NEET PG Exam > NEET PG Notes > Medicine > CheatSheet: Nutrition
CheatSheet: Nutrition
1. Energy and Macronutrients
1.1 Energy Requirements
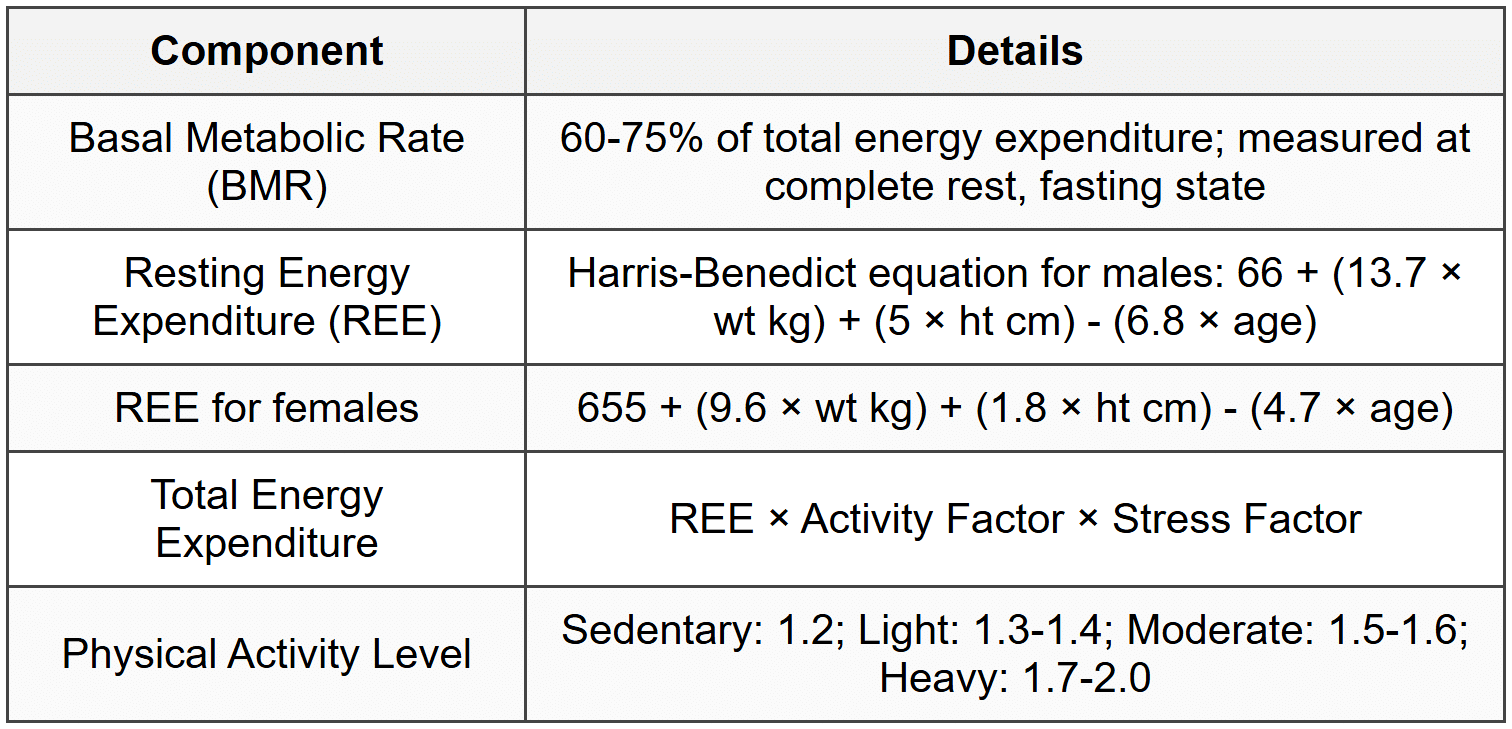
1.2 Carbohydrates
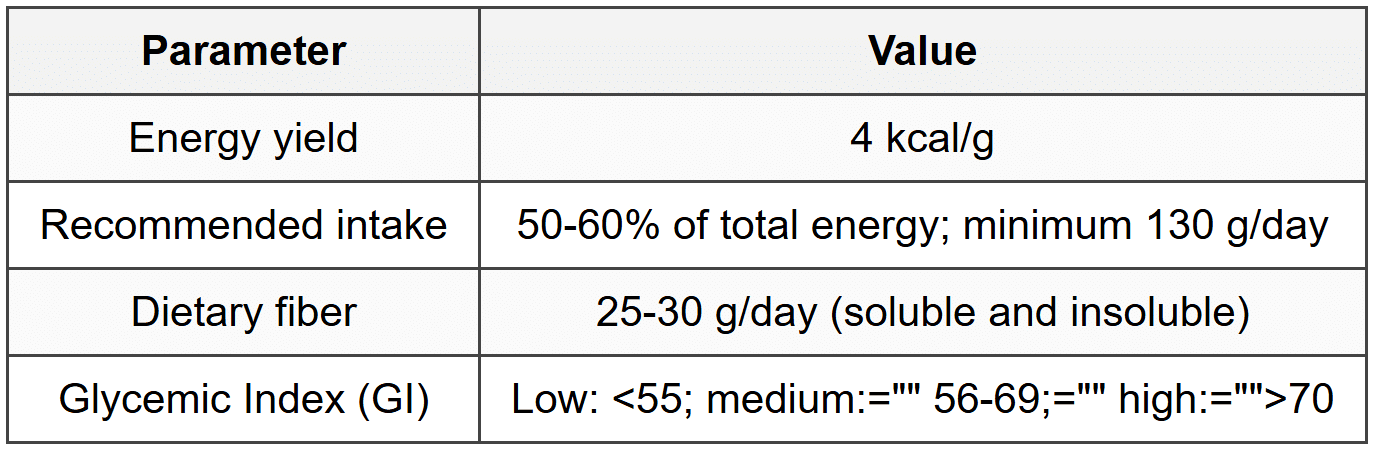

1.3 Proteins
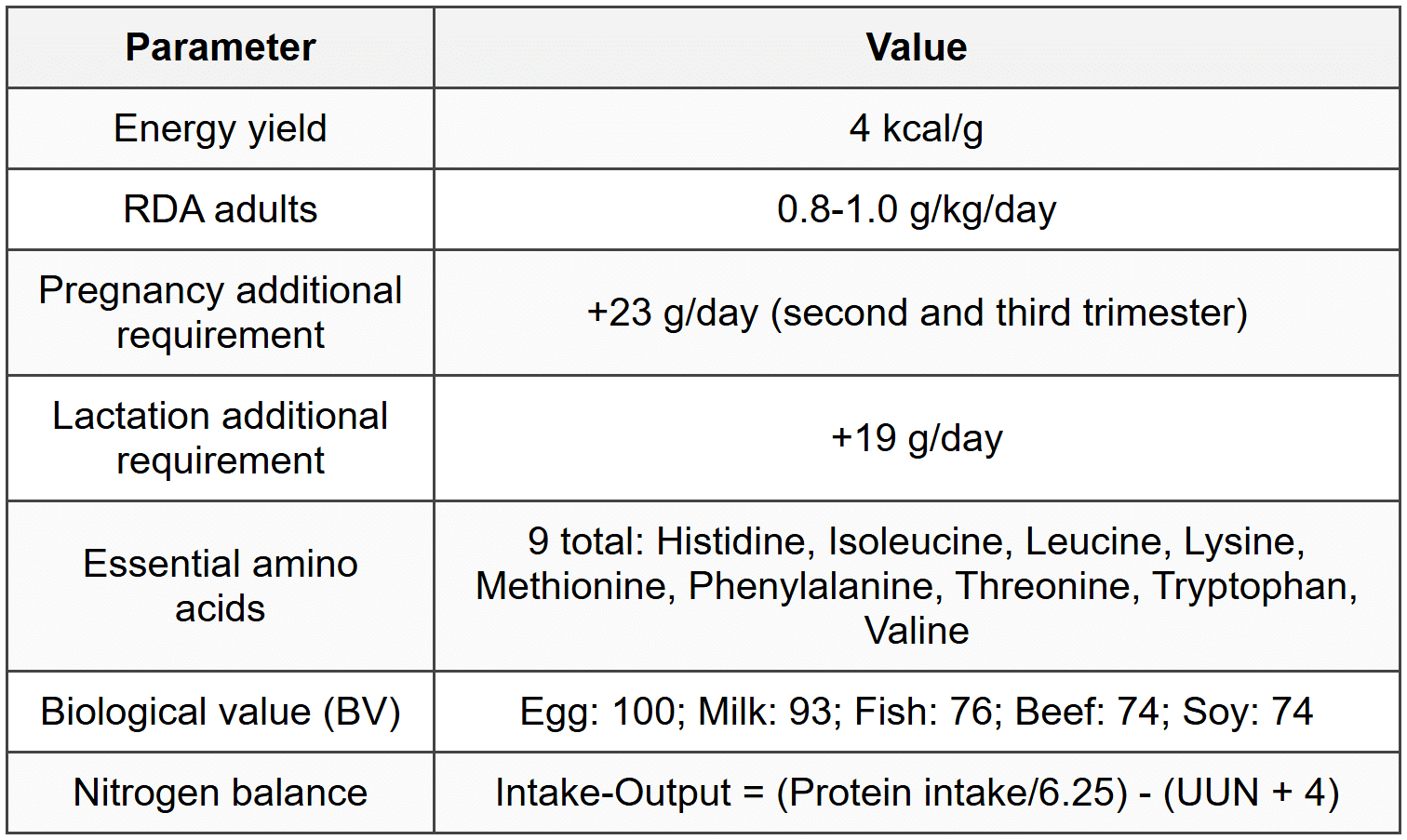
1.4 Fats
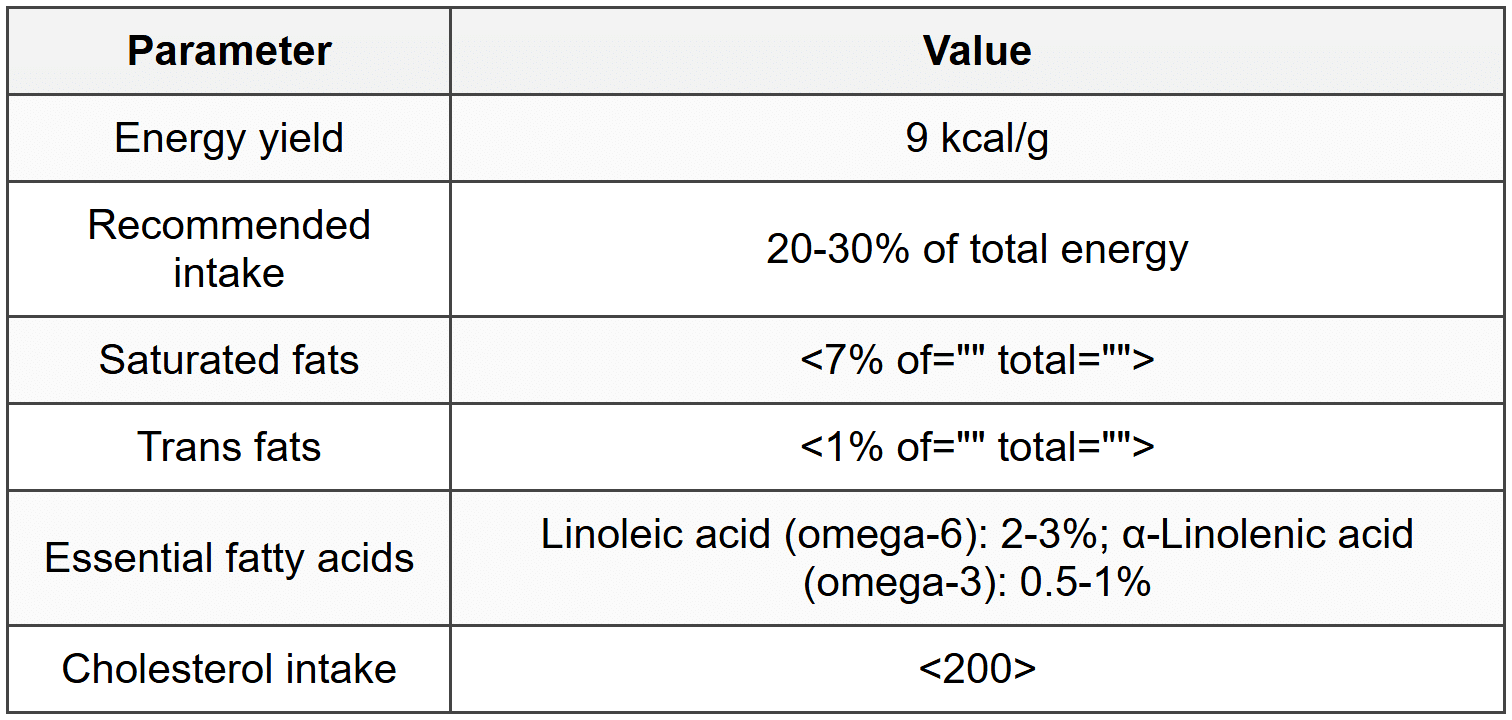
2. Micronutrients - Vitamins
2.1 Fat-Soluble Vitamins
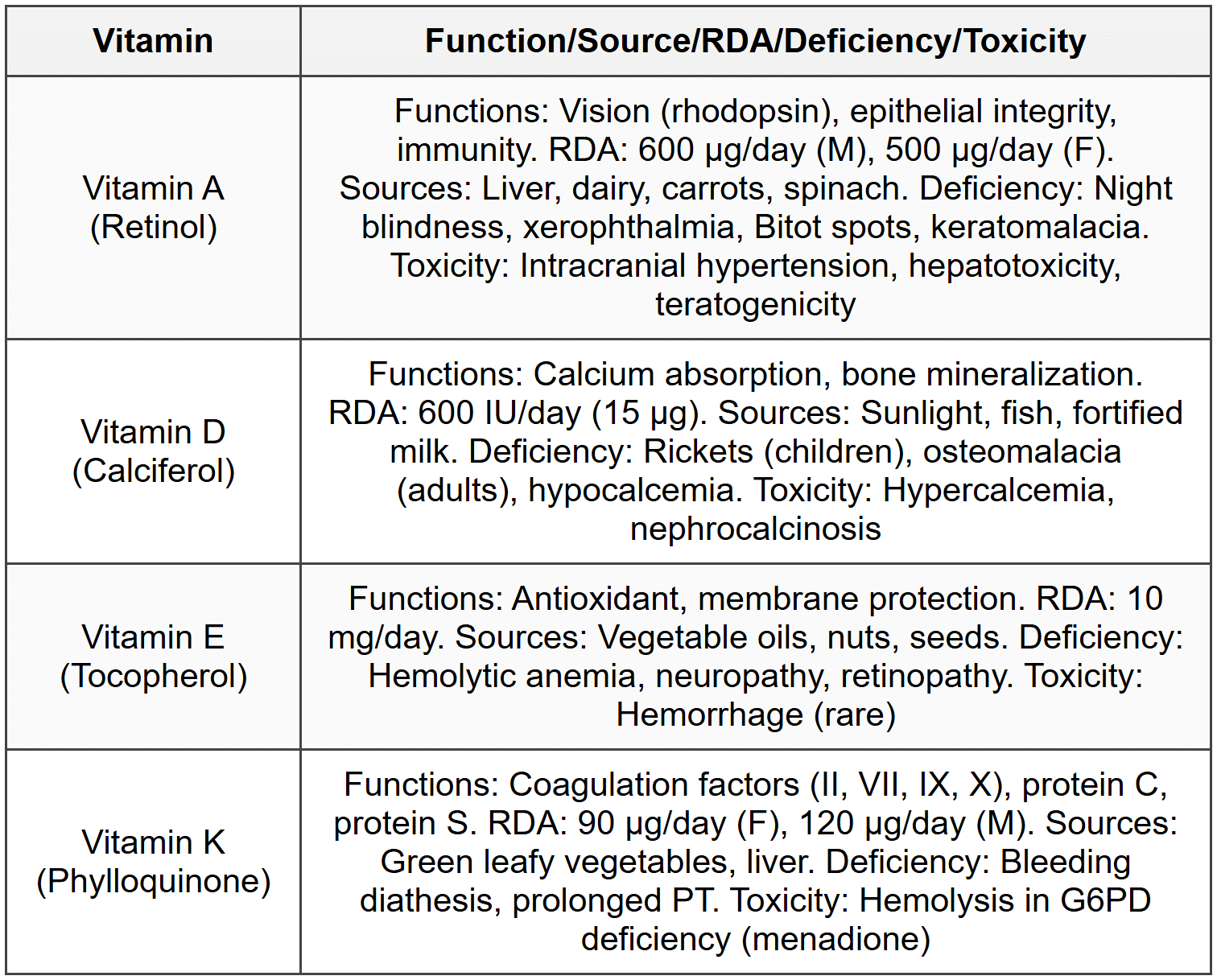
2.2 Water-Soluble Vitamins - B Complex
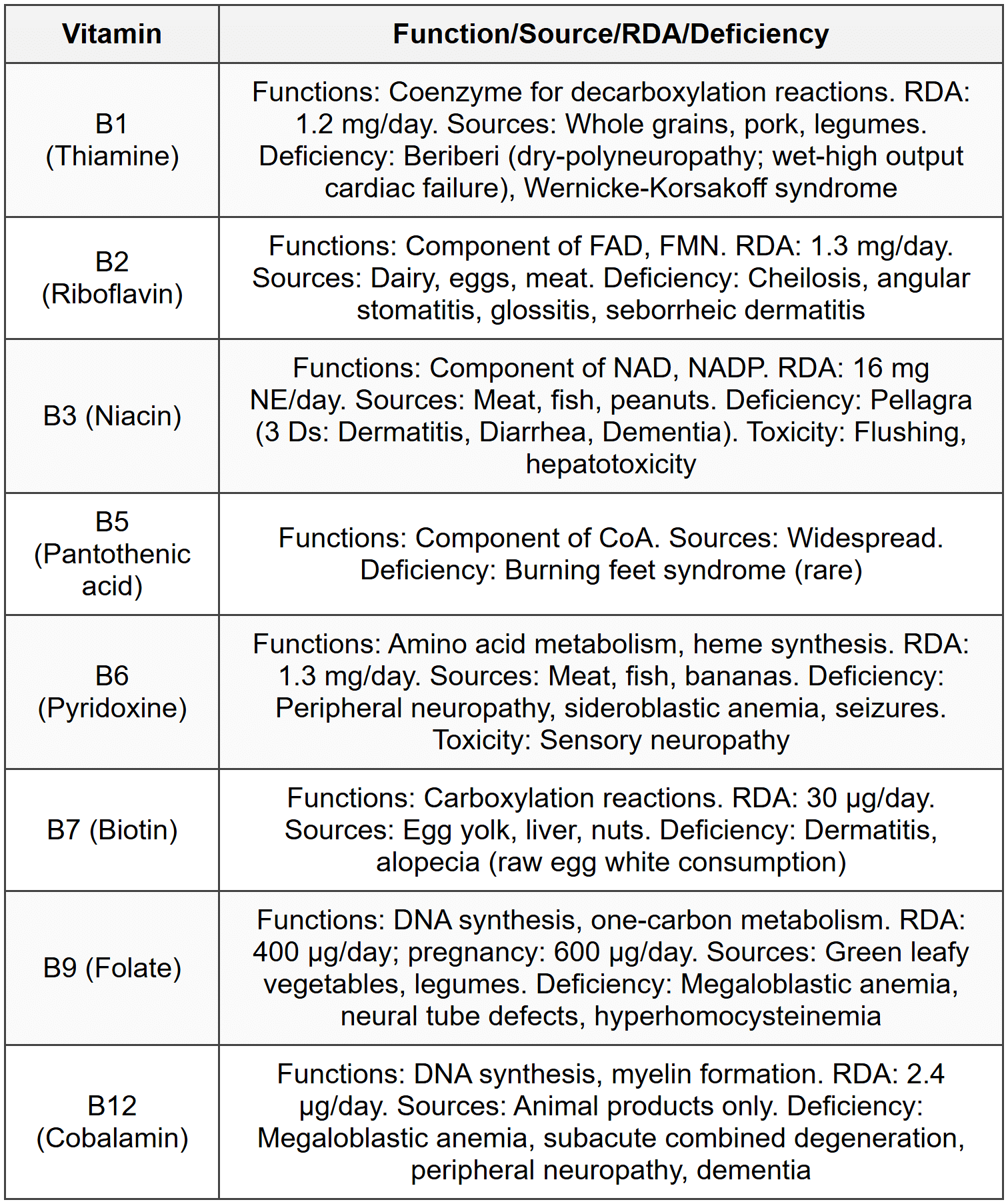
2.3 Vitamin C
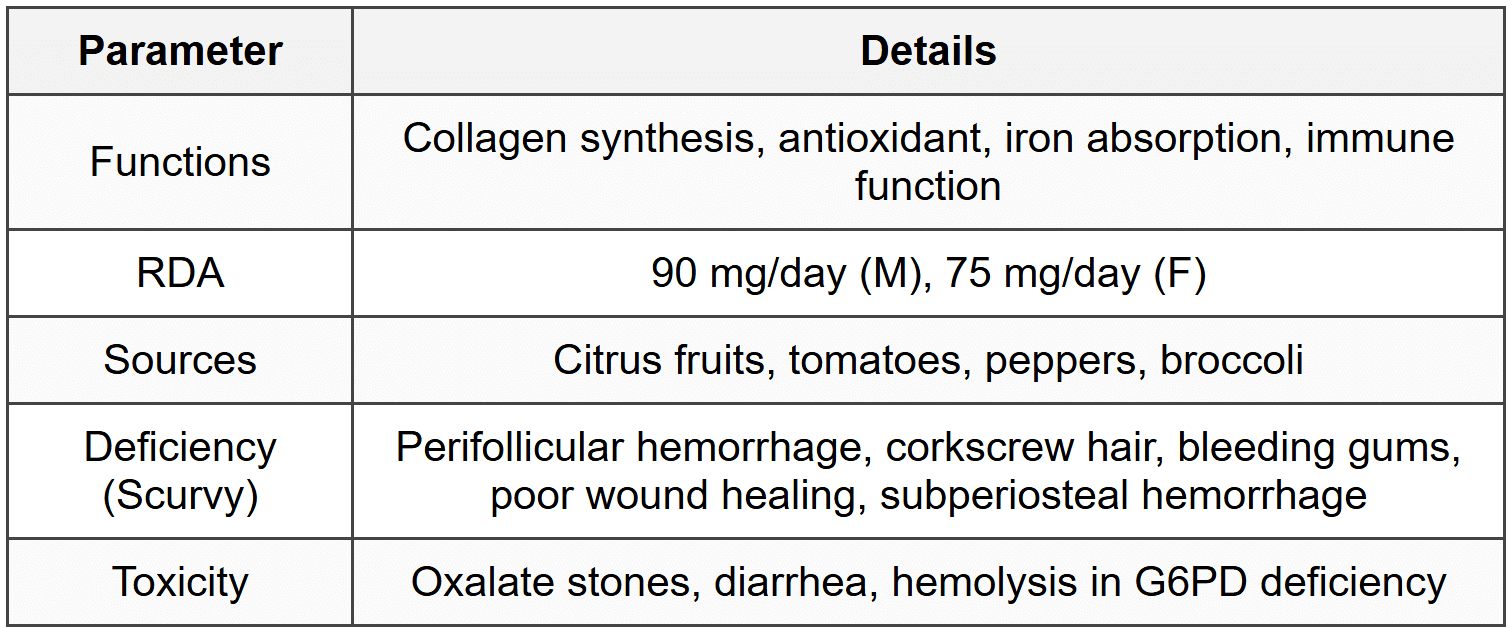
3. Micronutrients - Minerals
3.1 Macrominerals
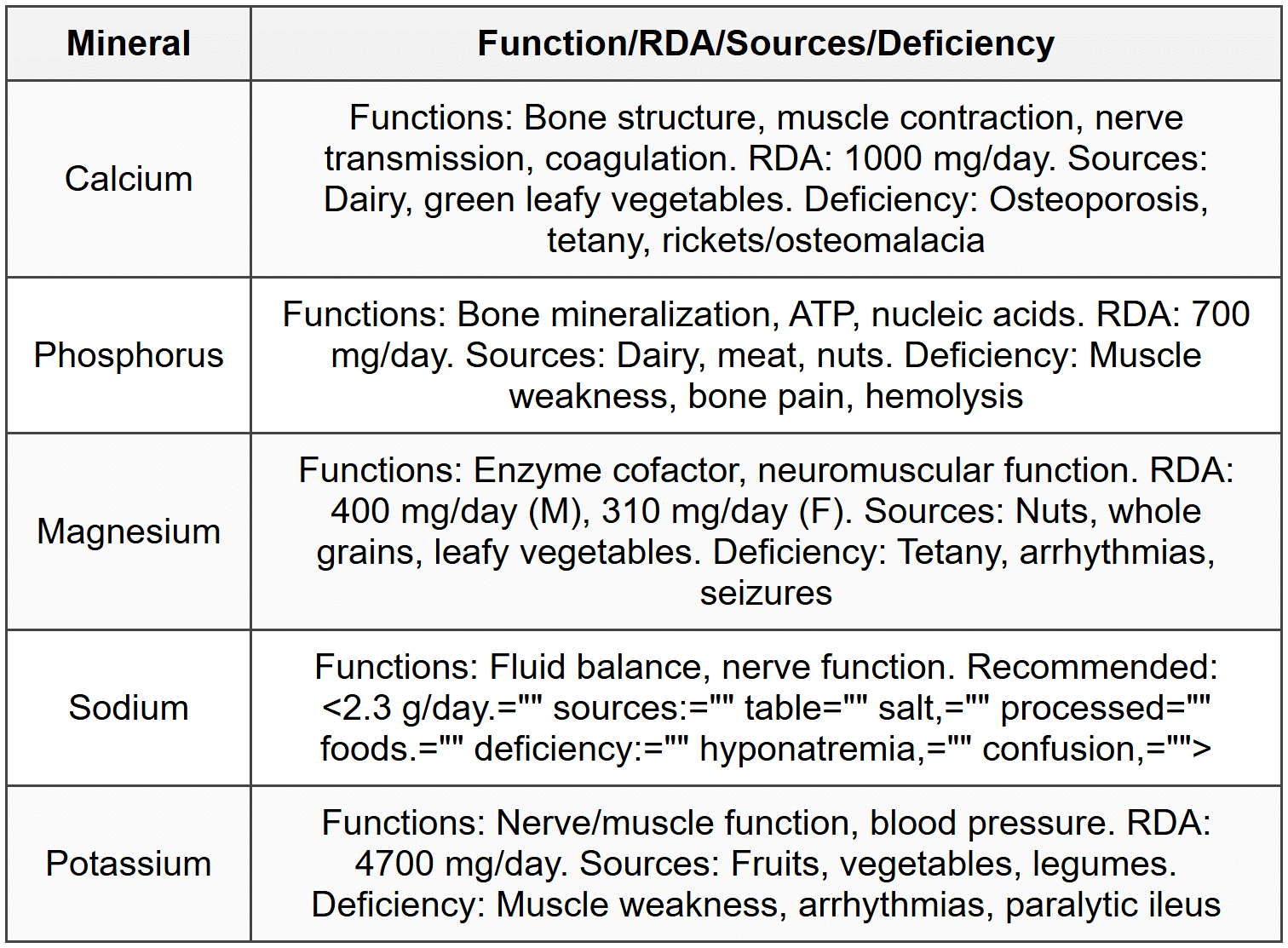
3.2 Trace Elements - Iron
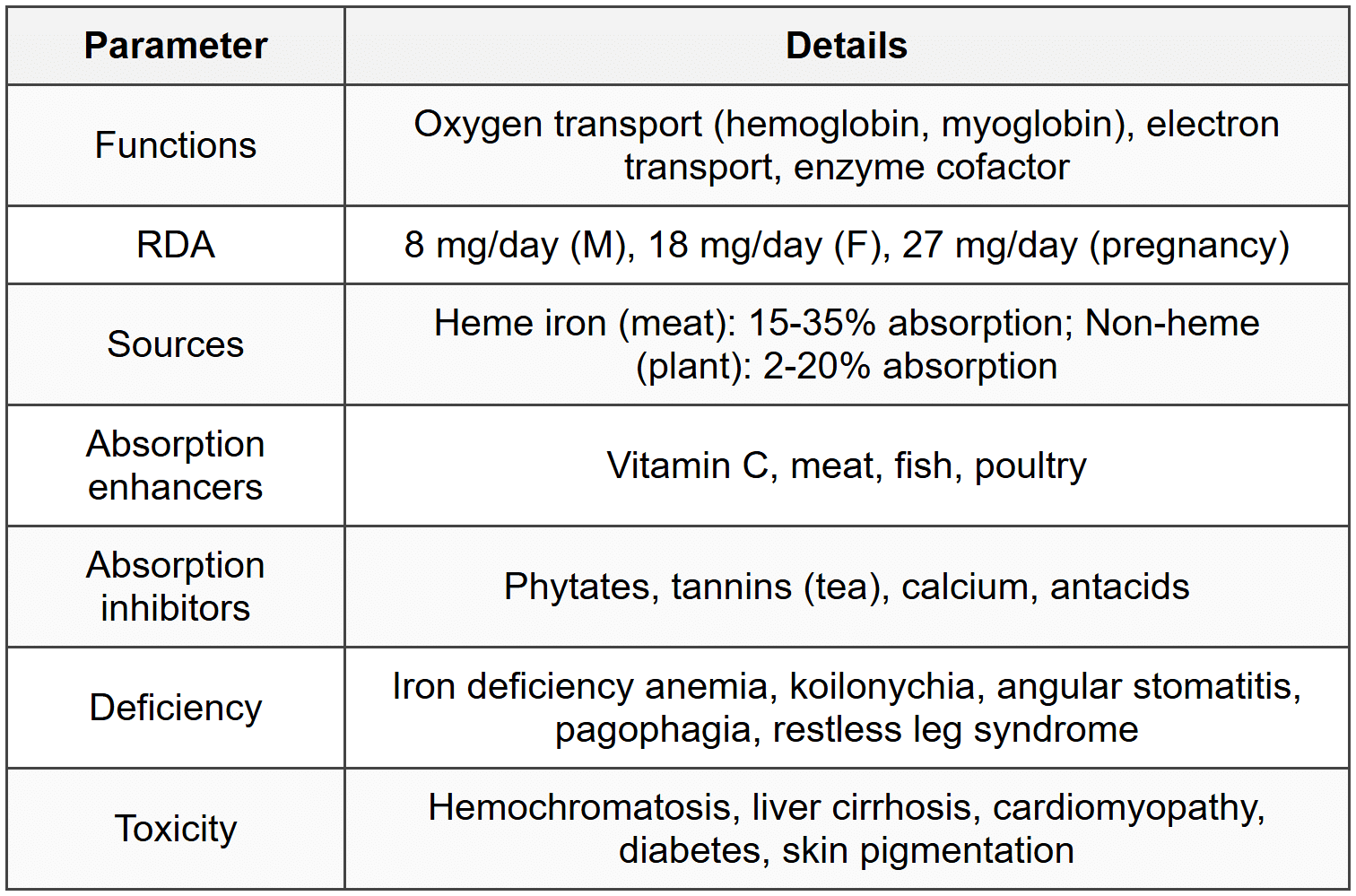
3.3 Other Trace Elements
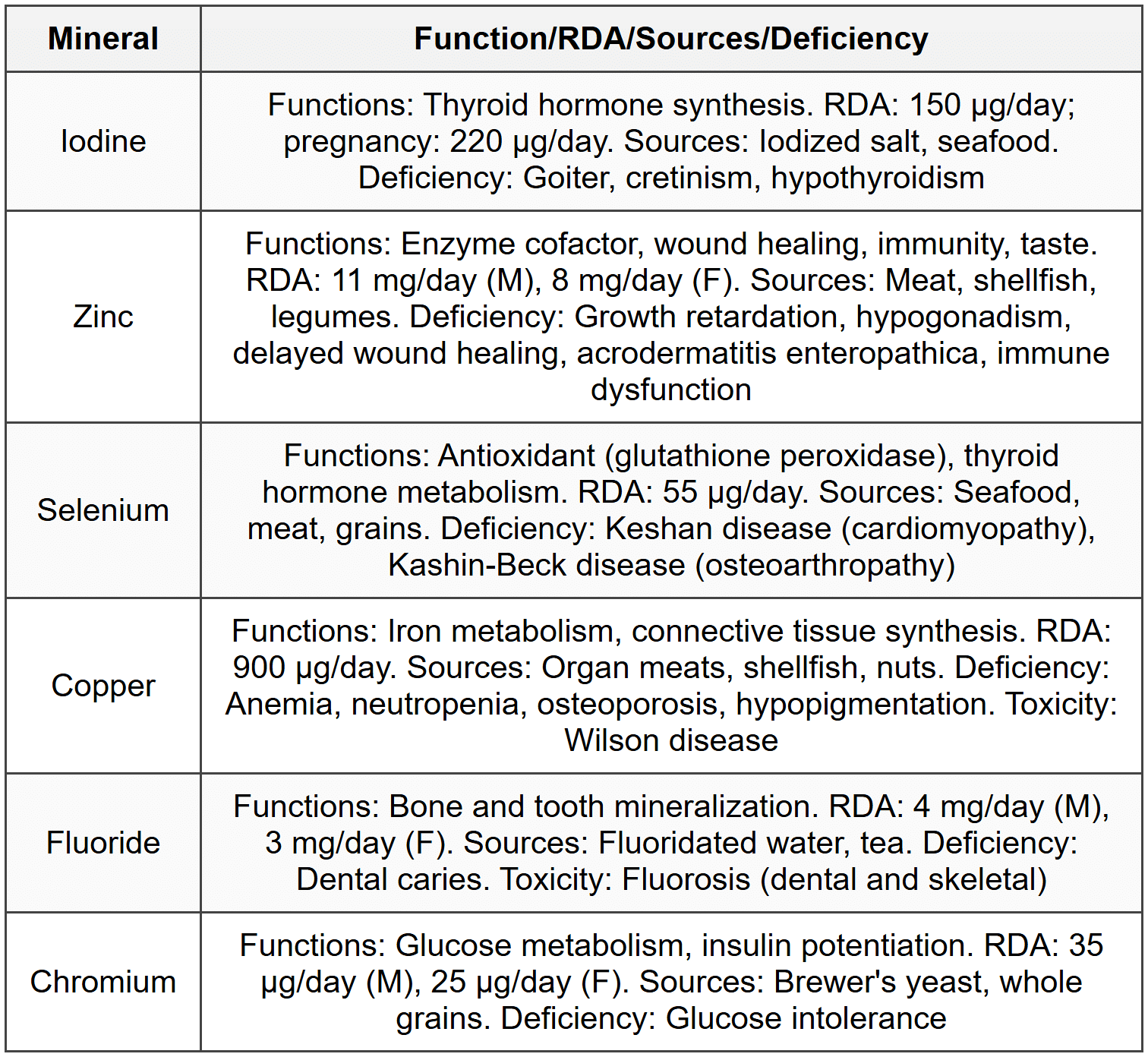
4. Protein-Energy Malnutrition
4.1 Classification
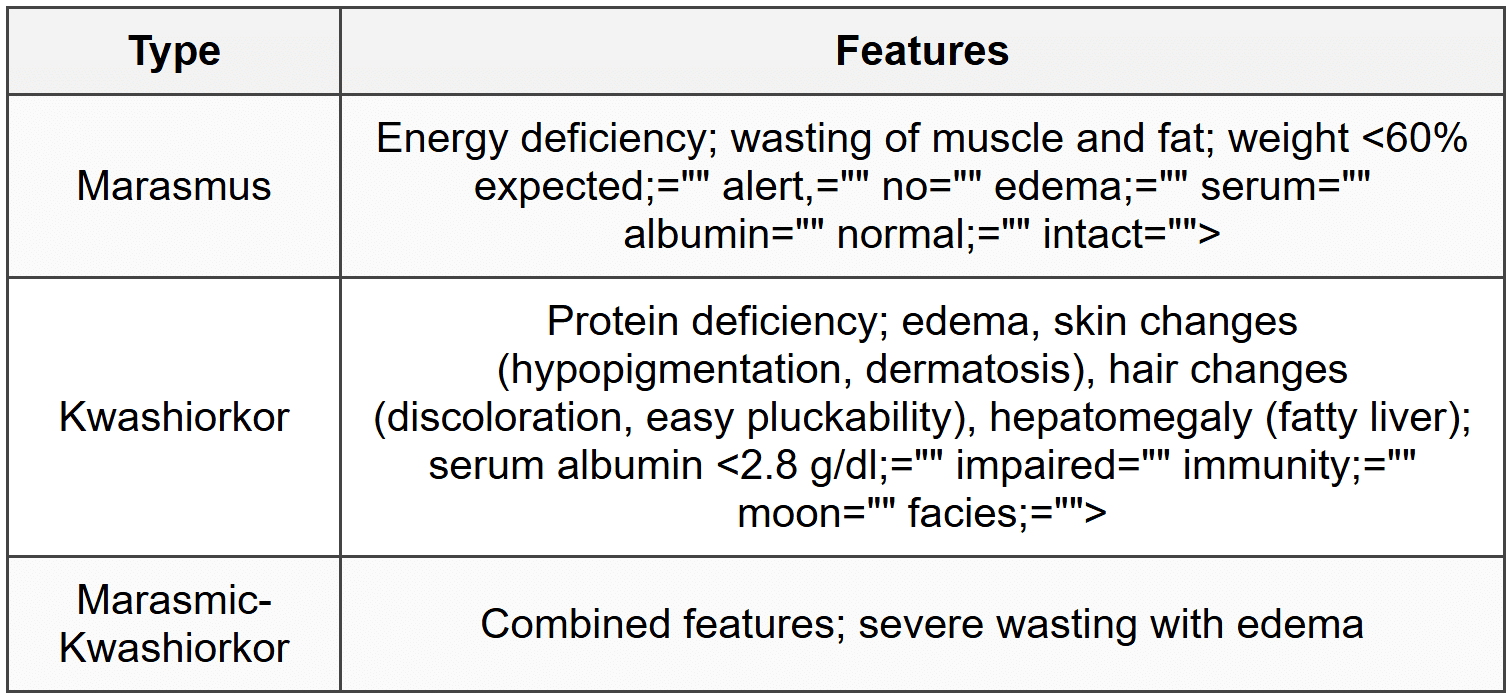

