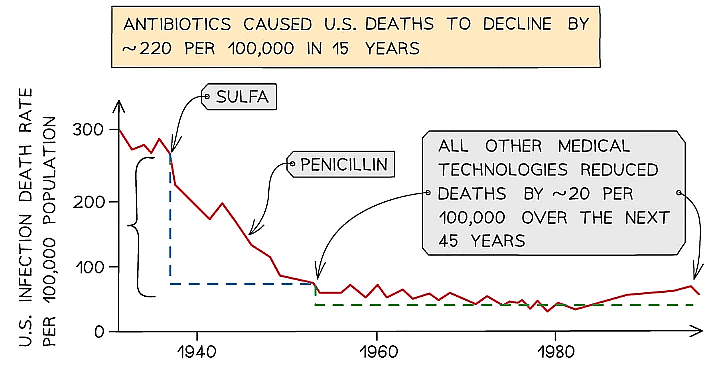 The introduction of antibiotics has had one of the largest impacts on global health, shown by this example in the USA
The introduction of antibiotics has had one of the largest impacts on global health, shown by this example in the USA - However, since their discovery and widespread use, antibiotics have been overused and antibiotic resistance has developed in many different types of bacterial species
- Bacteria, like all organisms, have random mutations in their DNA
- One of these mutations may give them resistance to an antibiotic
- If an organism is infected with bacteria and some of them have resistance, they are likely to survive treatment with antibiotic
- The population of the resistant bacteria will increase
- If the resistant strain is causing a serious infection then another antibiotic will be needed
- A strain of Staphylococcus aureus has developed resistance to a powerful antibiotic methicillin, this is known as MRSA (Methicillin resistant Staphylococcus aureus)
- MRSA can infect wounds and is difficult to treat without antibiotics
 Bacteria evolve rapidly as they reproduce quickly and acquire random mutations - some of which confer resistance
Bacteria evolve rapidly as they reproduce quickly and acquire random mutations - some of which confer resistance
- To reduce the number of bacteria that are becoming resistant to antibiotics:
- Doctors need to avoid the overuse of antibiotics, prescribing them only when needed - they may test the bacteria first to make sure that they prescribe the correct antibiotic
- Antibiotics shouldn't be used in non-serious infections that the immune system will 'clear up'
- Antibiotics shouldn't be used for viral infections
- Patients need to finish the whole course of antibiotics so that all the bacteria are killed and none are left to mutate to resistant strains
- Antibiotics use should be reduced in industries such as agriculture - controls are now in place to limit their use in farming
- Good hygiene practices such as handwashing and the use of hand sanitisers have reduced the rates of resistant strains of bacteria, such as MRSA, in hospitals
- The isolation of infected patients to prevent the spread of resistant strains, in particular in surgical wards where MRSA can infect surgical wounds
Discovering New Drugs
- Traditionally drugs were extracted from plants and microorganisms
- New drugs are being developed all the time by scientists at universities and drug companies around the world
- Lots of the medications that we use today are based on chemicals extracted from plants
- The heart drug digitalis originates from foxgloves
- The painkiller aspirin originates from willow
- Penicillin was discovered by Alexander Fleming from the Penicillium mould
- Most new drugs are synthesised by chemists in the pharmaceutical industry. However, the starting point may still be a chemical extracted from a plant
Drugs from plants table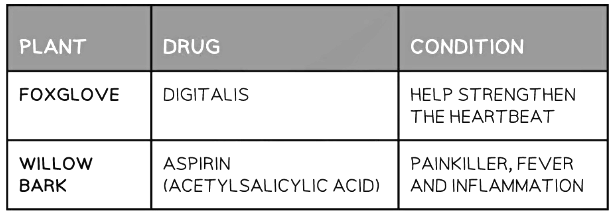
- Penicillin was first discovered by Alexander Flemming in 1928. He left some Petri dishes that had been contaminated with mould and found the bacteria would not grow near the mould
- He discovered that the mould (Penicillium notatum) was releasing a chemical (penicillin) that killed the bacteria surrounding it
- New drugs are now developed by the pharmaceutical industry. Many of these still have plants as their source
Testing New Drugs
- All new drugs need to be tested and trialled before they can be used in patients. They are tested for:
- Toxicity - does it have harmful side effects?
- Efficacy - does the drug work?
- Dose - what dose is the lowest that can be used and still have an effect?
- The results of any testing are then peer-reviewed to make sure that the results are described accurately. The results would then be published in journals
Developing New Drugs
- Preclinical testing is done in a laboratory using cells, tissues and live animals
- Clinical trials use healthy volunteers and patients
- Very low doses of the drug are given at the start of the clinical trial
- If the drug is found to be safe, further clinical trials are carried out to find the optimum dose for the drug
- In double-blind trials, some patients are given a placebo
The 3 stages of drug development
- Preclinical Testing
- The drug is tested on cells in the lab
- Computer models may also be used to simulate the metabolic pathways that may be taken by the drug
- Efficacy and toxicity are tested at this stage
- Whole organism testing
- The drug is tested on animals to see the effect in a whole organism - all new medicines in the UK have to have tests on 2 different animals by law
- Efficacy, toxicity and dosage are tested at this stage
- Clinical trials
- The drug is tested on human volunteers first, generally with a very low dose then increased. This is to make sure it is safe in a body that is working normally
- The next stage is to test on patients with the condition.
- The patients are often split into two groups; one given the drug the other given a placebo. This is called a double-blind study - neither the doctor nor the patient knows if the patient is getting the placebo or the active drug
- Once the drug is found to be safe then the lowest effective dose is tested at this stage
Future medications
- Pharmaceutical companies are always looking to find new medications these include:
- Vaccinations to different diseases
- Antibiotics that have a different action on the bacteria, so that bacteria are not resistant to them
- Painkillers with fewer side effects
- Antiviral drugs that don't damage the body's tissues
- Sources of these medications may be plants or microorganisms
Exam Tip: You should be able to describe the process of discovery and development of potential new medicines, including preclinical and clinical testing in the exam.
Solved Examples
Example 1: HIV/AIDS is what type of pathogen?
HIV/AIDS is a virus.
Example 2: Salmonella is what type of pathogen?
Salmonella is a bacterium.
Example 3: Rose black spot is what type of pathogen?
Rose black spot is a fungus.
Example 4: Malaria is caused by what type of pathogen?
Malaria is caused by a protist.
Example 5: What term describes an organism that transmits a disease?
A vector is an organism that transmits a disease.
Example 6: How is measles often transmitted?
Measles is often transmitted through the air. Escherichia coli is an example of a disease transmitted by uncooked food.
Example 7: In which foods is Salmonella more likely to be found?
Meat, eggs and poultry are more likely to contain Salmonella.
Example 8: Which of these does not prevent the spread of diseases?
Cancer screening does not prevent the spread of the disease. It makes early treatment more likely.
Example 9: Which of these is a non-specific defence against disease?
Skin is a non-specific defence against infection.
Example 10: Which of these do lymphocytes not produce?
Lymphocytes do not produce antigens. Antibodies are produced by lymphocytes after exposure to a pathogen.






