NEET PG Exam > NEET PG Notes > Medicine > CheatSheet: Disorders of Kidney
CheatSheet: Disorders of Kidney
1. Glomerular Diseases
1.1 Classification
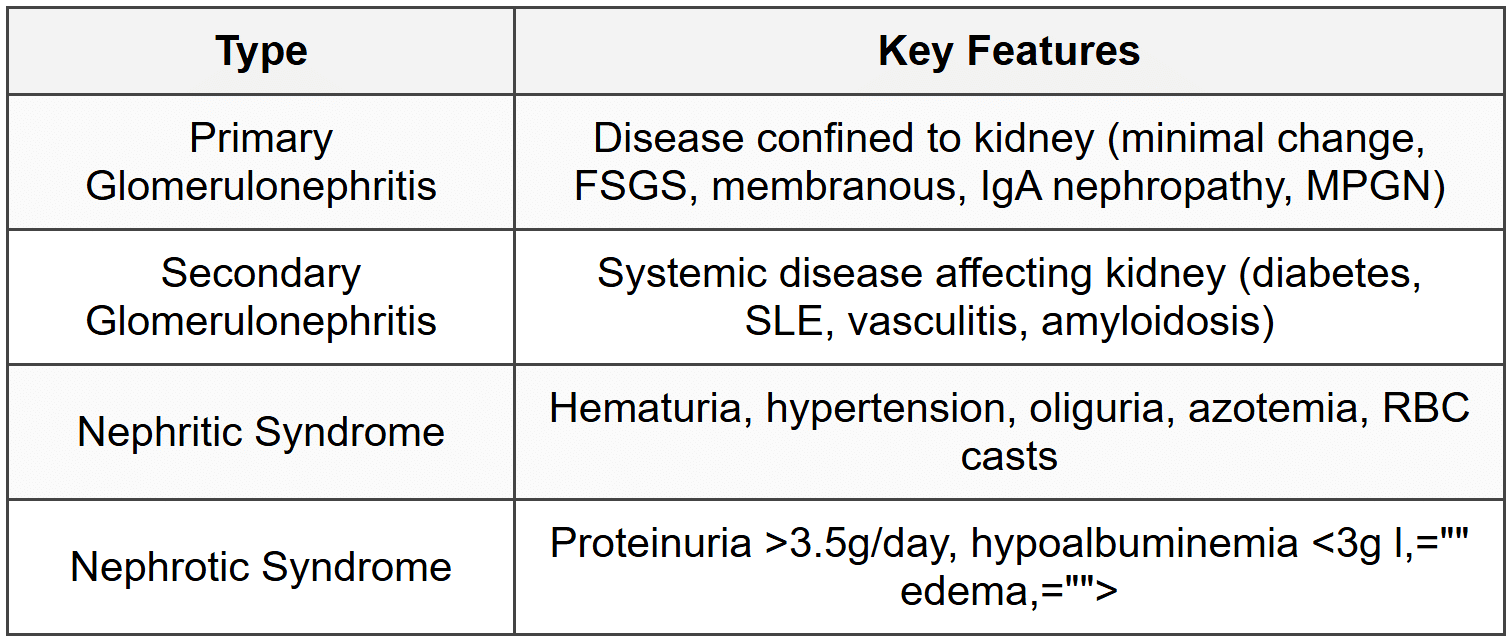
1.2 Minimal Change Disease
- Most common cause of nephrotic syndrome in children (90%)
- Selective proteinuria (albumin only), normal GFR, no hematuria
- Light microscopy: normal glomeruli; EM: podocyte foot process effacement
- Treatment: Corticosteroids - 90% response rate in children
- Associated with Hodgkin lymphoma, NSAIDs
1.3 Focal Segmental Glomerulosclerosis (FSGS)
- Most common primary glomerular disease in adults causing nephrotic syndrome
- Non-selective proteinuria, hematuria, hypertension, progressive renal failure
- Light microscopy: focal and segmental sclerosis; EM: foot process effacement
- Poor response to steroids (20-30%); 50% progress to ESRD in 10 years
- Secondary causes: HIV, heroin, obesity, reflux nephropathy, sickle cell disease
1.4 Membranous Nephropathy
- Most common primary cause of nephrotic syndrome in Caucasian adults
- Anti-PLA2R antibodies in 70% primary cases
- Light microscopy: thickened GBM; IF: granular IgG and C3; EM: subepithelial deposits with spike and dome
- Secondary causes: SLE, hepatitis B, malignancy, NSAIDs, penicillamine
- Rule of thirds: 1/3 remit, 1/3 persistent proteinuria, 1/3 progress to ESRD
- Treatment: ACEi/ARB; immunosuppression if high risk (Cyclophosphamide + steroids or Tacrolimus)
1.5 IgA Nephropathy (Berger Disease)
- Most common primary glomerulonephritis worldwide
- Recurrent gross hematuria within 1-2 days of URTI (synpharyngitic hematuria)
- Mesangial IgA deposition on immunofluorescence
- Henoch-Schonlein Purpura is systemic form with purpura, arthritis, abdominal pain
- Treatment: ACEi/ARB; steroids if proteinuria >1g/day; fish oil
- 25-30% progress to ESRD in 20 years
1.6 Membranoproliferative Glomerulonephritis (MPGN)

- Tram-track appearance on silver stain; mesangial proliferation
- Mixed nephritic-nephrotic presentation
1.7 Post-Infectious Glomerulonephritis
- Follows group A beta-hemolytic Streptococcus infection (pharyngitis/impetigo) by 1-3 weeks
- Acute nephritic syndrome: hematuria, cola-colored urine, hypertension, edema, oliguria
- Low C3, elevated ASO and anti-DNase B titers
- Light microscopy: diffuse proliferative GN; IF: granular IgG and C3 (starry sky); EM: subepithelial humps
- Self-limited in children (>95% recover); worse prognosis in adults
- Treatment: supportive (salt restriction, diuretics, antihypertensives)
1.8 Rapidly Progressive Glomerulonephritis (RPGN)

- Hallmark: crescentic GN on biopsy (>50% glomeruli with crescents)
- Rapid decline in GFR over days to weeks; oliguria, hematuria, RBC casts
- Treatment: pulse methylprednisolone + cyclophosphamide; plasmapheresis for anti-GBM disease
1.9 Alport Syndrome
- X-linked dominant mutation in COL4A5 gene (type IV collagen)
- Hematuria, progressive renal failure, sensorineural deafness, ocular abnormalities (lenticonus)
