Bleeding from GIT & Diseases of Esophagus- 1 - Free MCQ Practice Test
MCQ Practice Test & Solutions: Test: Bleeding from GIT & Diseases of Esophagus- 1 (20 Questions)
You can prepare effectively for NEET PG Medicine with this dedicated MCQ Practice Test (available with solutions) on the important topic of "Test: Bleeding from GIT & Diseases of Esophagus- 1". These 20 questions have been designed by the experts with the latest curriculum of NEET PG 2026, to help you master the concept.
Test Highlights:
- - Format: Multiple Choice Questions (MCQ)
- - Duration: 20 minutes
- - Number of Questions: 20
Sign up on EduRev for free to attempt this test and track your preparation progress.
The test shown below has been performed on a stool sample producing blue colour. Comment on the test being done. GIT/ bleeding from git (Recent Question 2019)
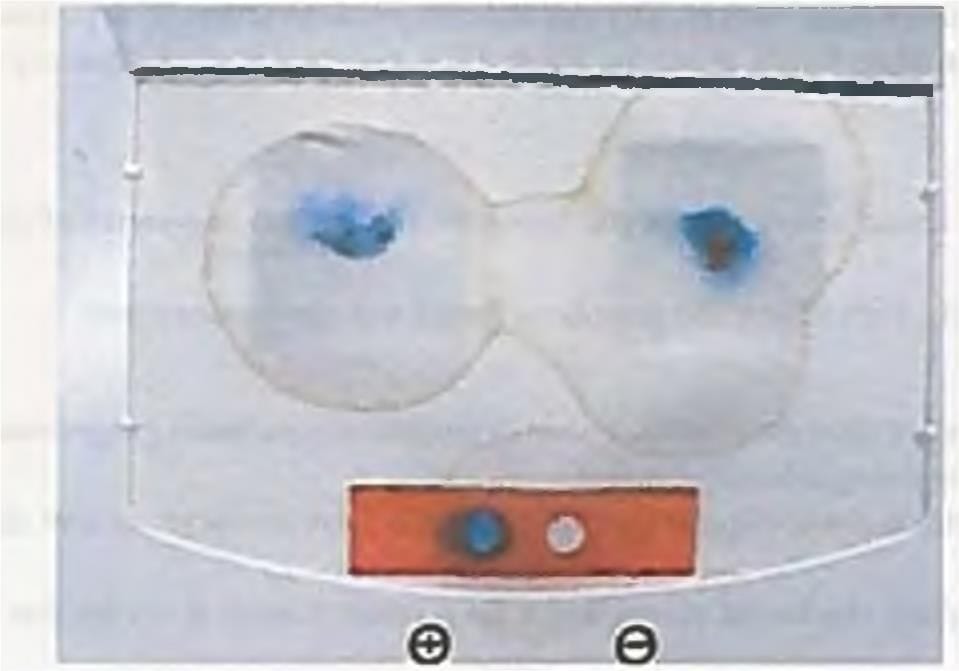

Detailed Solution: Question 1
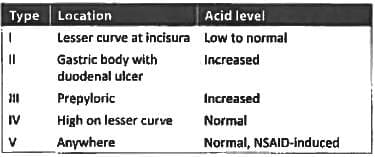
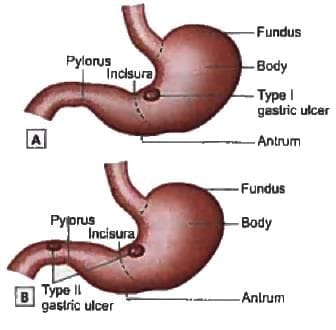
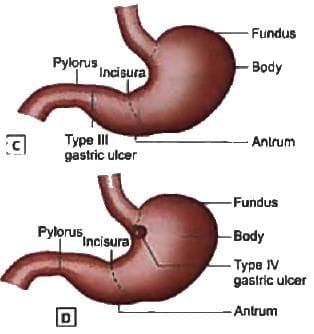
Which is the most common site for chronic gastric ulcer? (Recent Pattern 2018)
Detailed Solution: Question 2
A patient presents with complaints of fever and abdominal distention. He is having history of bloody diarrhoea off and on for previous 6 months. X ray abdomen is shown below. What is the diagnosis? (AIIMS May 2017)
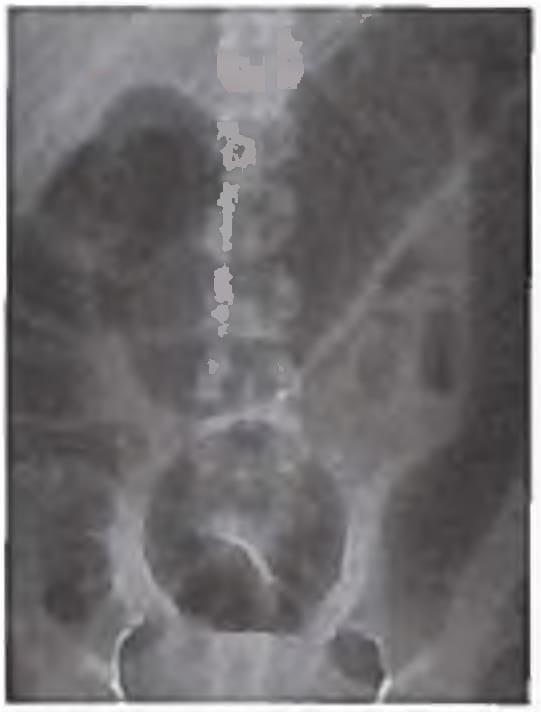