4.2 Anthropometric Assessment
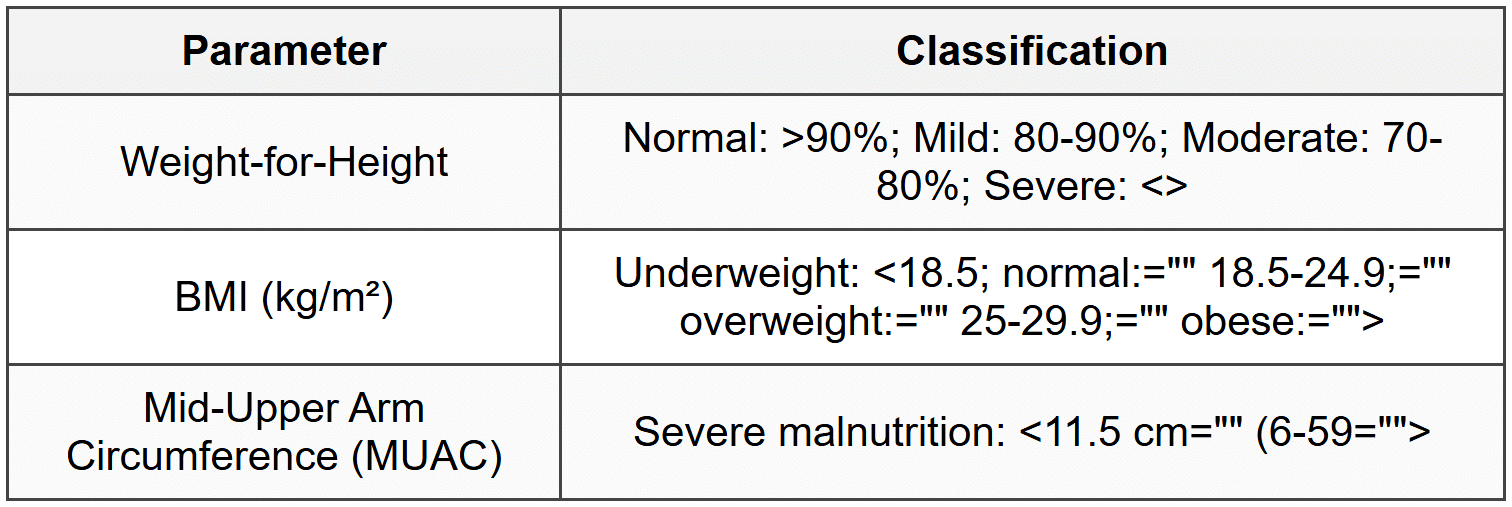
4.3 Management Principles
- Initial stabilization: Treat hypoglycemia, hypothermia, dehydration (use ReSoMal - reduced osmolarity), electrolyte imbalance
- Infections: Broad-spectrum antibiotics empirically
- Micronutrients: Multivitamin, folic acid, zinc, copper
- Feeding: Start with 80-100 kcal/kg/day, protein 1-1.5 g/kg/day; gradually increase
- F-75 formula (initial stabilization): 75 kcal/100 mL, 0.9 g protein/100 mL
- F-100 formula (rehabilitation): 100 kcal/100 mL, 2.9 g protein/100 mL
- Ready-to-Use Therapeutic Food (RUTF): Peanut-based paste, 500 kcal/92 g sachet
- Refeeding syndrome: Risk of hypophosphatemia, hypokalemia, hypomagnesemia; thiamine deficiency; monitor closely
5. Obesity
5.1 Classification and Assessment
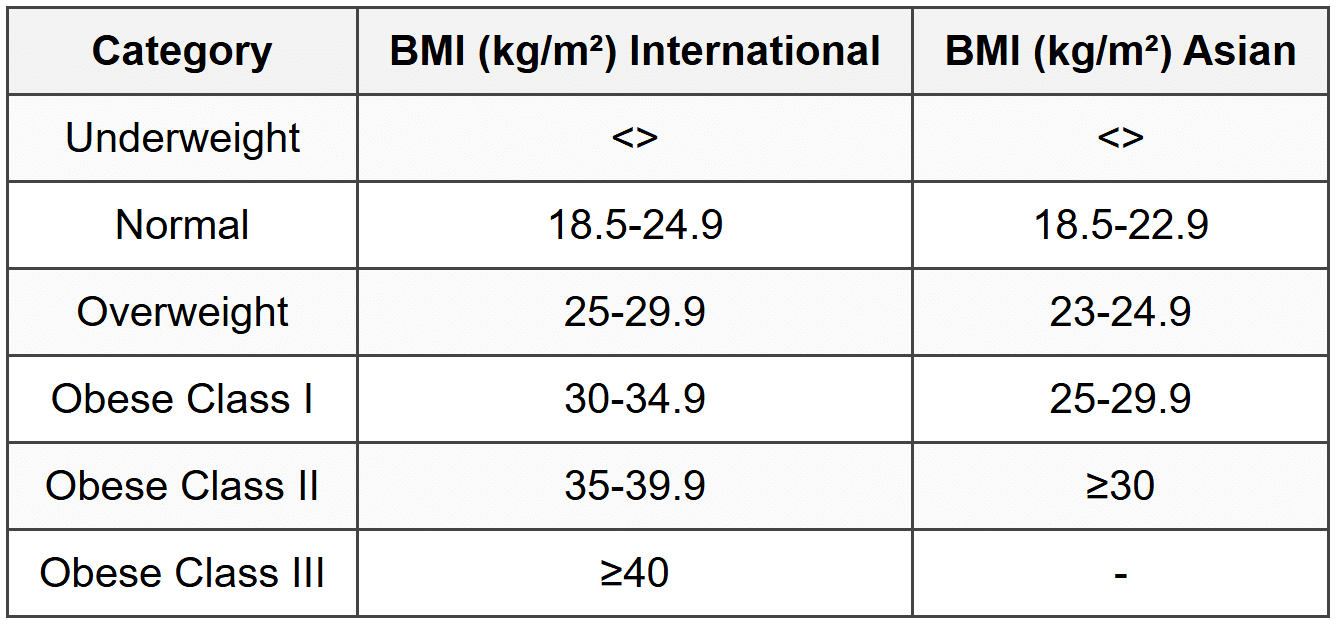
5.2 Central Obesity
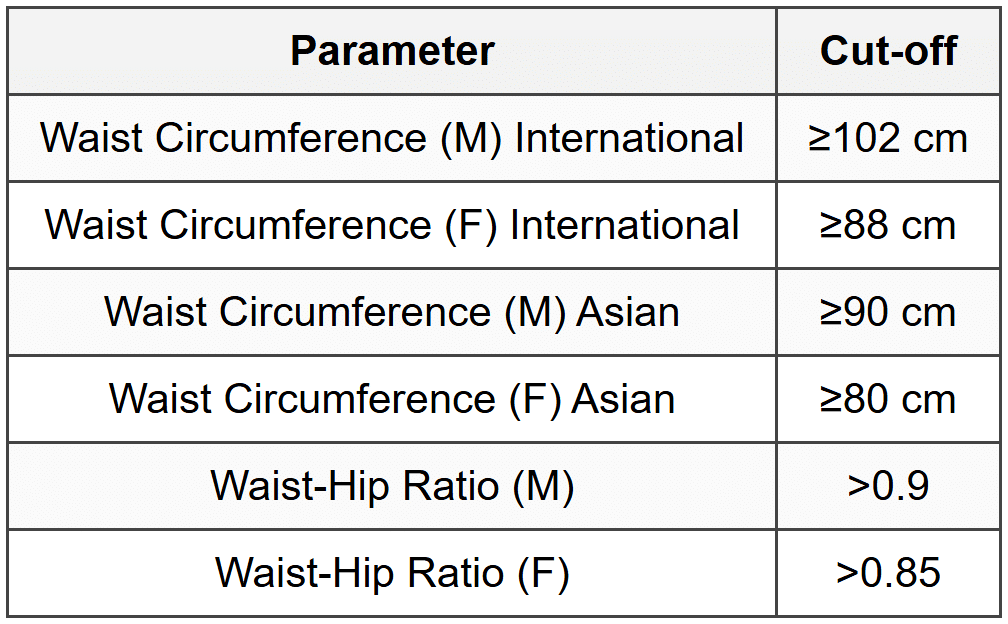