- EM: GBM splitting (basket-weave appearance)
- Males more severely affected; ESRD by 20-30 years
1.10 Thin Basement Membrane Disease
- Benign familial hematuria; autosomal dominant
- Persistent microscopic hematuria, no proteinuria, normal renal function
- EM: diffusely thin GBM (<250>
- Excellent prognosis; no treatment required
2. Tubular and Interstitial Diseases
2.1 Acute Tubular Necrosis (ATN)
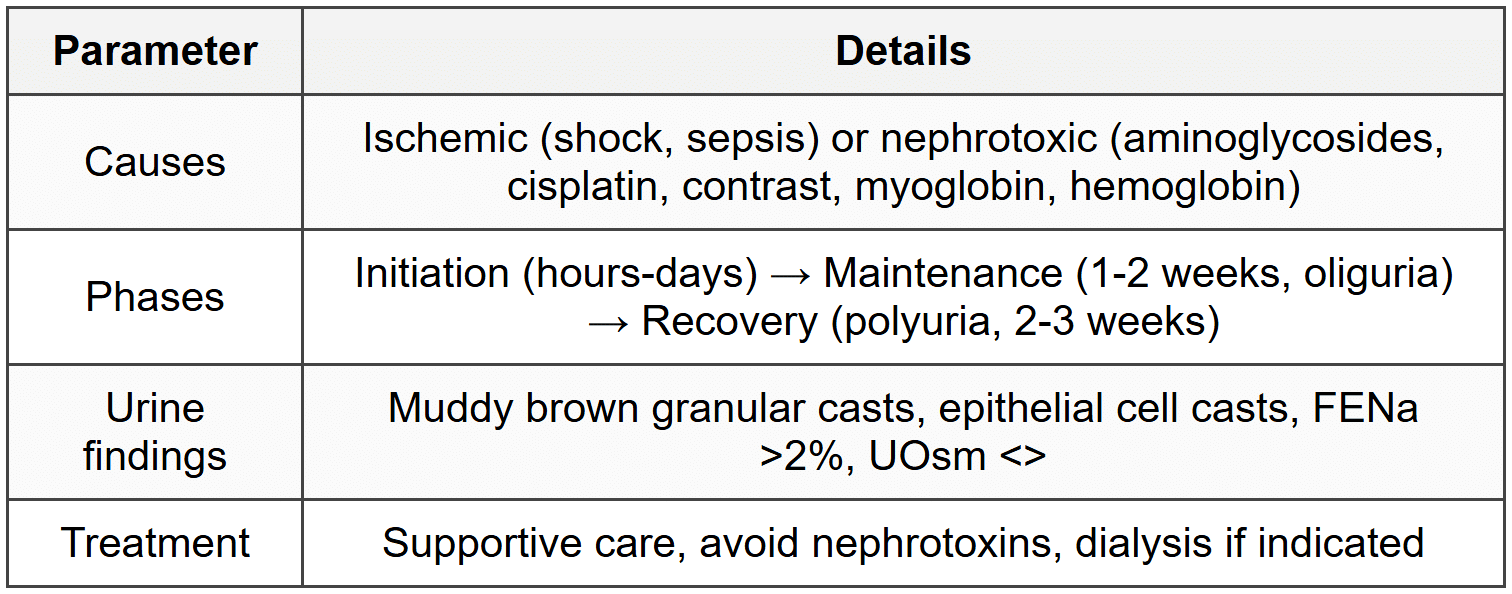
2.2 Acute Interstitial Nephritis (AIN)
- Causes: drugs (beta-lactams, NSAIDs, PPIs, 5-ASA, allopurinol), infections, autoimmune
- Classic triad: fever, rash, eosinophilia (in <10%>
- Urine: eosinophiluria, WBC casts, sterile pyuria, mild proteinuria
- NSAIDs cause AIN with nephrotic-range proteinuria (minimal change disease)
- Biopsy: interstitial inflammation with eosinophils and lymphocytes
- Treatment: stop offending drug, steroids if severe
2.3 Chronic Interstitial Nephritis
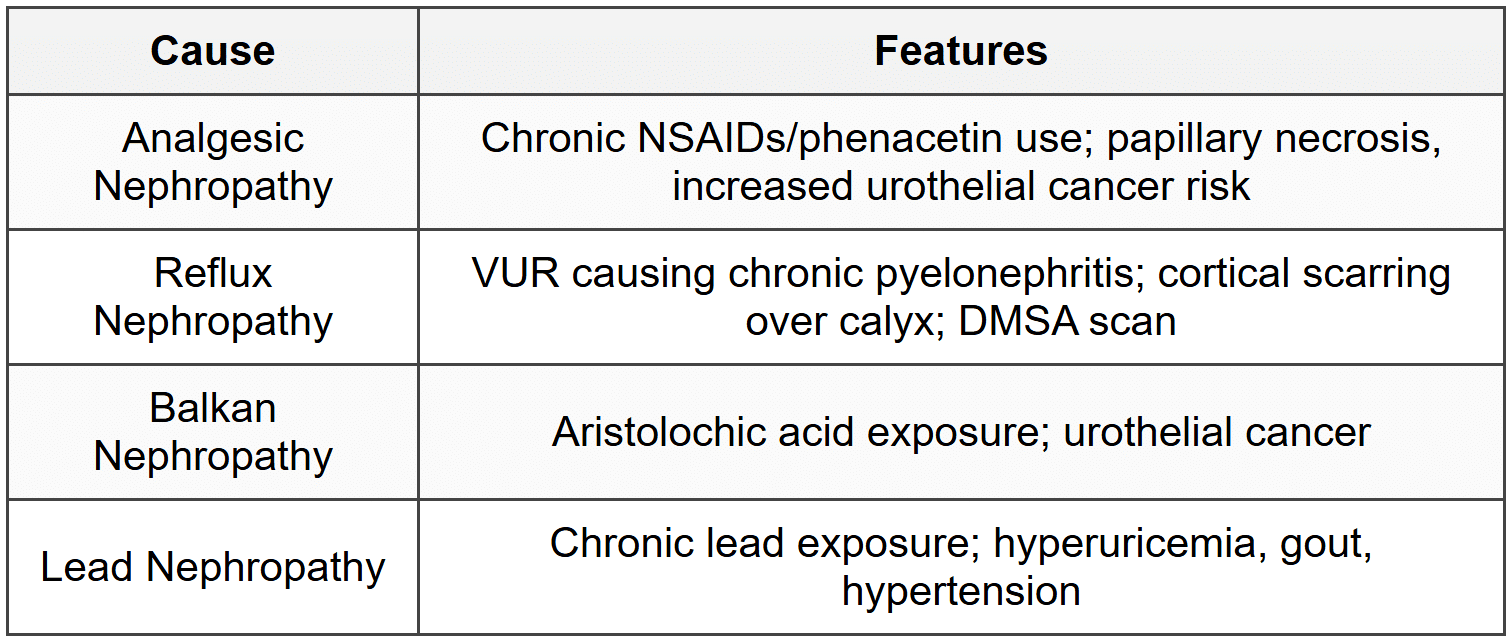
2.4 Renal Tubular Acidosis (RTA)
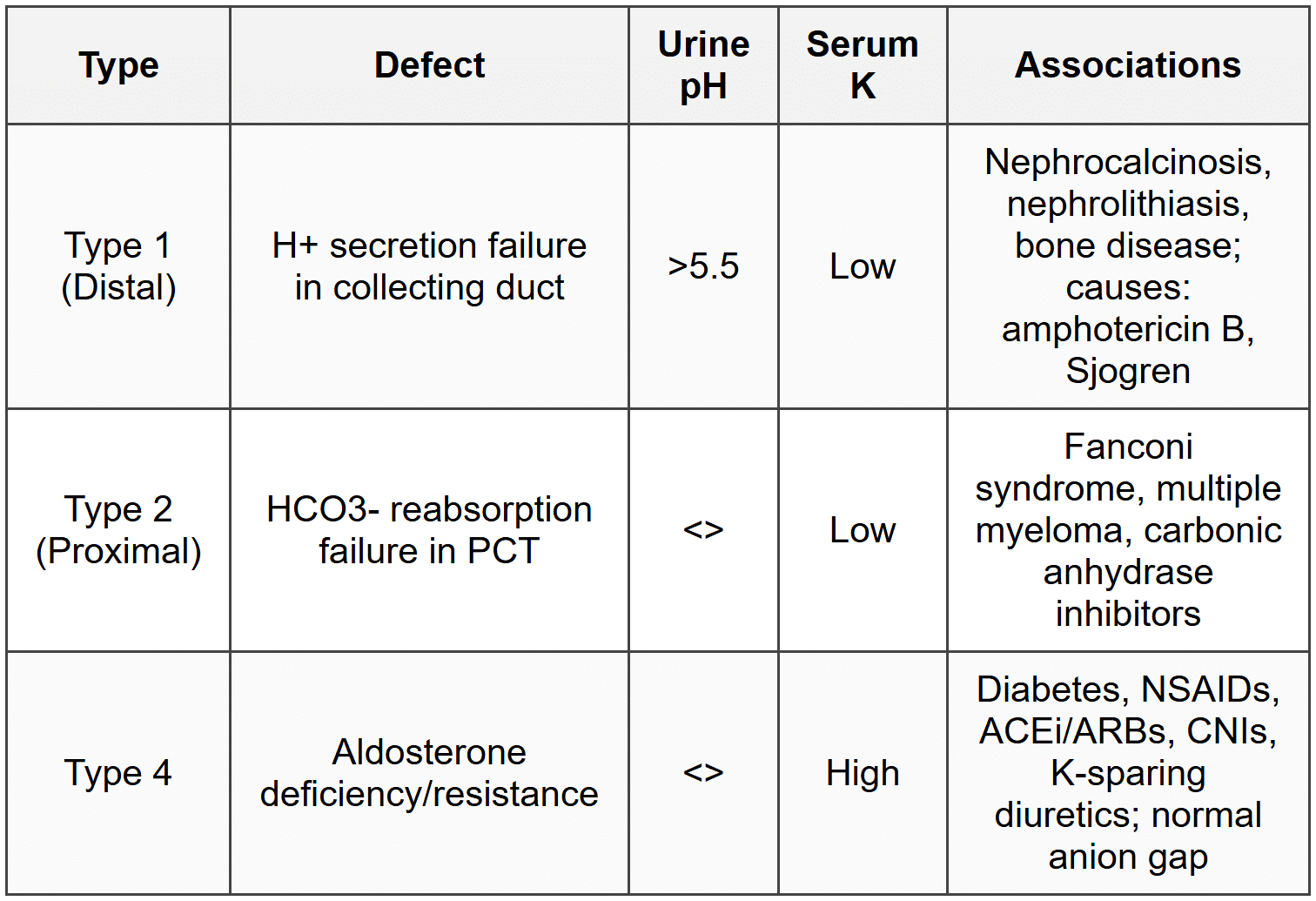

2.5 Fanconi Syndrome
- Generalized PCT dysfunction: aminoaciduria, glycosuria, phosphaturia, bicarbonaturia, uricosuria
- Causes: cystinosis (most common in children), multiple myeloma (adults), ifosfamide, tenofovir
- Rickets/osteomalacia due to phosphate wasting
- Type 2 RTA with hypokalemia
2.6 Bartter and Gitelman Syndromes
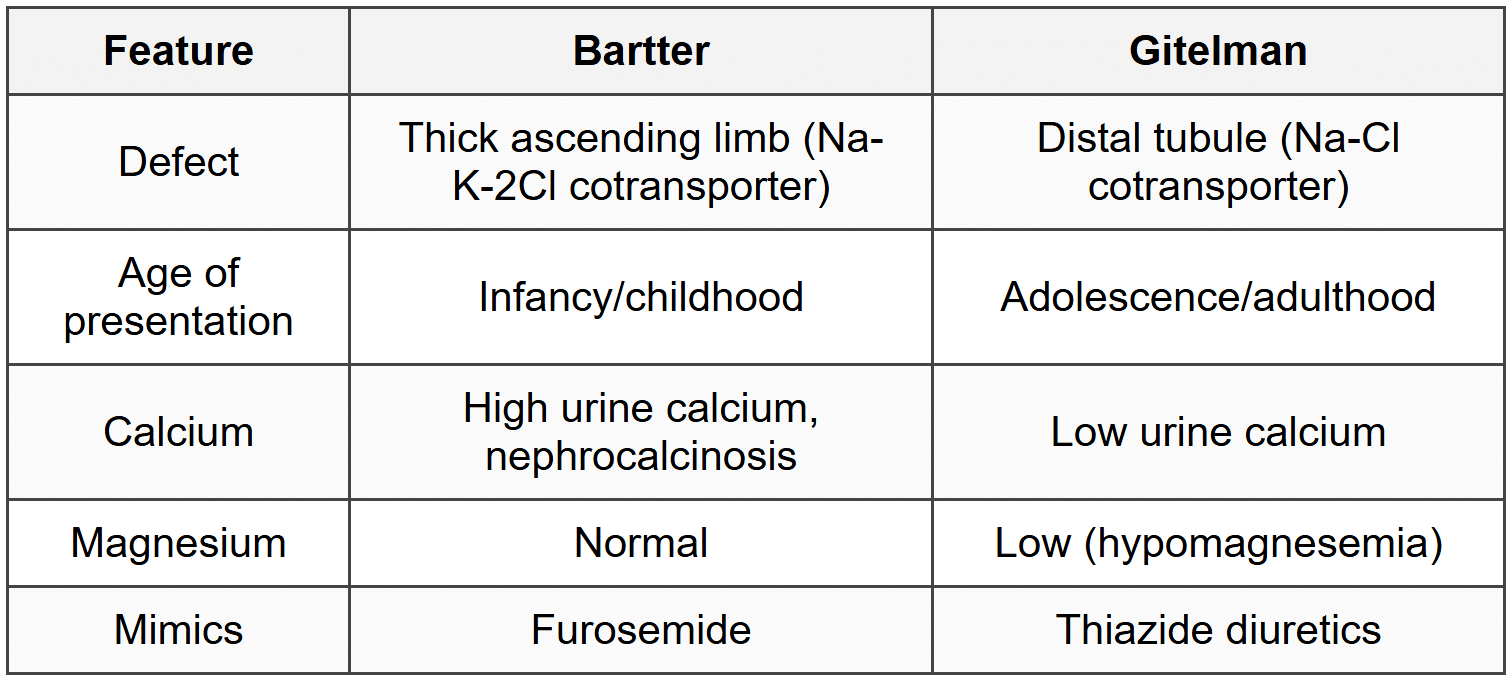
- Both: hypokalemic metabolic alkalosis, hyperreninemia, hyperaldosteronism, normal BP
3. Acute Kidney Injury (AKI)
3.1 Definition and Staging (KDIGO)

3.2 Classification
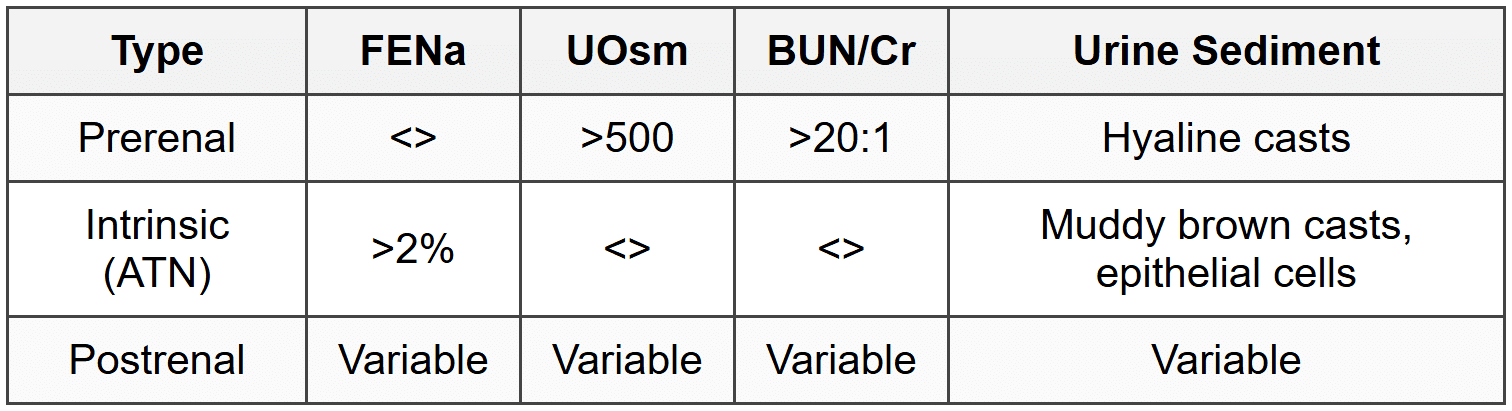
3.3 Prerenal AKI
- Causes: volume depletion (bleeding, GI losses, burns), decreased effective circulating volume (CHF, cirrhosis), renal vasoconstriction (NSAIDs, ACEi/ARBs, HRS)
- Rapidly reversible with volume resuscitation
- If prolonged, progresses to ATN (intrinsic renal failure)
3.4 Intrinsic AKI
- ATN: ischemic or nephrotoxic (see section 2.1)
- Acute interstitial nephritis (see section 2.2)
- Glomerulonephritis: RPGN (see section 1.8)
- Vascular: renal artery thrombosis/stenosis, renal vein thrombosis, atheroembolic disease, TTP/HUS, malignant hypertension
3.5 Postrenal AKI
- Bilateral ureteric obstruction or unilateral in single functioning kidney
- Causes: BPH, prostate cancer, cervical cancer, retroperitoneal fibrosis, bilateral stones, neurogenic bladder
- Diagnosis: ultrasound showing hydronephrosis (may be absent in early obstruction or retroperitoneal fibrosis)
- Treatment: relieve obstruction (catheterization, nephrostomy); watch for post-obstructive diuresis
3.6 Contrast-Induced Nephropathy (CIN)
- Rise in creatinine ≥0.5 mg/dL or ≥25% from baseline within 48-72 hours of contrast
- Risk factors: pre-existing CKD, diabetes, volume depletion, CHF, age >75, contrast volume
- Prevention: IV isotonic saline hydration, minimize contrast volume, hold NSAIDs/diuretics, NAC (controversial)