Detailed Solution: Question 3
All are true about persistent calibre artery except? (Recent Question 2016-17)
Detailed Solution: Question 4
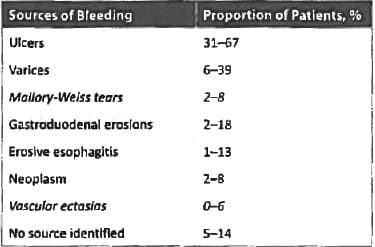
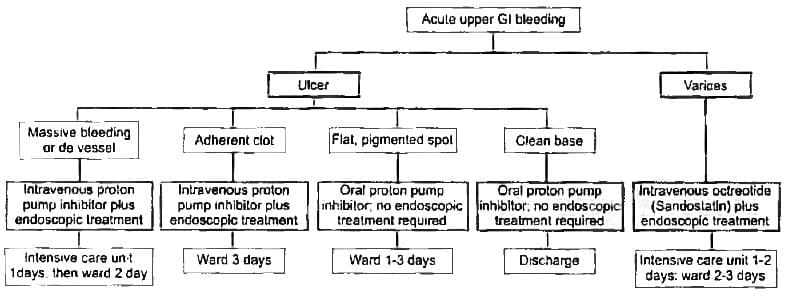
Among the following the least common cause of acute upper GI bleeding is? (APPG 2015)
Detailed Solution: Question 5
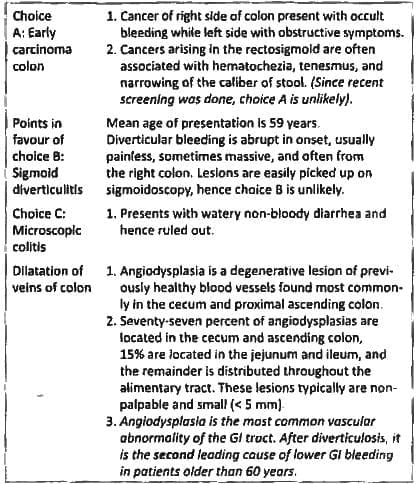
50 year old man became dizzy while passing stool and noticed fresh blood in stool. Previous stool examination for routine screening of carcinoma colon was normal. What is the most likely cause of bleed? (AIIMS Nov 2014)
Detailed Solution: Question 6
Which indicates least chances of re-bleeding after hematemesis episode: (Recent Pattern 2014-15)
Detailed Solution: Question 7
Most common site of dieulafoys lesion is: (Recent Pattern 2015-16)
Detailed Solution: Question 8
Most common cause of hematochezia in children? (Recent Pattern 2014-15)
Detailed Solution: Question 9
Rockall score is used for prognosis of patients of: (Recent Pattern 2014-15)
Detailed Solution: Question 10
Feline Oesophagus is seen in? (Recent Pattern 2018)
Detailed Solution: Question 11
Which is the best investigation for Dysphagia Lusoria? (Recent Question 2016-17)
Detailed Solution: Question 12
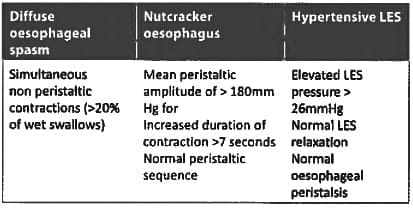
Diffuse esophageal spasm is best diagnosed by? (Bihar PG 2015)
Detailed Solution: Question 13
Diffuse oesophageal spasm treatment is? (JIPMER Nov 2015)
Detailed Solution: Question 14
All of the following is true regarding G.E.R.D except? (JIPMER Nov 2014)
Detailed Solution: Question 15
Incorrect about Zenkers diverticulum? (Recent Question 2015-16)
Detailed Solution: Question 16
Identify the endoscopic image? (Recent Question 2017)
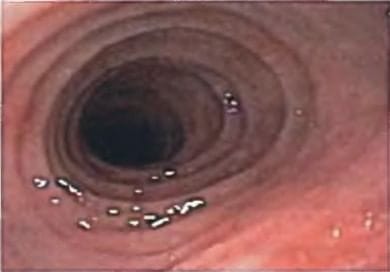

Detailed Solution: Question 17
Gold standard test for achalasia cardia? (Recent 2015-16)
Detailed Solution: Question 18
Which of the following is located in Laimer's triangle: (Recent Pattern 2014-15)
Detailed Solution: Question 19
Esophageal tear is best detected with: (Recent Pattern 2014-15)
Detailed Solution: Question 20
50 docs|64 tests |