5.3 Complications
- Metabolic: Type 2 diabetes, dyslipidemia, metabolic syndrome, insulin resistance
- Cardiovascular: Hypertension, coronary artery disease, stroke, heart failure
- Respiratory: Obstructive sleep apnea, obesity hypoventilation syndrome, restrictive lung disease
- Gastrointestinal: NAFLD, NASH, gallstones, GERD
- Musculoskeletal: Osteoarthritis, gout
- Reproductive: PCOS, infertility, complications in pregnancy
- Malignancy: Breast, endometrial, colon, kidney, esophageal cancers
- Psychological: Depression, low self-esteem
5.4 Management
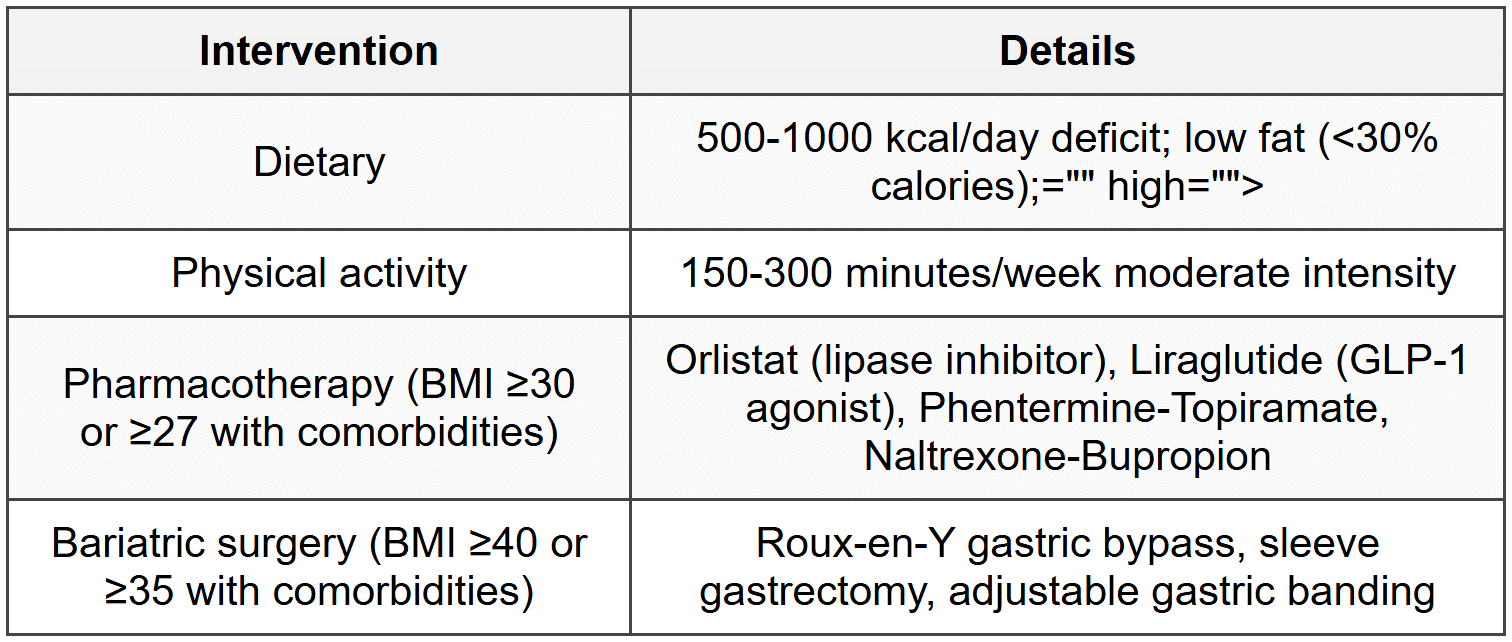
6. Specific Nutritional Deficiencies
6.1 Iodine Deficiency Disorders
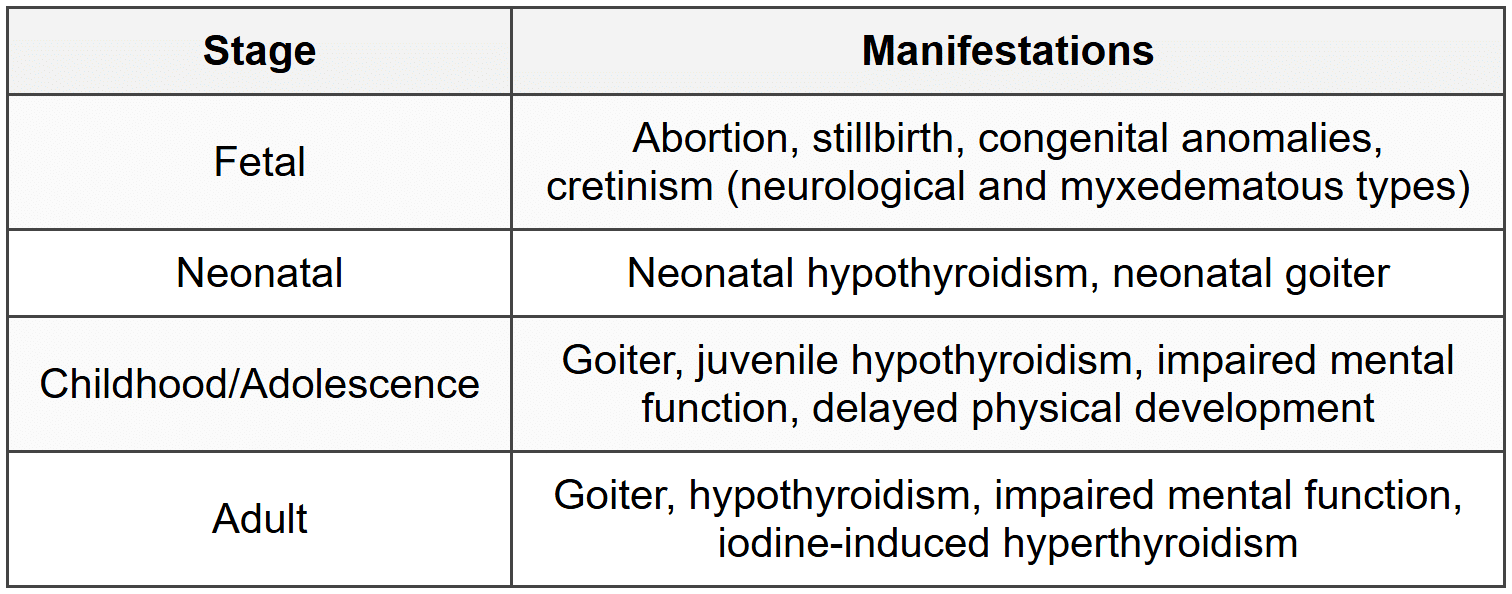
6.2 Zinc Deficiency
- Growth retardation and dwarfism
- Hypogonadism and delayed sexual maturation
- Acrodermatitis enteropathica: periorificial and acral dermatitis