- Avoid metformin (lactic acidosis risk); restart after 48 hours if renal function stable
3.7 Rhabdomyolysis
- Causes: trauma, prolonged immobilization, seizures, drugs (statins, cocaine), heat stroke, malignant hyperthermia
- Myoglobin causes ATN; serum CK >5000 U/L, hyperkalemia, hyperphosphatemia, hypocalcemia (early), hyperuricemia
- Urine: dipstick positive for blood but no RBCs on microscopy (detects myoglobin)
- Treatment: aggressive IV fluids (200-300 mL/hr), urine alkalinization (sodium bicarbonate), monitor for compartment syndrome
3.8 Tumor Lysis Syndrome
- Massive cell lysis after chemotherapy: hyperkalemia, hyperphosphatemia, hypocalcemia, hyperuricemia
- AKI from uric acid and calcium phosphate precipitation in tubules
- Prevention: allopurinol or rasburicase (preferred if high risk), aggressive hydration, avoid loop diuretics
- Treatment: rasburicase, dialysis if refractory
4. Chronic Kidney Disease (CKD)
4.1 Definition and Staging
- CKD: GFR <60 ml/min/1.73m²="" or="" kidney="" damage="" for="" ≥3="">
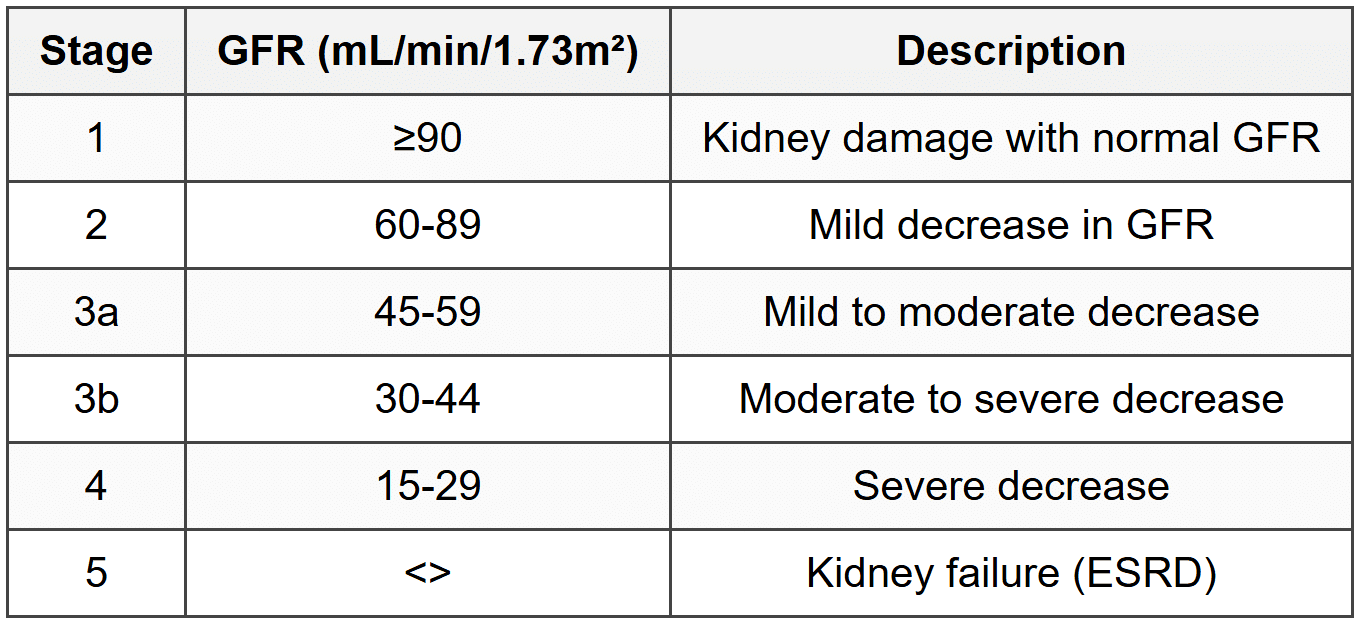
4.2 Common Causes
- Diabetes mellitus (40%): most common cause
- Hypertension (25-30%)
- Glomerulonephritis (10-15%)
- Polycystic kidney disease
- Chronic interstitial nephritis
4.3 Clinical Features

4.4 CKD-Mineral Bone Disease
- Decreased phosphate excretion → hyperphosphatemia
- Decreased calcitriol production → hypocalcemia
- Secondary hyperparathyroidism → renal osteodystrophy
- Target PTH: 2-9 times upper limit of normal in ESRD
- Treatment: phosphate binders (calcium carbonate, sevelamer), calcitriol, calcimimetics (cinacalcet)
- Adynamic bone disease: oversuppression of PTH
4.5 Management
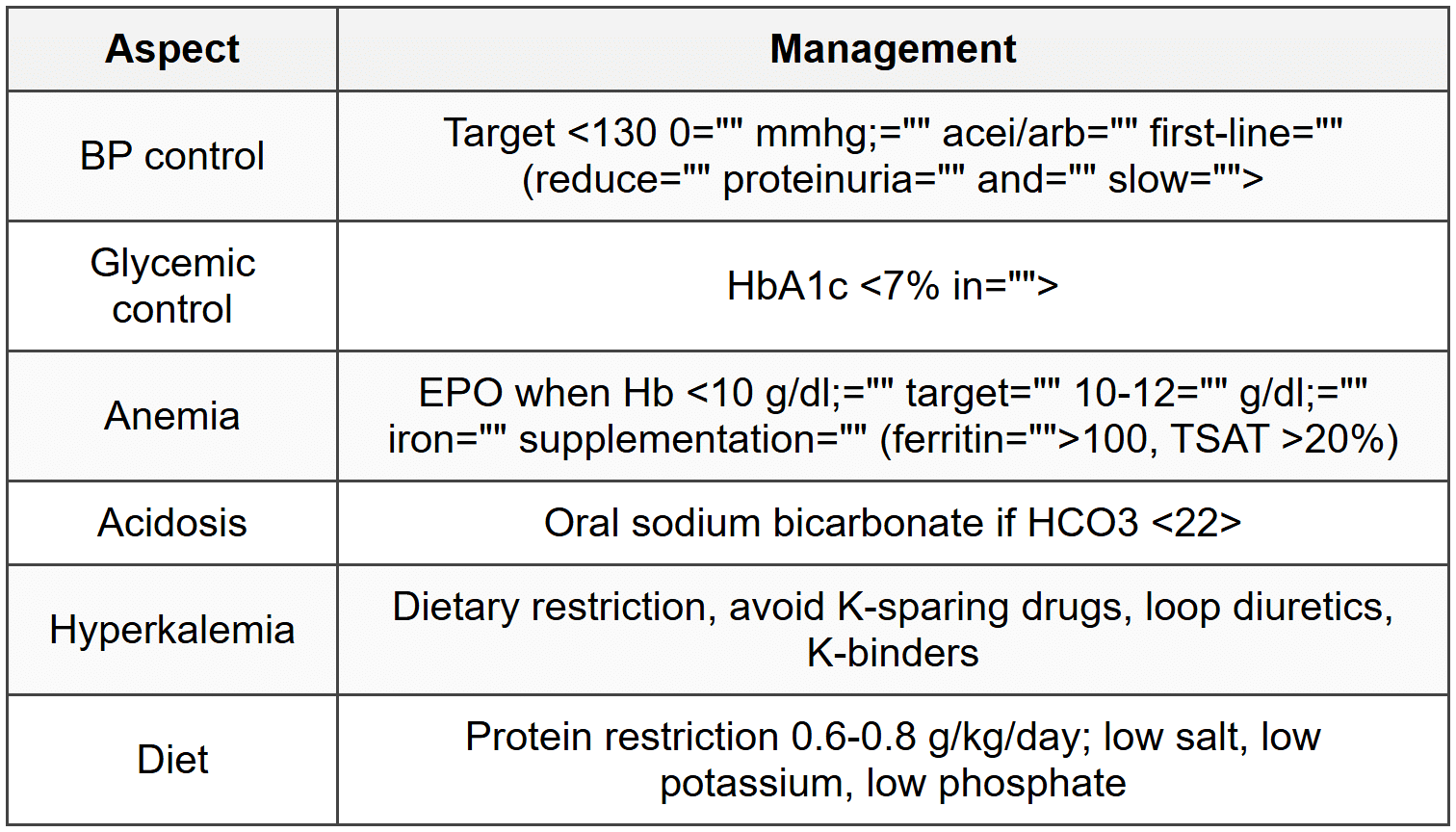

4.6 Indications for Dialysis (AEIOU)
- A: Acidosis (refractory metabolic acidosis)
- E: Electrolyte abnormalities (hyperkalemia refractory to medical therapy)
- I: Intoxications (methanol, ethylene glycol, lithium, salicylates)
- O: Fluid overload (refractory to diuretics)
- U: Uremia (pericarditis, encephalopathy, bleeding)
- GFR <15 ml/min="" with="" symptoms="" or="" gfr=""><10>
4.7 Uremic Pericarditis
- Indication for urgent dialysis
- Pericardial friction rub, chest pain, ECG changes
- Risk of hemorrhagic pericardial effusion and tamponade
- Does not respond to NSAIDs (contraindicated in CKD)
5. Cystic Kidney Diseases
5.1 Autosomal Dominant Polycystic Kidney Disease (ADPKD)
- Most common inherited cause of ESRD (10% of ESRD cases)
- PKD1 (85%, chromosome 16, worse prognosis) and PKD2 (15%, chromosome 4)
- Bilateral renal cysts, enlarged kidneys, flank pain, hematuria, hypertension
- Extrarenal: hepatic cysts (most common), cerebral berry aneurysms (5-10%), mitral valve prolapse, colonic diverticula
- Screening: MRI brain for aneurysm if family history of SAH or high-risk occupation
- Treatment: BP control (ACEi/ARB), tolvaptan slows cyst growth and GFR decline
- ESRD by 50-60 years
