Headache & Neurocutaneous Disorders - Free MCQ Practice Test with solutions,
MCQ Practice Test & Solutions: Test: Headache & Neurocutaneous Disorders (15 Questions)
You can prepare effectively for NEET PG Medicine with this dedicated MCQ Practice Test (available with solutions) on the important topic of "Test: Headache & Neurocutaneous Disorders". These 15 questions have been designed by the experts with the latest curriculum of NEET PG 2026, to help you master the concept.
Test Highlights:
- - Format: Multiple Choice Questions (MCQ)
- - Duration: 15 minutes
- - Number of Questions: 15
Sign up on EduRev for free to attempt this test and track your preparation progress.
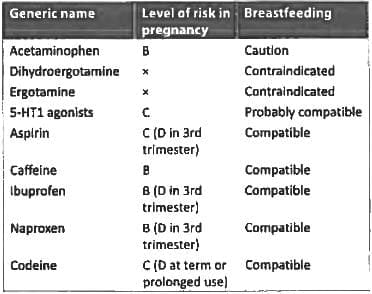
True statement regarding migraine in pregnancy? (JIPMER May 2018)
Detailed Solution: Question 1
Which of the following best describes a patient with classical migraine? (Recent Pattern Questions)
Detailed Solution: Question 2
A patient presents with sudden onset occipital headache, ataxia,vomiting and drowsiness and down beating nystagmus.What is the diagnosis? (JIPMER Nov 2014)
Detailed Solution: Question 3
A 22-yrs old man present with history of headache for 6 months which is mainly on frontal region occasionally associated with nausea He has been taking paracetamol 3g per day hydroxycodeine 50 mg 3 times a day and aspirin 300 mg 3 times a day for headache but only with temporary relief from symptoms no focal signs on neurological examinations he also has history of depression and is on treatment for 2 year with paroxetine now What is the diagnosis? (JIPMER Nov 2014)
Detailed Solution: Question 4
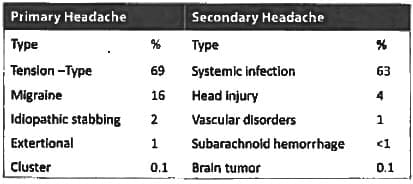
All of the following are causes of primary headache EXCEPT: (Recent Question 2015-16)
Detailed Solution: Question 5
A 65 yr old lady underwent mastectomy. 6 months later she developed headache with pain at temple region with ESR = 55mm fall in 1 st hour. Diagnosis? (JIPMER 2014)
Detailed Solution: Question 6
Sumatriptan is contraindicated in all except: (Recent Pattern 2014/15)
Detailed Solution: Question 7
A 70 year old retired Military person with good previous medical record complains of bi-temporal headache which is decreased in lying down position. He states that he gets relief by giving pressure over bilateral temples. The patient also complains of loss of appetite with feeling feverish. The most probable diagnosis is: (AIIMS Nov 2012)
Detailed Solution: Question 8
All are criteria for NF-1 except? (Recent Pattern 2018)
Detailed Solution: Question 9
Schwannoma of spinal nerve roots is seen in? (Recent Question 2016-17)
Detailed Solution: Question 10
Lisch nodules are seen in which of the following conditions? (UPSC 2015)
Detailed Solution: Question 11
A 6-year old child with port wine stain, mental retardation and recurrent focal seizures. All are true about the condition except?
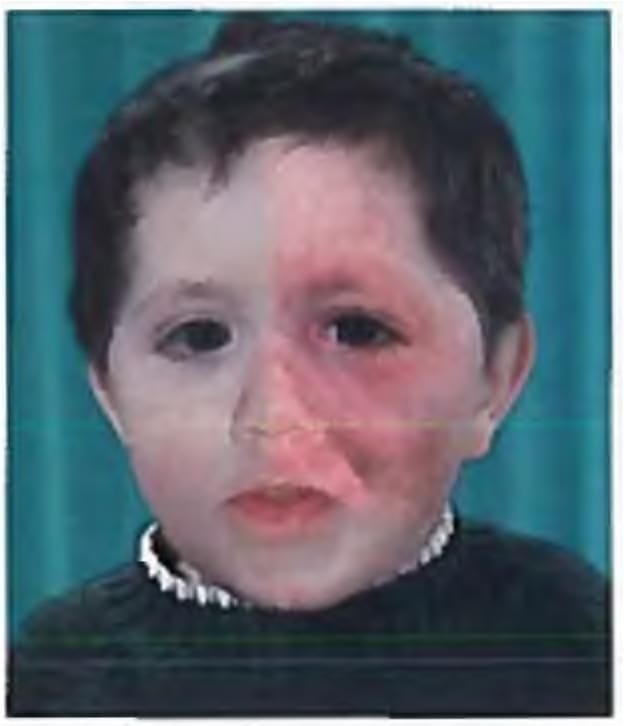

Detailed Solution: Question 12
Not seen in tuberous sclerosis (AIIMS Nov 14)
Detailed Solution: Question 13
All of the following are true about von Hippel Lindau syndrome except? (Recent Pattern 2014/15)
Detailed Solution: Question 14
Tuberculosis sclerosis is associated with all except: (APPG 2014)
Detailed Solution: Question 15
56 docs|64 tests |