- Delayed wound healing
- Immune dysfunction, increased infections
- Alopecia, glossitis, nail dystrophy
- Night blindness, photophobia
- Diarrhea
6.3 Vitamin A Deficiency
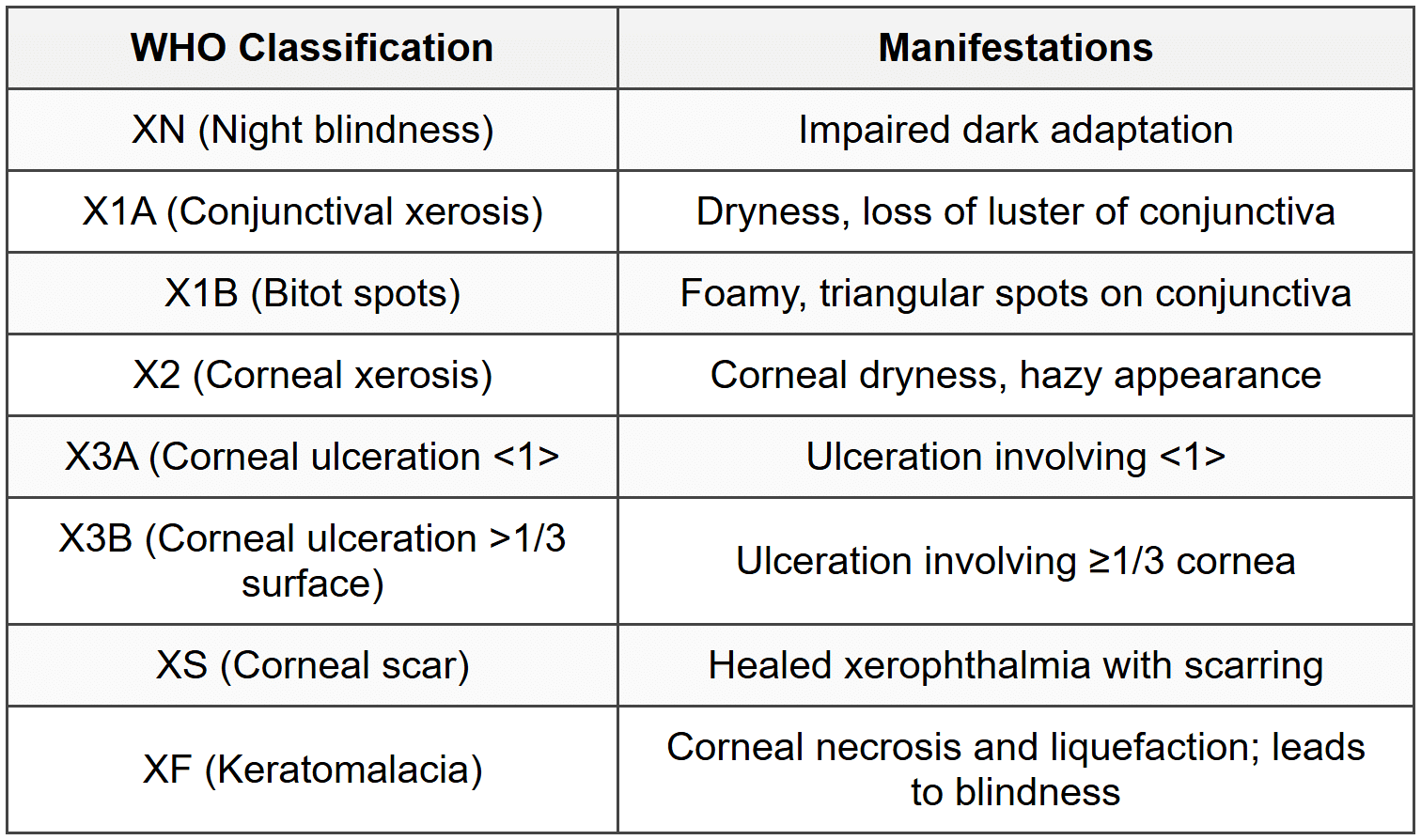
6.4 Vitamin D Deficiency
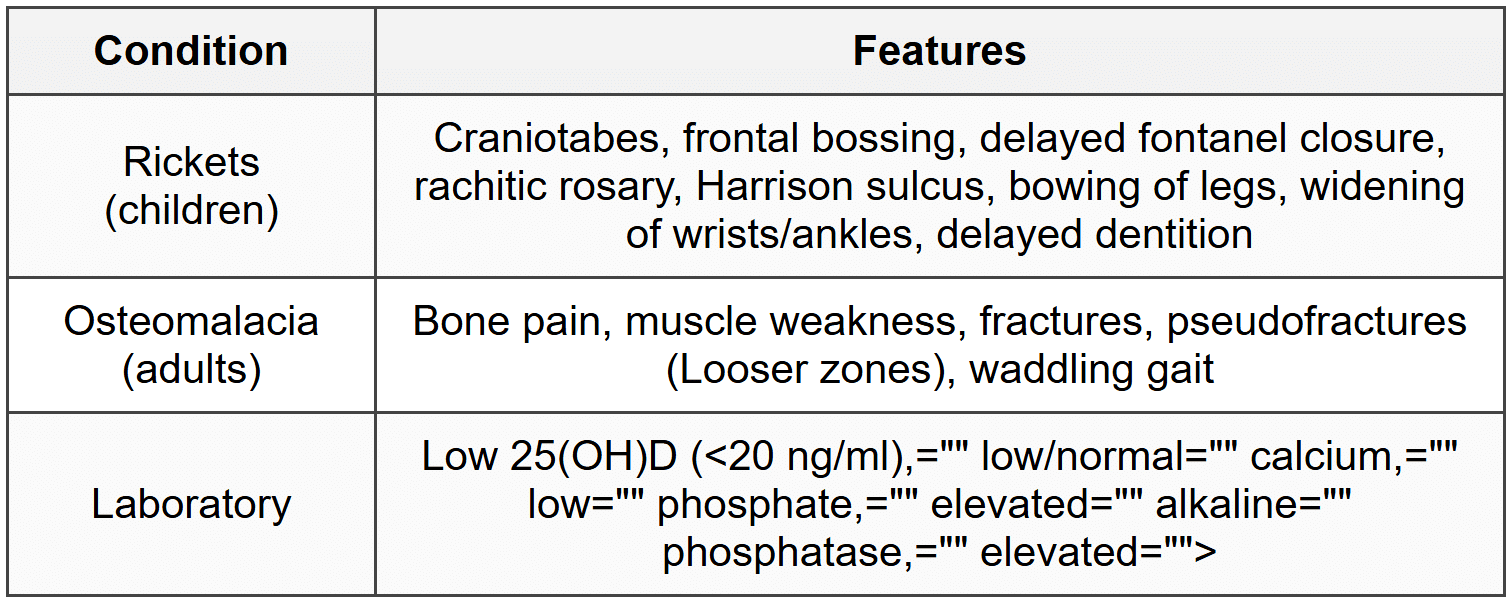
7. Special Nutritional Requirements
7.1 Pregnancy
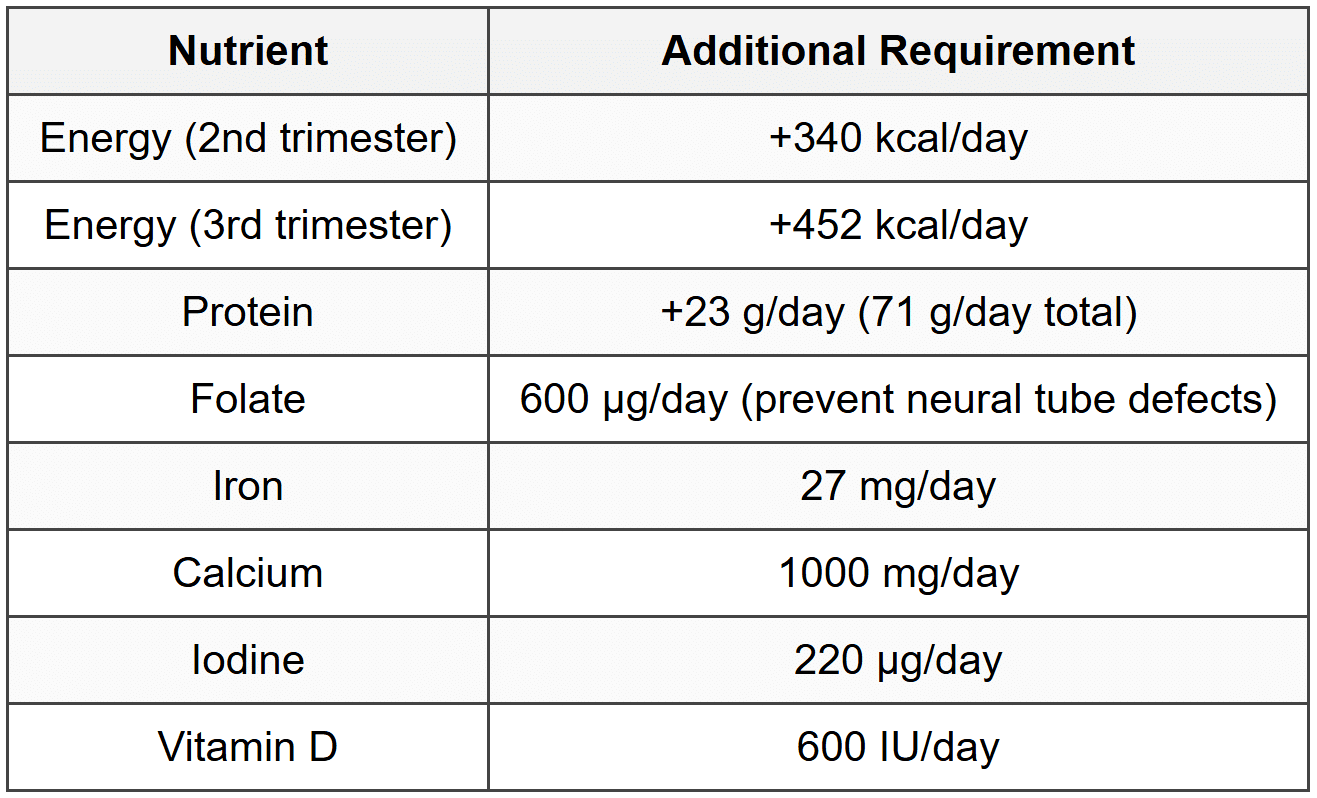
7.2 Lactation
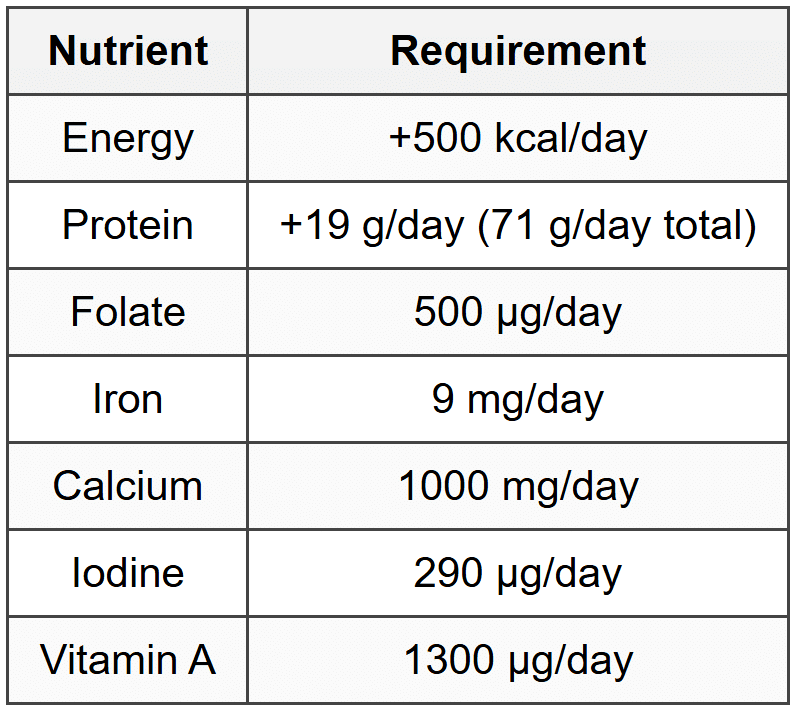
7.3 Elderly
- Decreased energy requirements due to reduced basal metabolic rate and physical activity
- Increased protein requirements: 1.0-1.2 g/kg/day to prevent sarcopenia
- Vitamin D: 800-1000 IU/day (reduced skin synthesis, decreased sun exposure)
- Vitamin B12: Risk of deficiency due to atrophic gastritis, decreased intrinsic factor
- Calcium: 1200 mg/day (prevent osteoporosis)
- Fiber: Prevent constipation
- Hydration: Decreased thirst sensation, risk of dehydration