5.2 Autosomal Recessive Polycystic Kidney Disease (ARPKD)
- PKHD1 gene mutation; presents in infancy/childhood
- Bilateral enlarged cystic kidneys, Potter sequence (oligohydramnios → pulmonary hypoplasia, limb deformities)
- Congenital hepatic fibrosis → portal hypertension, varices, splenomegaly
- Poor prognosis; many die in neonatal period
5.3 Medullary Cystic Kidney Disease
- Autosomal dominant; cysts at corticomedullary junction
- Polyuria, salt wasting, progressive renal failure
- Small kidneys (unlike ADPKD)
5.4 Medullary Sponge Kidney
- Benign condition; dilated collecting ducts in medulla
- Nephrolithiasis (calcium stones), hematuria, UTI, nephrocalcinosis
- Normal renal function; IVP shows contrast-filled cystic spaces (bouquet of flowers)
5.5 Simple Renal Cysts
- Very common; increase with age; no clinical significance
- Bosniak classification for characterizing cysts on CT
- Bosniak I-II: benign; Bosniak IIF: follow-up; Bosniak III-IV: surgical exploration (malignancy risk)
6. Vascular Disorders
6.1 Renal Artery Stenosis (RAS)
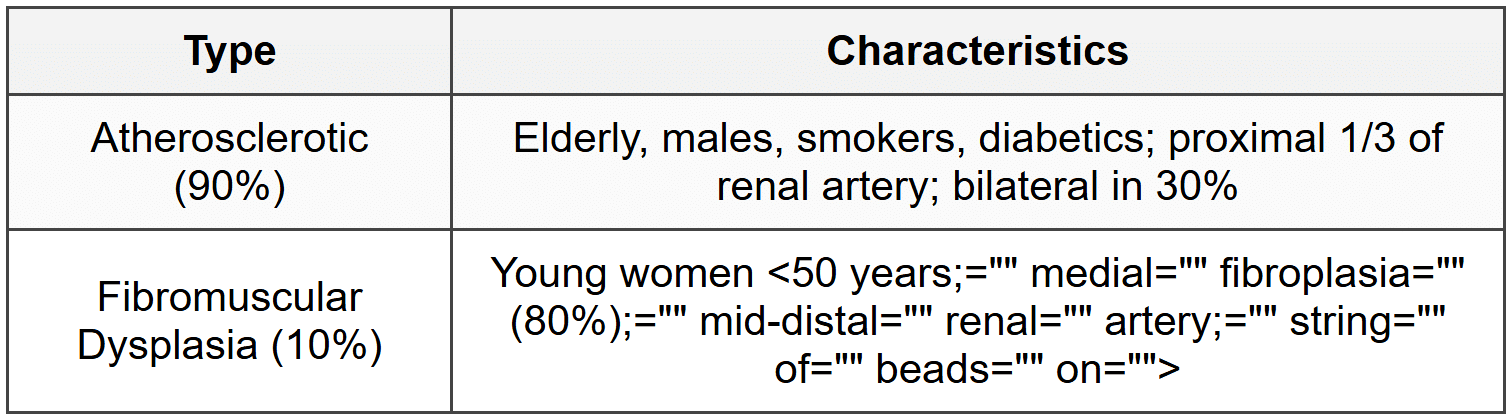
- Clinical clues: resistant hypertension, abdominal bruit, flash pulmonary edema, rise in creatinine >30% after ACEi/ARB
- Diagnosis: Doppler ultrasound (screening), CT/MR angiography, gold standard is renal arteriography
- Captopril renography (decreased use now)
- Treatment: ACEi/ARB for medical therapy; angioplasty for FMD (high cure rate); stenting for atherosclerotic (limited benefit)
6.2 Renal Vein Thrombosis
- Causes: nephrotic syndrome (membranous nephropathy, especially), hypercoagulable states, trauma, malignancy
- Acute: flank pain, hematuria, AKI, left testicular swelling (left-sided)
- Chronic: asymptomatic or worsening proteinuria
- Diagnosis: CT/MR venography, Doppler ultrasound
- Treatment: anticoagulation
6.3 Atheroembolic Disease
- Cholesterol emboli to kidneys after vascular procedure or spontaneous in severe atherosclerosis
- Subacute renal failure (days to weeks post-procedure), eosinophilia, eosinophiluria, hypocomplementemia
- Extrarenal: livedo reticularis, blue toe syndrome, GI ischemia, stroke
- Biopsy: cholesterol clefts in arterioles
- No specific treatment; supportive care; poor prognosis
6.4 Renal Infarction
- Causes: atrial fibrillation (embolic), endocarditis, atherosclerosis, trauma, vasculitis
- Sudden flank pain, nausea, fever, hematuria, elevated LDH
- CT with contrast: wedge-shaped perfusion defect
- Treatment: anticoagulation if embolic; thrombolysis if early presentation
6.5 Malignant Hypertension
- BP >180/120 mmHg with acute end-organ damage (retinopathy, AKI, encephalopathy, cardiac)
- Renal: AKI, hematuria, proteinuria, RBC casts
- Biopsy: acute tubular necrosis, fibrinoid necrosis of arterioles
- Treatment: gradual BP reduction over 24-48 hours; IV labetalol, nicardipine, nitroprusside (avoid in renal failure)
6.6 Scleroderma Renal Crisis
- Acute renal failure with malignant hypertension in systemic sclerosis (diffuse cutaneous)