7.4 Athletes
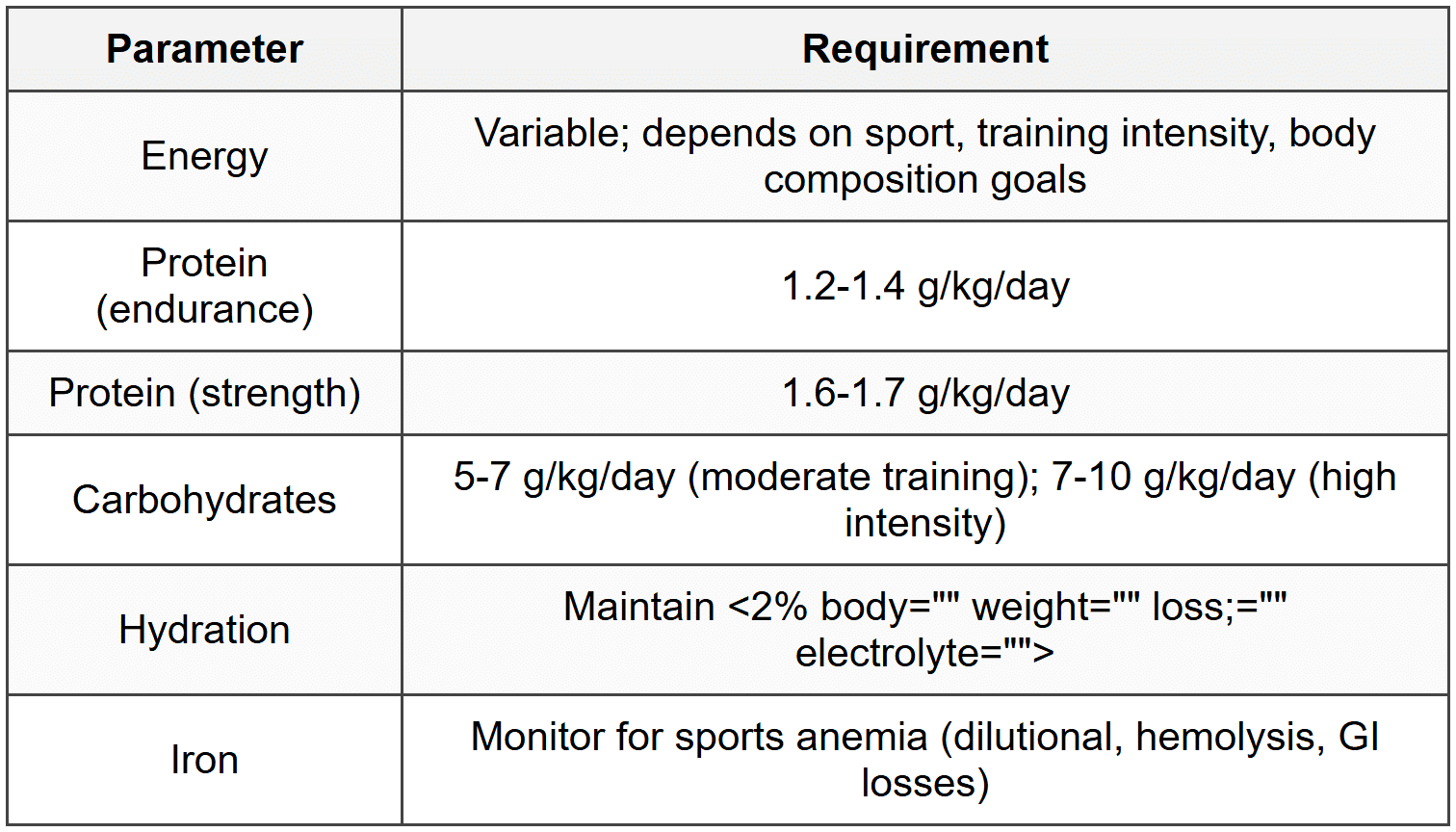
8. Nutritional Support
8.1 Enteral Nutrition
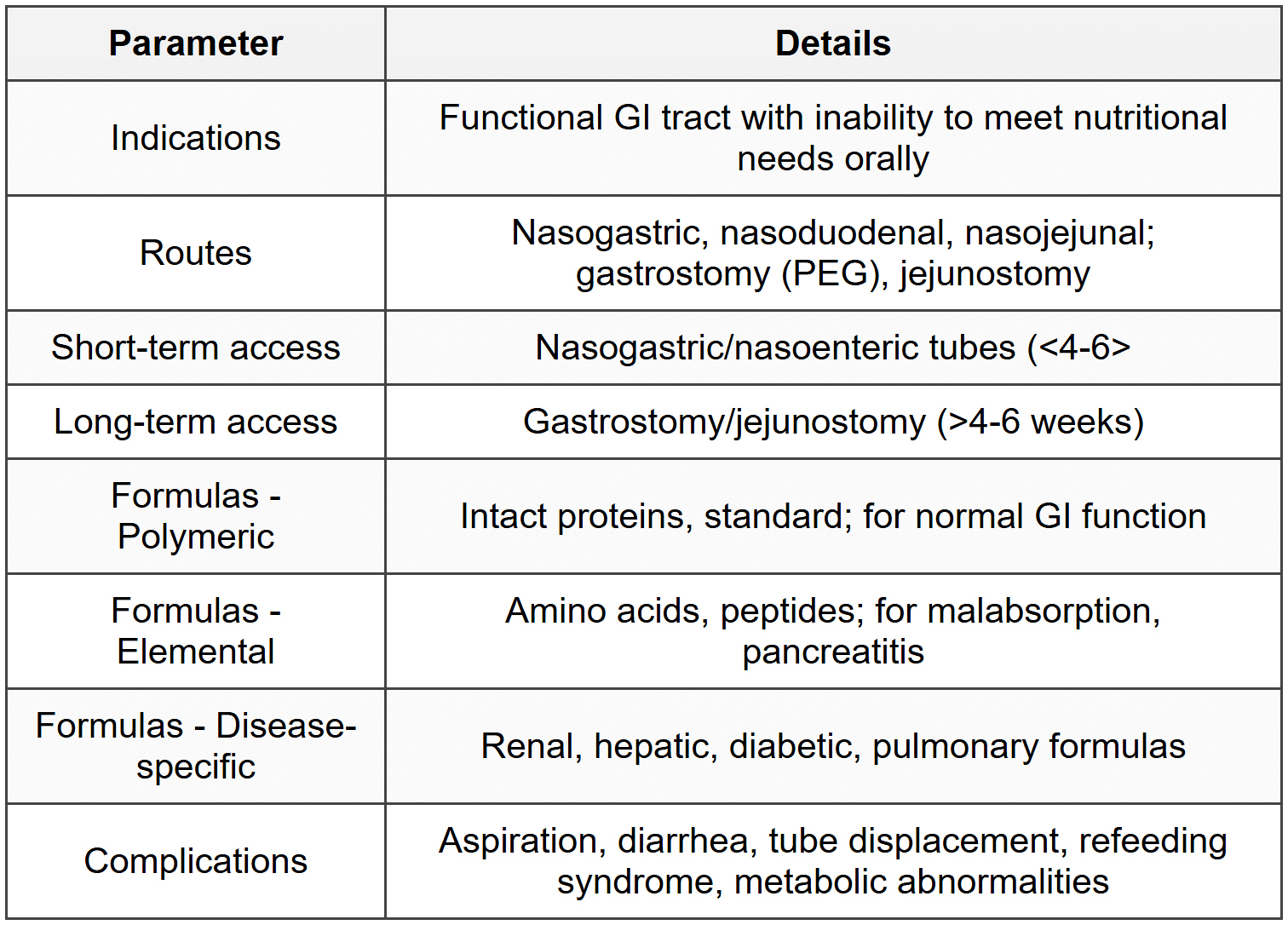
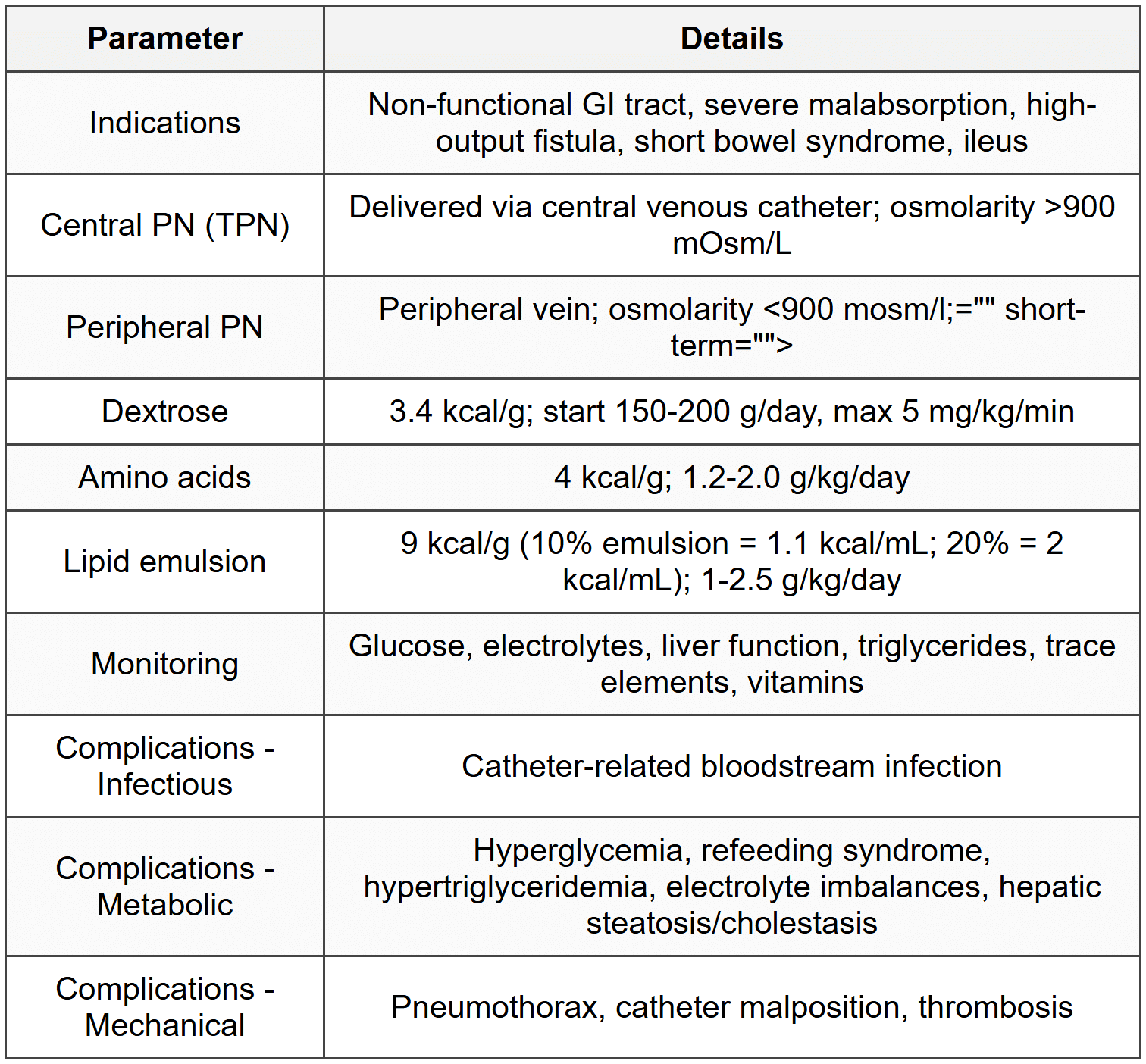
8.2 Parenteral Nutrition
8.3 Refeeding Syndrome
- Definition: Metabolic complications following reintroduction of nutrition in malnourished patients
- Mechanism: Insulin surge → intracellular shift of phosphate, potassium, magnesium; thiamine depletion
- Risk factors: Prolonged fasting, chronic malnutrition, anorexia nervosa, chronic alcoholism
- Features: Hypophosphatemia (<0.6 mmol/l),="" hypokalemia,="" hypomagnesemia,="" thiamine="">
- Complications: Cardiac arrhythmias, heart failure, respiratory failure, seizures, rhabdomyolysis, hemolysis
- Prevention: Start nutrition slowly (25% of requirements); supplement thiamine, phosphate, potassium, magnesium; monitor electrolytes closely
9. Nutritional Assessment
9.1 Anthropometric Measurements
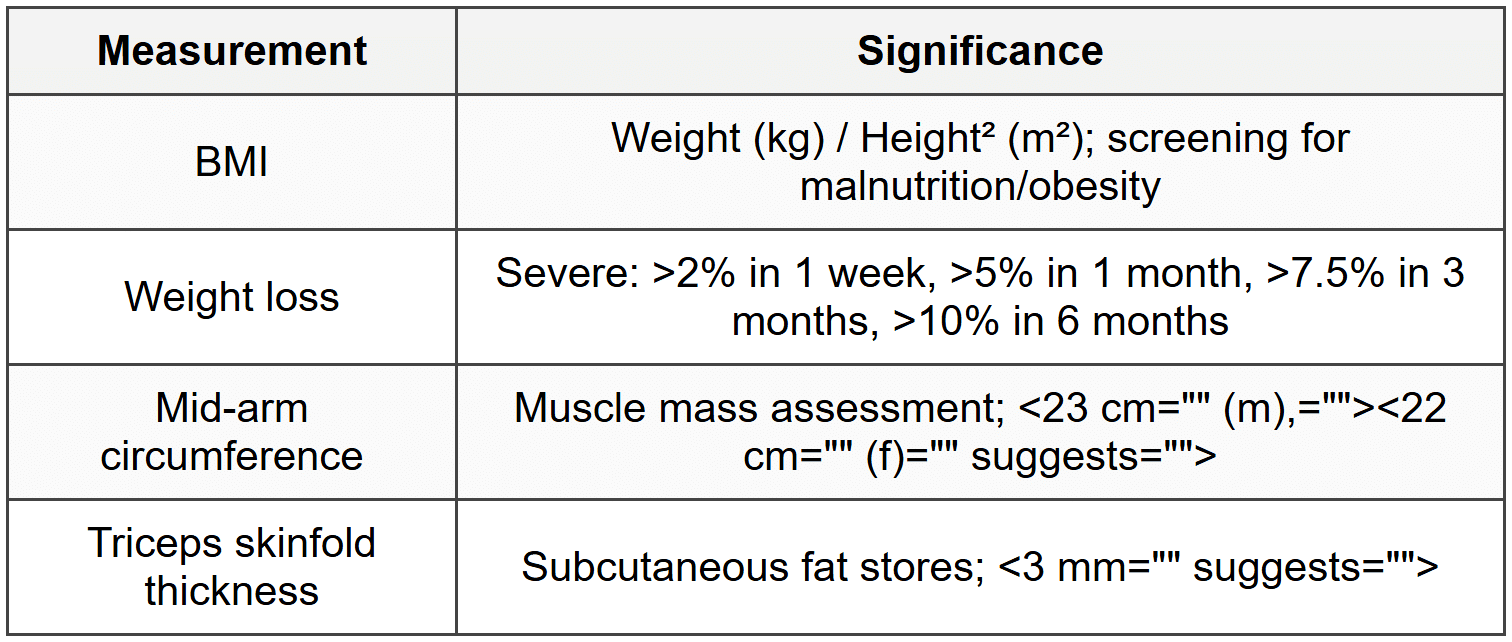
9.2 Biochemical Markers
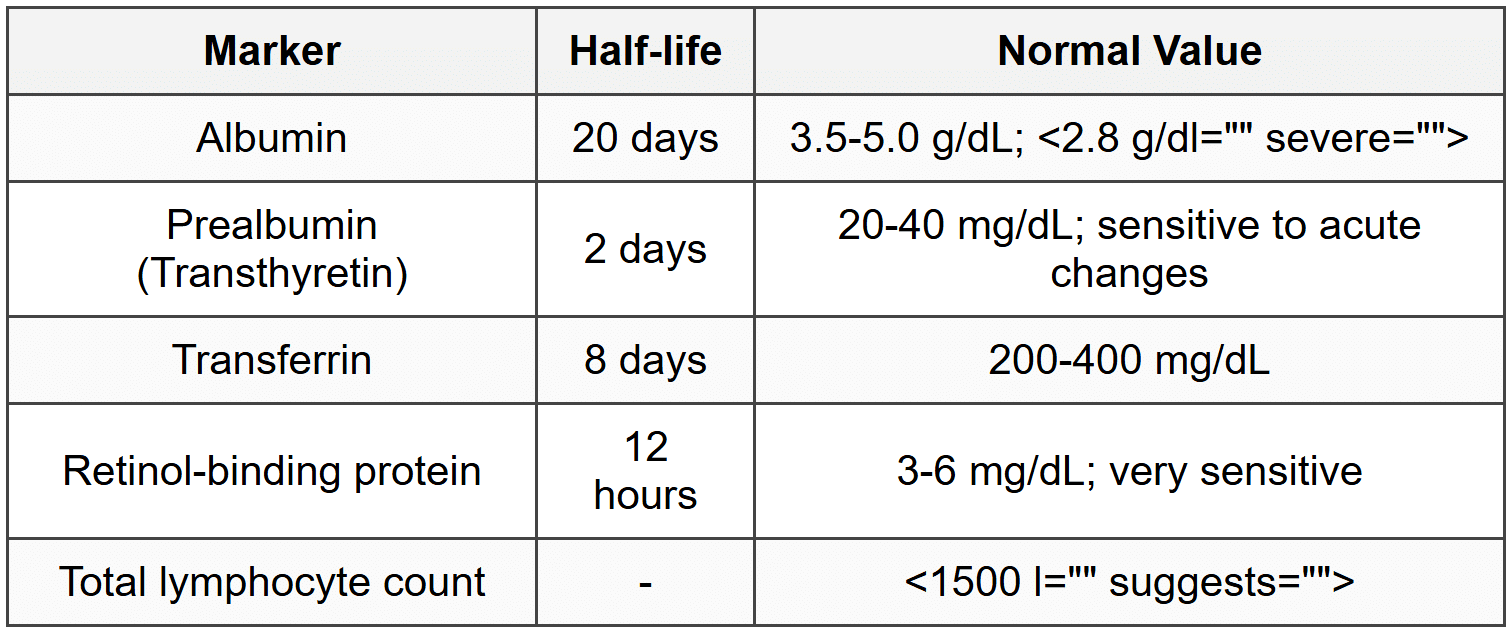
9.3 Screening Tools
- MUST (Malnutrition Universal Screening Tool): BMI, weight loss, acute disease effect
- NRS-2002 (Nutritional Risk Screening): Severity of disease, nutritional impairment, age
- SGA (Subjective Global Assessment): History (weight change, intake, GI symptoms, functional capacity) + physical examination
- MNA (Mini Nutritional Assessment): Primarily for elderly
10. Disease-Specific Nutrition
10.1 Diabetes Mellitus
- Carbohydrates: 45-60% of total energy; emphasize complex carbohydrates, low glycemic index foods
- Fiber: ≥25 g/day (F), ≥38 g/day (M)
- Protein: 15-20% of total energy; 1.0-1.5 g/kg/day
- Fats: <30% total="" energy;="" saturated="" fats=""><7%, trans="" fats="">
- Sodium: <2.3 g/day;=""><1.5 g/day="" if="">