- Microangiopathic hemolytic anemia, thrombocytopenia
- Risk: anti-RNA polymerase III antibodies, early diffuse skin involvement, corticosteroids
- Treatment: ACEi (captopril) started immediately; dialysis if needed (some recover renal function)
7. Thrombotic Microangiopathies
7.1 Hemolytic Uremic Syndrome (HUS)

- Classic triad: microangiopathic hemolytic anemia (schistocytes), thrombocytopenia, AKI
- Normal coagulation profile (PT, aPTT), elevated LDH, low haptoglobin, negative Coombs
- Renal manifestations predominate (unlike TTP)
7.2 Thrombotic Thrombocytopenic Purpura (TTP)
- ADAMTS13 deficiency (cleaves vWF); congenital or acquired (autoantibodies)
- Pentad: microangiopathic hemolytic anemia, thrombocytopenia, AKI, neurologic symptoms, fever
- Neurologic manifestations predominate (headache, confusion, seizures, stroke)
- ADAMTS13 activity <>
- Treatment: plasma exchange (first-line), rituximab, caplacizumab (anti-vWF); avoid platelet transfusion
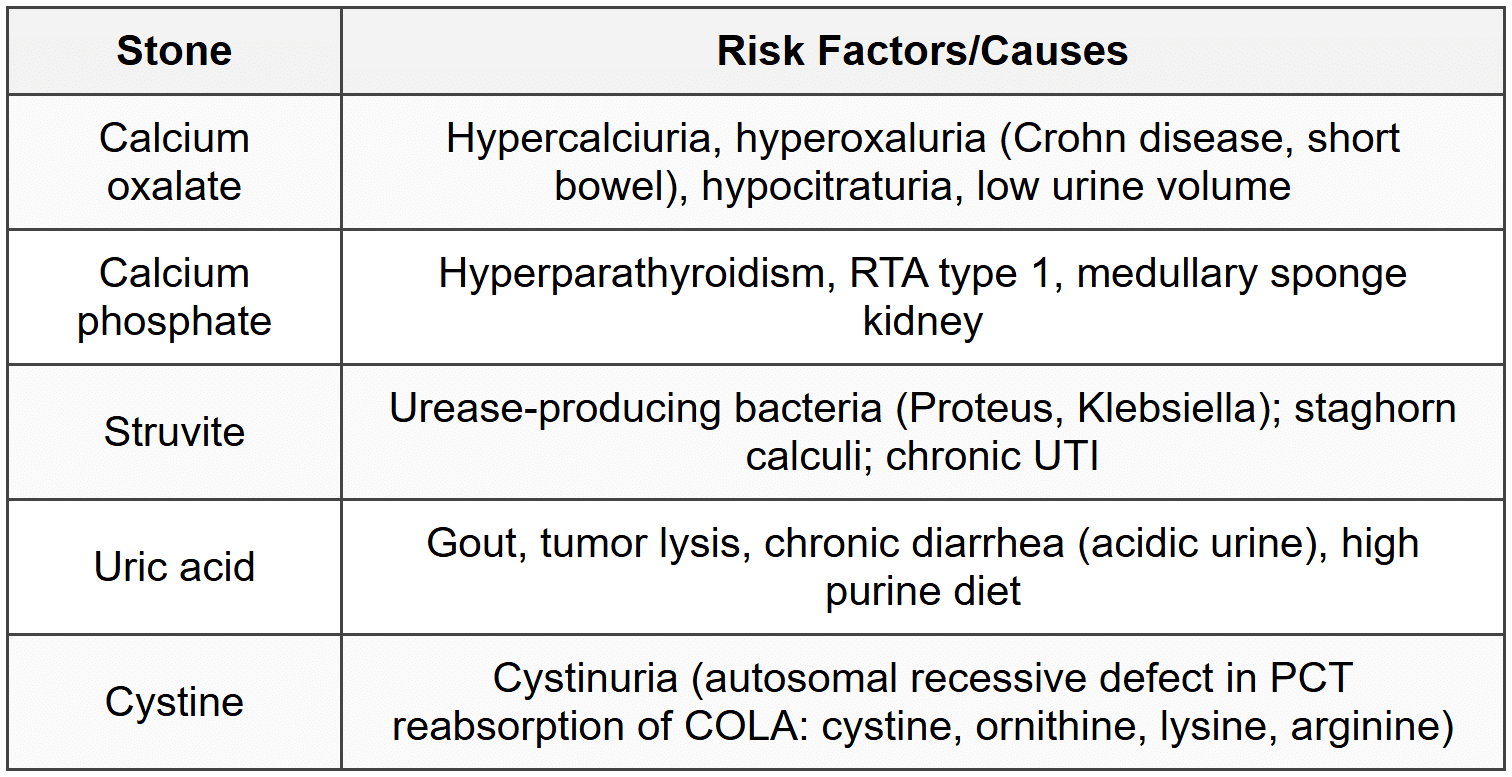
8. Nephrolithiasis
8.1 Stone Types
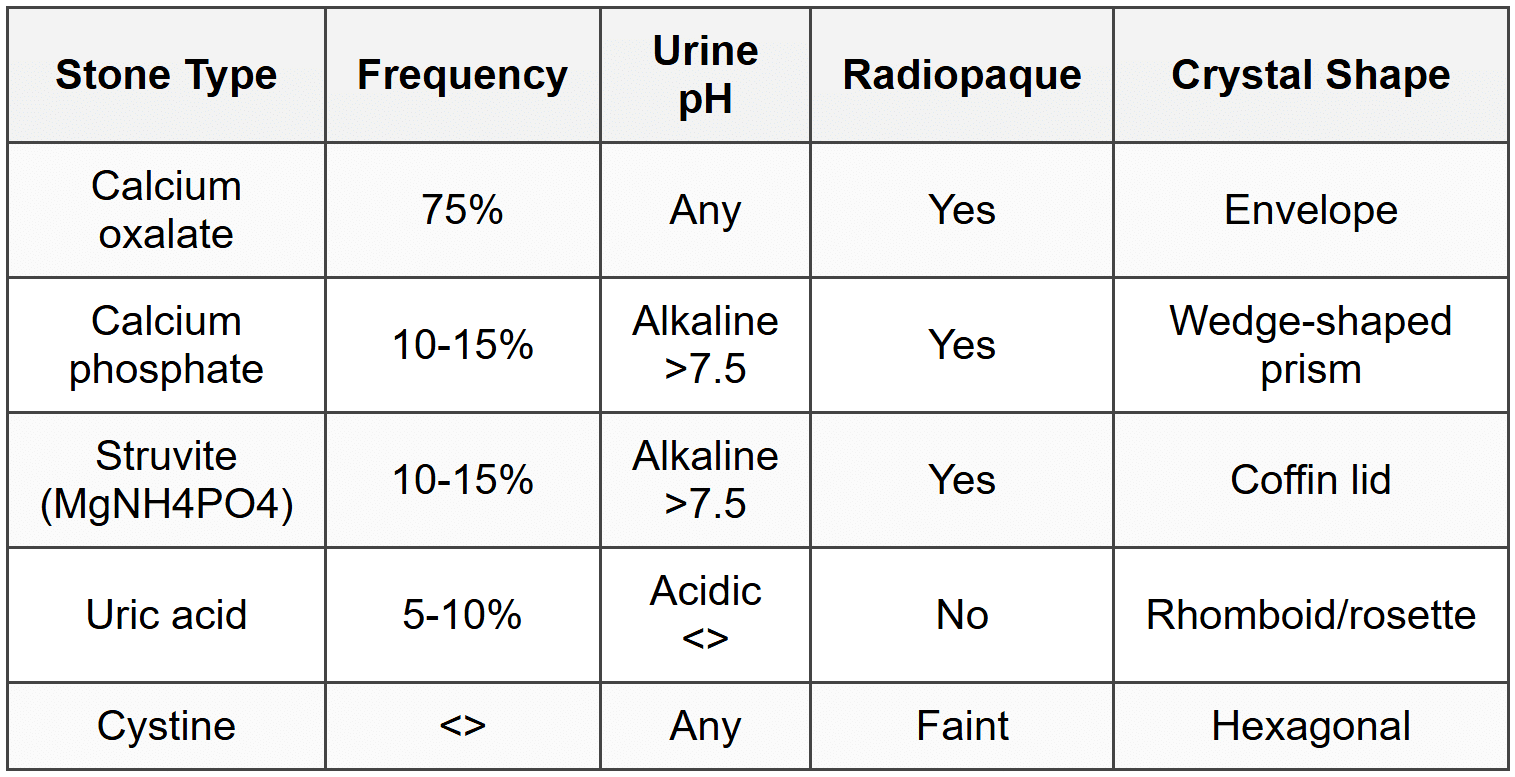
8.2 Risk Factors and Causes
8.3 Clinical Presentation
- Acute renal colic: sudden severe flank pain radiating to groin, nausea, vomiting, restlessness
- Hematuria (90% cases), UTI, hydronephrosis, AKI (if bilateral obstruction)
- Diagnosis: non-contrast CT KUB (gold standard); ultrasound in pregnancy
8.4 Management
- Acute: NSAIDs for pain, hydration, medical expulsive therapy (tamsulosin) for stones 5-10 mm
- Indications for intervention: stone >10 mm, obstruction with infection (emergency), intractable pain, AKI
- Procedures: ESWL (stones <20 mm),="" ureteroscopy,="" pcnl="" (large/staghorn="">
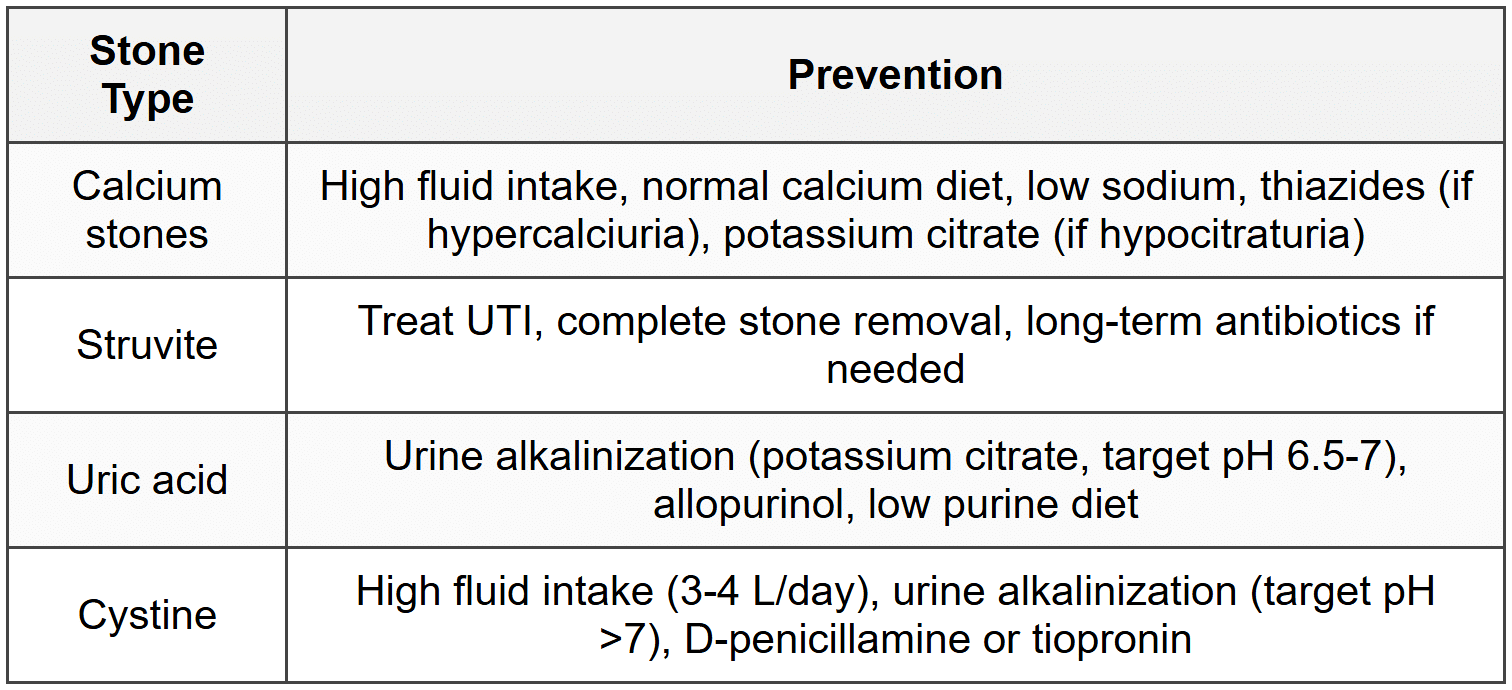
8.5 Prevention
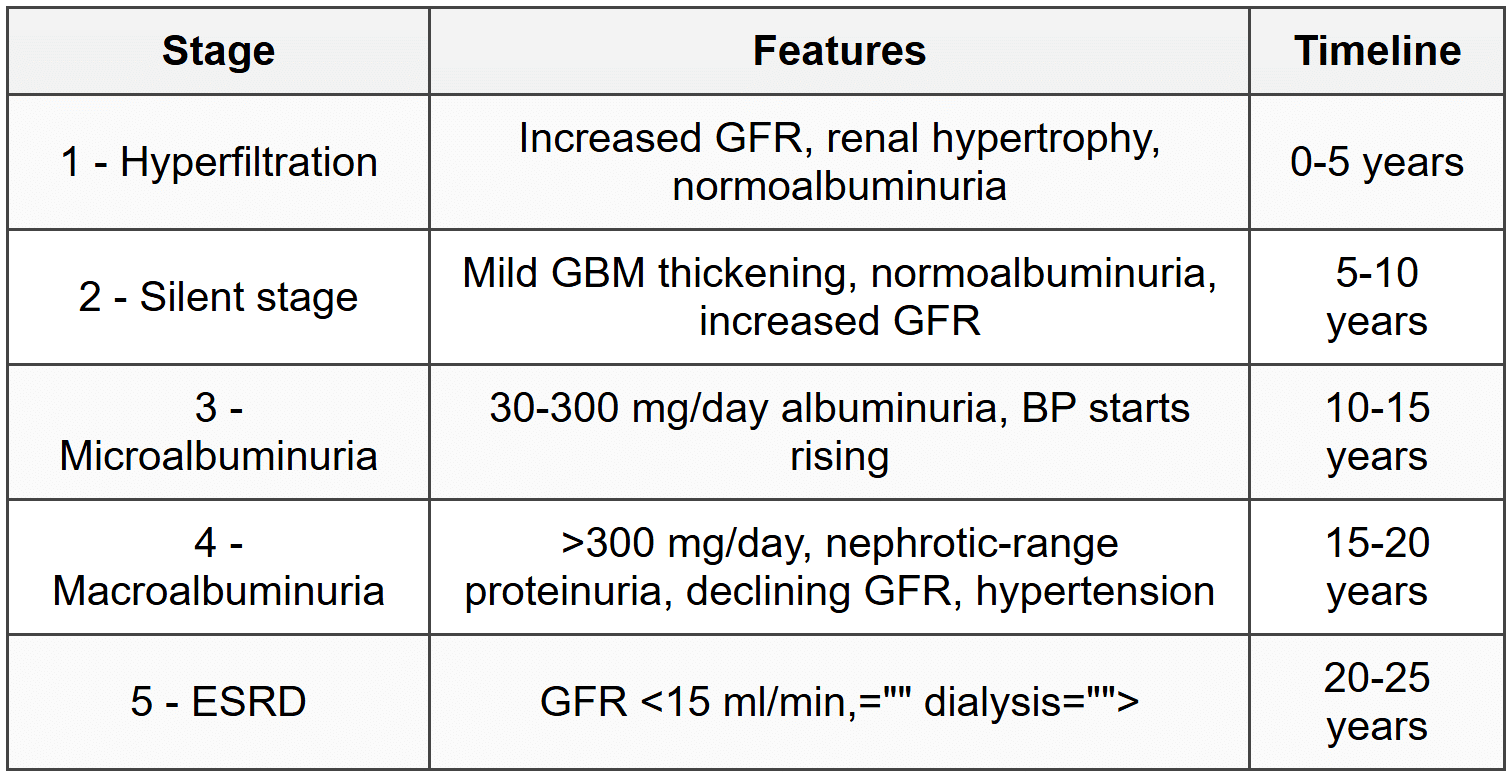
9. Diabetic Nephropathy
9.1 Stages
9.2 Pathology
- Kimmelstiel-Wilson nodules: nodular glomerulosclerosis (pathognomonic)
- Diffuse glomerulosclerosis (more common)
- GBM thickening, mesangial expansion, arteriolar hyalinosis
- IF and EM: linear IgG and albumin along GBM
9.3 Clinical Features
- Albuminuria precedes decline in GFR
- Non-nephrotic proteinuria initially, progresses to nephrotic syndrome
- Retinopathy present in >90% cases (if absent, consider other causes)
- Hypertension, accelerated CVD
9.4 Management
- Glycemic control: HbA1c <7%; intensive="" control="" prevents="" onset="" but="" limited="" benefit="" once="">
- BP control: target <130 0;="" acei="" or="" arb="" (first-line,="" antiproteinuric,="">
- SGLT2 inhibitors: reduce albuminuria, slow GFR decline, reduce CV events (canagliflozin, dapagliflozin, empagliflozin)
- GLP-1 agonists: reduce albuminuria and CV events (liraglutide, semaglutide)
- Finerenone (non-steroidal MRA): reduces CKD progression and CV events
- Protein restriction: 0.8 g/kg/day
- Lipid control: statin therapy
10. Hypertensive Nephropathy
10.1 Pathophysiology
- Chronic hypertension → renal arteriosclerosis → ischemic injury → nephrosclerosis