- Alcohol: Moderate (≤1 drink/day for F, ≤2 drinks/day for M); avoid if poor glycemic control or hypertriglyceridemia
10.2 Chronic Kidney Disease
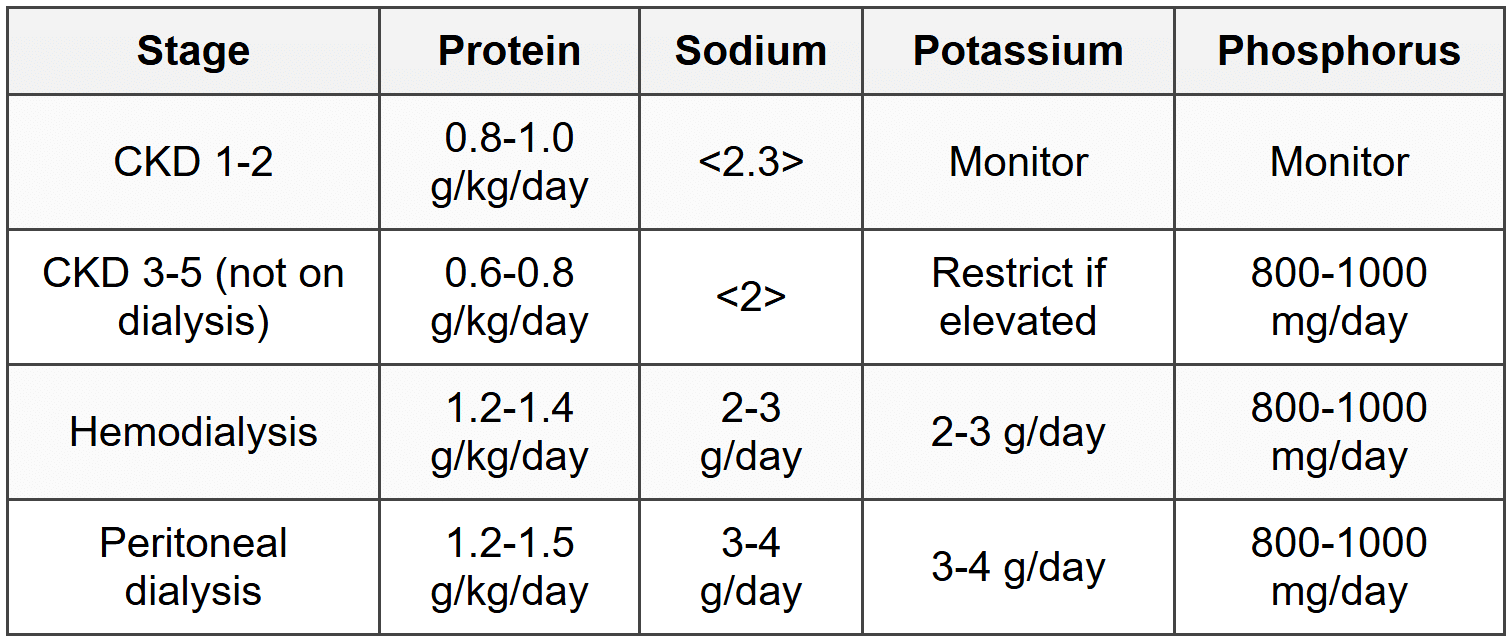
10.3 Chronic Liver Disease
- Energy: 35-40 kcal/kg/day
- Protein: 1.2-1.5 g/kg/day; use branched-chain amino acids if hepatic encephalopathy
- Sodium: <2 g/day="" if="">
- Fluid restriction: If hyponatremia present
- Vitamin supplementation: Thiamine, folate, vitamin K
- Zinc supplementation: 220 mg zinc sulfate twice daily
- Late evening snack: Prevent overnight catabolism
10.4 Inflammatory Bowel Disease
- Active Crohn disease: Low residue diet, consider elemental/polymeric feeds
- Stricturing Crohn: Low fiber to prevent obstruction
- Fat malabsorption: Medium-chain triglycerides
- Lactose intolerance: Common; limit dairy
- Iron, B12, folate, vitamin D, zinc supplementation as needed
- Parenteral nutrition: Severe disease, bowel rest, fistulas
10.5 Cardiovascular Disease
- Total fat: <30% of="" energy;="" saturated="" fat=""><7%; trans="" fat="">
- Cholesterol: <200>
- Omega-3 fatty acids: 1 g/day EPA+DHA; fish 2 times/week
- Fiber: 25-30 g/day (soluble fiber reduces LDL)
- Sodium: <2.3 g/day;=""><1.5 g/day="" if="" hypertension/heart="">
- DASH diet: Emphasize fruits, vegetables, low-fat dairy, whole grains
- Mediterranean diet: Olive oil, nuts, fish, fruits, vegetables
Related Searches
Objective type Questions, Viva Questions, CheatSheet: Nutrition, Summary, video lectures, Previous Year Questions with Solutions, Exam, past year papers, pdf , Sample Paper, CheatSheet: Nutrition, CheatSheet: Nutrition, mock tests for examination, practice quizzes, ppt, Important questions, MCQs, study material, Semester Notes, Extra Questions, shortcuts and tricks, Free;