- Benign nephrosclerosis: gradual decline in GFR, mild proteinuria (<1>
- Accelerated by diabetes, smoking, hyperlipidemia
10.2 Pathology
- Arteriolosclerosis: hyaline arteriolosclerosis (benign hypertension), hyperplastic arteriolosclerosis (malignant hypertension)
- Glomerulosclerosis, tubular atrophy, interstitial fibrosis
- Granular contracted kidneys bilaterally
10.3 Clinical Features
- Long-standing hypertension, slowly progressive CKD
- Mild proteinuria, bland urine sediment, no RBC casts
- Left ventricular hypertrophy, retinopathy
10.4 Management
- BP target: <130 0="" mmhg="" in="">
- ACEi/ARB preferred if proteinuria present
- Multi-drug regimen often needed
11. Lupus Nephritis
11.1 ISN/RPS Classification
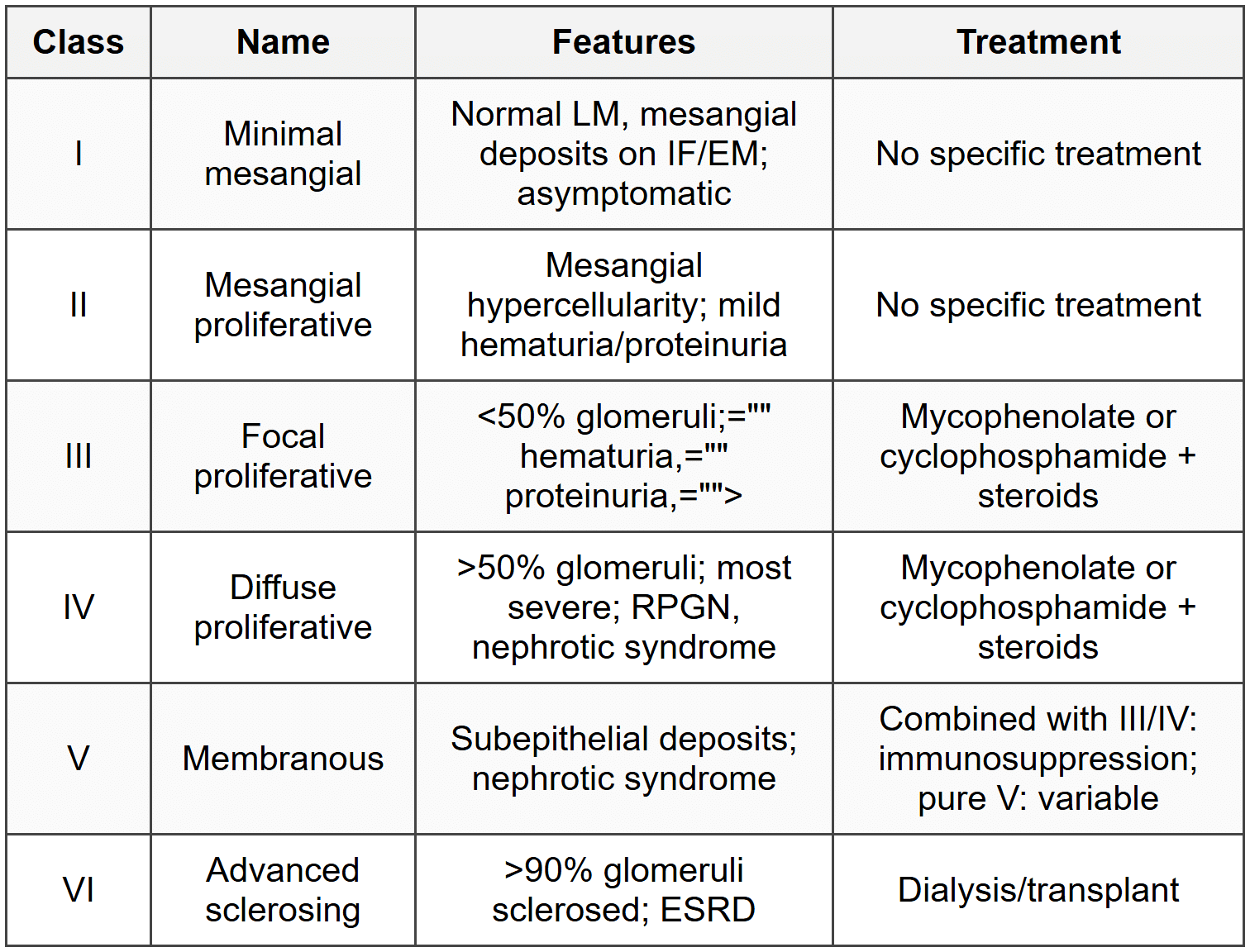
11.2 Diagnosis
- Renal biopsy required for classification and treatment planning
- IF: full house pattern (IgG, IgA, IgM, C3, C1q); C1q deposition highly specific
- Low C3 and C4 (consume both classical and alternative pathways)
- Anti-dsDNA antibodies correlate with disease activity
11.3 Clinical Features
- Hematuria, proteinuria (nephritic, nephrotic, or mixed), hypertension, renal insufficiency
- Extrarenal lupus manifestations
11.4 Treatment
- Induction (Class III/IV): mycophenolate mofetil or cyclophosphamide + high-dose steroids for 6 months
- Maintenance: mycophenolate or azathioprine + low-dose steroids
- Adjunct: hydroxychloroquine, ACEi/ARB
- Refractory: rituximab, belimumab, voclosporin
12. Renal Transplantation
12.1 Immunosuppression
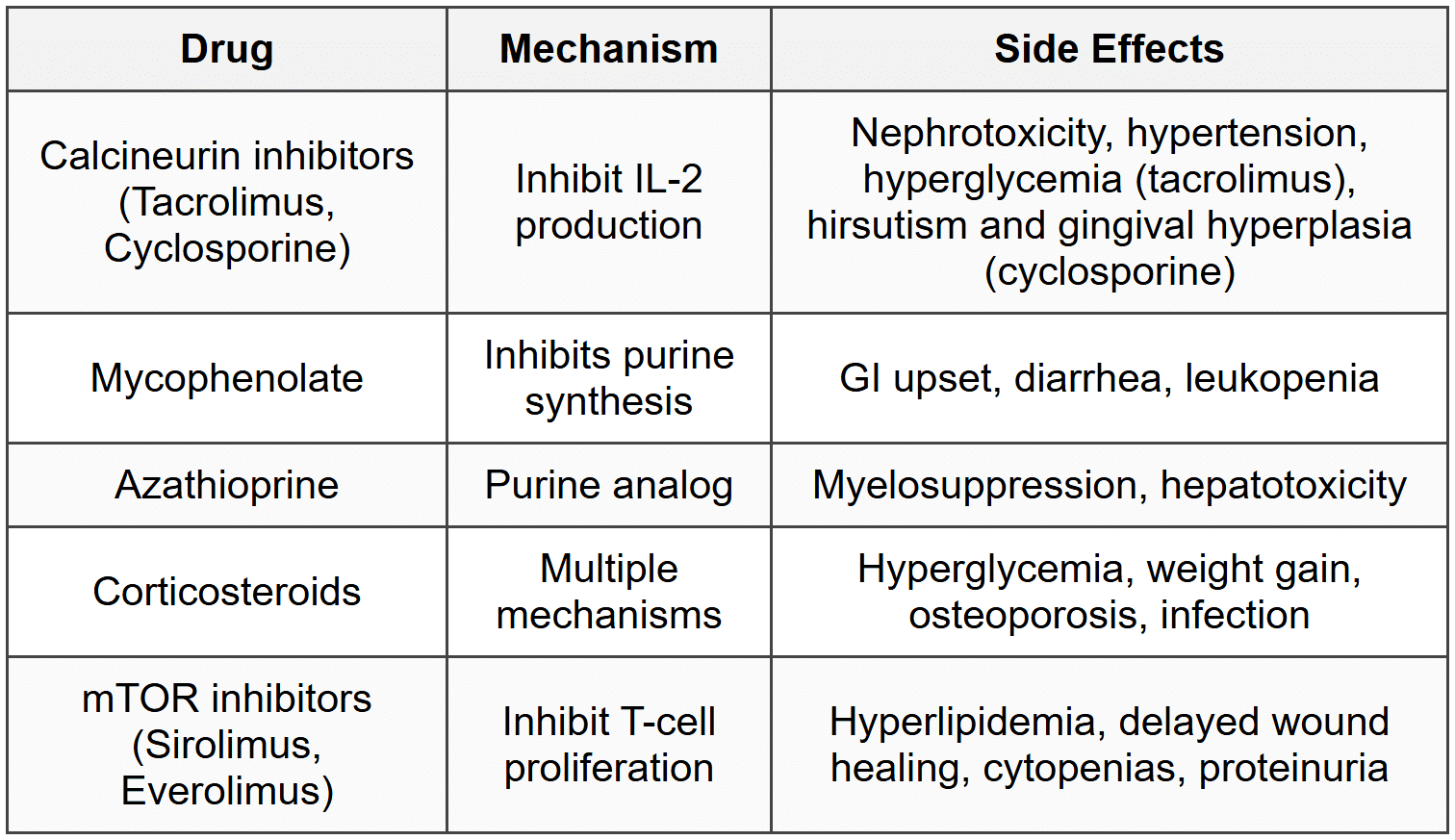
12.2 Rejection
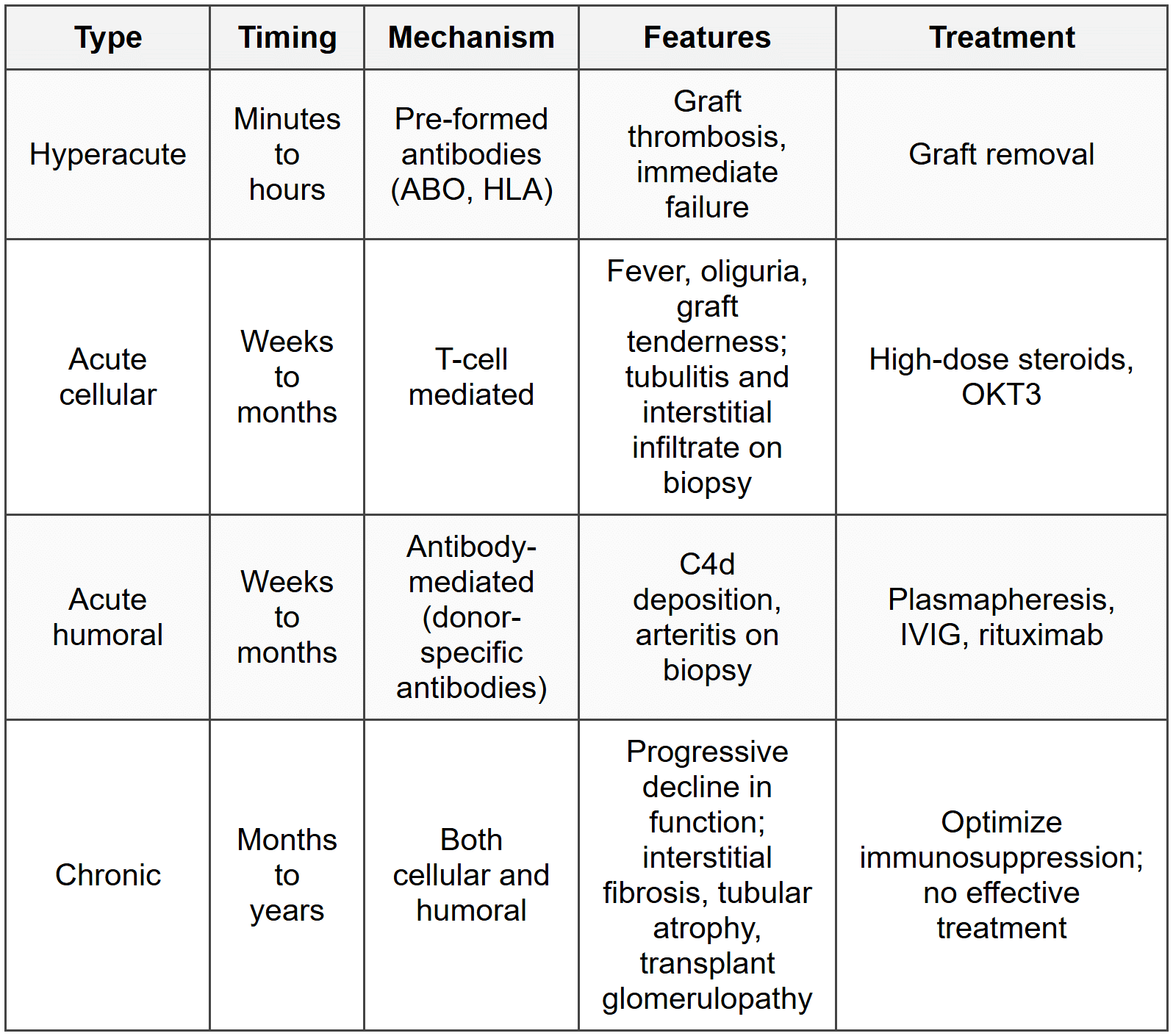
12.3 BK Virus Nephropathy
- Polyomavirus reactivation in immunosuppressed transplant recipients
- Progressive graft dysfunction; decoy cells in urine
- Diagnosis: BK viremia, viruria; biopsy shows tubular injury with viral inclusions
- Treatment: reduce immunosuppression; cidofovir or leflunomide in severe cases
12.4 Post-Transplant Complications
- Infections: CMV (most common 1-6 months), PCP, Nocardia, Aspergillus, BK virus
- Malignancy: PTLD (EBV-related), skin cancer (SCC > BCC), Kaposi sarcoma
- Recurrent disease: FSGS, IgA nephropathy, membranoproliferative GN, diabetic nephropathy
- New-onset diabetes after transplantation (NODAT): risk with tacrolimus, steroids
13. Acid-Base and Electrolyte Disorders
13.1 Hyperkalemia
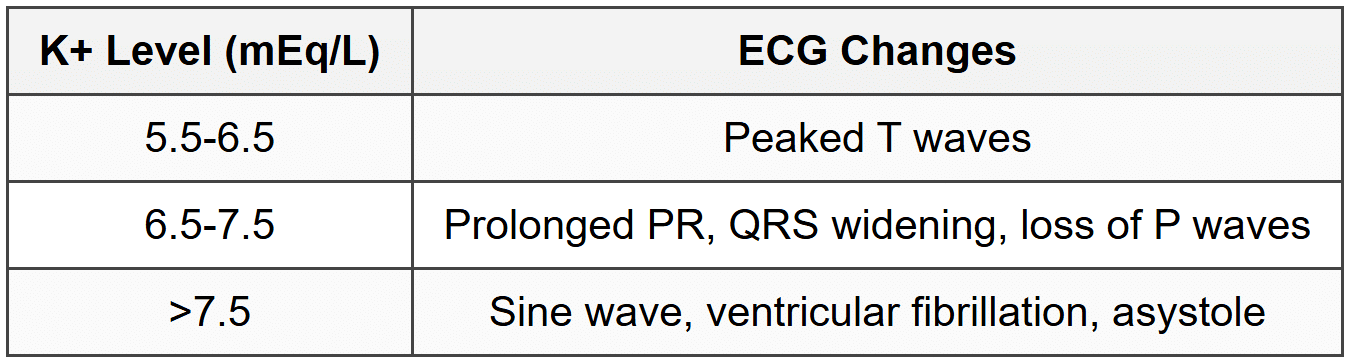

- Treatment: calcium gluconate (membrane stabilization), insulin + glucose (shift K into cells), beta-agonists, sodium bicarbonate (if acidotic), loop diuretics, K-binders (patiromer, sodium zirconium cyclosilicate), dialysis
13.2 Hypokalemia
- Causes: GI losses, renal losses (diuretics, RTA, hyperaldosteronism), intracellular shift
- ECG: U waves, flattened T waves, ST depression, prolonged QT
- Complications: muscle weakness, rhabdomyolysis, ileus, arrhythmias
- Treatment: potassium replacement (oral or IV); treat underlying cause
13.3 Hypernatremia
- Hypovolemic: dehydration, GI losses, osmotic diuresis
- Euvolemic: diabetes insipidus (central or nephrogenic), insensible losses
- Hypervolemic: hypertonic saline, hyperaldosteronism
- Treatment: correct slowly (<10-12 meq/l="" per="" 24="" hours)="" to="" avoid="" cerebral="" edema;="" use="" d5w="" or="" hypotonic="">
13.4 Hyponatremia
- Hypovolemic: GI losses, diuretics, renal losses; urine Na <20 (extrarenal)="" or="">20 (renal)
- Euvolemic: SIADH, hypothyroidism, adrenal insufficiency, psychogenic polydipsia
- Hypervolemic: CHF, cirrhosis, nephrotic syndrome; urine Na <>
- Treatment: treat underlying cause; hypertonic saline if severe/symptomatic; fluid restriction in SIADH; tolvaptan (V2 receptor antagonist)
- Correct slowly (<10-12 meq/l="" per="" 24="" hours)="" to="" avoid="" osmotic="" demyelination="">
13.5 Syndrome of Inappropriate ADH (SIADH)
- Euvolemic hypotonic hyponatremia with urine osmolality >100 mOsm/kg and urine Na >40 mEq/L
- Causes: CNS disorders, pulmonary disease (pneumonia, TB), malignancy (SCLC), drugs (SSRIs, carbamazepine, cyclophosphamide)
- Treatment: fluid restriction, salt tablets, demeclocycline, tolvaptan
13.6 Diabetes Insipidus

- Central DI causes: trauma, surgery, tumors (craniopharyngioma), infiltrative (sarcoid, histiocytosis)
- Nephrogenic DI causes: lithium, hypercalcemia, hypokalemia, chronic kidney disease, congenital
13.7 Hypercalcemia
- Causes: hyperparathyroidism (most common outpatient), malignancy (most common inpatient - PTHrP, lytic lesions, calcitriol in lymphoma)
- Other: vitamin D intoxication, granulomatous disease, thiazides, milk-alkali syndrome, immobilization
- Treatment: IV saline, loop diuretics, bisphosphonates, calcitonin, dialysis
13.8 Hypocalcemia
- Causes: hypoparathyroidism, vitamin D deficiency, CKD, hypomagnesemia, acute pancreatitis, tumor lysis
- Clinical: Chvostek sign, Trousseau sign, tetany, seizures, prolonged QT
- Treatment: calcium gluconate (IV if symptomatic), oral calcium, vitamin D; correct hypomagnesemia
14. Urinary Tract Infections and Related Disorders
14.1 Acute Pyelonephritis
- Fever, chills, flank pain, costovertebral angle tenderness, nausea, vomiting
- Urine: pyuria, WBC casts, bacteriuria, positive culture
- Organisms: E. coli (80%), Klebsiella, Proteus, Enterococcus
- Treatment: fluoroquinolone or ceftriaxone for 7-14 days; hospitalize if septic or unable to tolerate oral
14.2 Chronic Pyelonephritis
- Recurrent kidney infections → chronic tubulointerstitial inflammation and scarring
- Causes: VUR, obstruction, chronic stones
- Imaging: cortical scarring overlying blunted calyces
- Treatment: treat UTI, correct anatomic abnormalities
14.3 Xanthogranulomatous Pyelonephritis
- Chronic severe infection with foamy lipid-laden macrophages
- Associated with Proteus infection and staghorn calculi
- CT: enlarged kidney with mass-like appearance
- Treatment: nephrectomy
14.4 Renal Papillary Necrosis
- Ischemic necrosis of renal papillae
- Causes (POSTCARDS): Pyelonephritis, Obstruction, Sickle cell, TB, Cirrhosis, Analgesics (NSAIDs), Renal vein thrombosis, Diabetes, Systemic vasculitis
- Hematuria, flank pain, passing of tissue fragments in urine
- IVP: ring sign or contrast in necrotic papillae
14.5 Perinephric Abscess
- Collection of pus in perinephric space
- Causes: extension from pyelonephritis, hematogenous spread (S. aureus)
- Fever, flank pain persisting despite antibiotics
- CT: fluid collection with rim enhancement
- Treatment: drainage + antibiotics
15. Renal Neoplasms
15.1 Renal Cell Carcinoma

- Risk factors: smoking, obesity, hypertension, VHL, acquired cystic kidney disease in dialysis patients
- Classic triad (10%): hematuria, flank pain, palpable mass
- Paraneoplastic: polycythemia (EPO), hypercalcemia (PTHrP), hypertension (renin), Stauffer syndrome (reversible hepatic dysfunction)
- Metastases: lung, bone, brain; cannonball metastases in lungs
- Diagnosis: CT/MRI abdomen; renal mass protocol CT
- Treatment: partial or radical nephrectomy; sunitinib, pazopanib (VEGF inhibitors), nivolumab (immunotherapy) for metastatic
15.2 Wilms Tumor (Nephroblastoma)
- Most common renal malignancy in children (peak age 2-5 years)
- WAGR syndrome: Wilms, Aniridia, Genitourinary abnormalities, mental Retardation; WT1 gene deletion
- Denys-Drash syndrome: male pseudohermaphroditism, glomerulopathy, Wilms tumor
- Beckwith-Wiedemann syndrome: macroglossia, organomegaly, hemihypertrophy, Wilms tumor
- Presentation: asymptomatic abdominal mass, hematuria, hypertension
- Treatment: nephrectomy + chemotherapy (vincristine, actinomycin D, doxorubicin); excellent prognosis (>90% cure)
15.3 Angiomyolipoma
- Benign tumor composed of blood vessels, smooth muscle, and fat
- Associated with tuberous sclerosis (bilateral, multiple); sporadic cases (unilateral, single)
- Risk of spontaneous hemorrhage if >4 cm
- Diagnosis: CT showing fat density (negative Hounsfield units)
- Treatment: observation if <4 cm;="" embolization="" or="" resection="" if="">4 cm or symptomatic
15.4 Oncocytoma
- Benign renal tumor; mahogany brown with central scar
- Cannot distinguish from RCC on imaging; diagnosed after nephrectomy
- No malignant potential
15.5 Transitional Cell Carcinoma (Urothelial Carcinoma)
- Arises from renal pelvis, ureter, bladder
- Risk factors: smoking, analgesic nephropathy, Balkan nephropathy, cyclophosphamide, aromatic amines
- Painless gross hematuria
- Treatment: nephroureterectomy for upper tract; TURBT for bladder
Related Searches
Summary, Semester Notes, practice quizzes, CheatSheet: Disorders of Kidney, Free, study material, ppt, MCQs, past year papers, pdf , Objective type Questions, Extra Questions, Viva Questions, Previous Year Questions with Solutions, video lectures, Exam, Important questions, mock tests for examination, CheatSheet: Disorders of Kidney, shortcuts and tricks, CheatSheet: Disorders of Kidney, Sample Paper;






