Inflammatory Bowel Disease, Premalignant Lesions of GIT & Diarrhea - Free
MCQ Practice Test & Solutions: Test: Inflammatory Bowel Disease, Premalignant Lesions of GIT & Diarrhea (25 Questions)
You can prepare effectively for NEET PG Topic Wise MCQs for NEET PG with this dedicated MCQ Practice Test (available with solutions) on the important topic of "Test: Inflammatory Bowel Disease, Premalignant Lesions of GIT & Diarrhea". These 25 questions have been designed by the experts with the latest curriculum of NEET PG 2026, to help you master the concept.
Test Highlights:
- - Format: Multiple Choice Questions (MCQ)
- - Duration: 25 minutes
- - Number of Questions: 25
Sign up on EduRev for free to attempt this test and track your preparation progress.
What is the earliest radiological finding of ulcerative colitis on single contrast barium enema? (Recent Question 2016-17)
Detailed Solution: Question 1
DOC of acute exacerbation of ulcerative colitis? (Recent 2015-16)
Detailed Solution: Question 2
All are complications of ulcerative colitis, except: (Recent Pattern 2014-15)
Detailed Solution: Question 3
Best screening test for Crohn's disease is: (Recent Pattern 2014-15)
Detailed Solution: Question 4
Invariably involved site in ulcerative colitis: (Recent Pattern 2014-15)
Detailed Solution: Question 5
Treatment of choice in intractable ulcerative colitis: (Recent Pattern 2014-15)
Detailed Solution: Question 6
Treatment of choice in ulcerative colitis is: (Recent Pattern 2014-15)
Detailed Solution: Question 7
Best treatment of refractory peri-anal fistula in crohn's disease: (Recent Pattern 2014-15)
Detailed Solution: Question 8
Which of the following is the established biological therapy for Crohn’s disease? (Recent Pattern 2014-15)
Detailed Solution: Question 9
A highly sensitive and specific marker for detecting intestinal inflammation in ulcerative colitis is? (APPG 2014)
Detailed Solution: Question 10
Ulcterative colitis associated features include all, except: (Recent Pattern 2014-15)
Detailed Solution: Question 11
Chronic inflammatory bowel disease is associated with: (Recent Pattern 2014-15)
Detailed Solution: Question 12
Mutation of STK 11 and LKB 1 gene is associated with? (JIPMER 2014)
Detailed Solution: Question 13
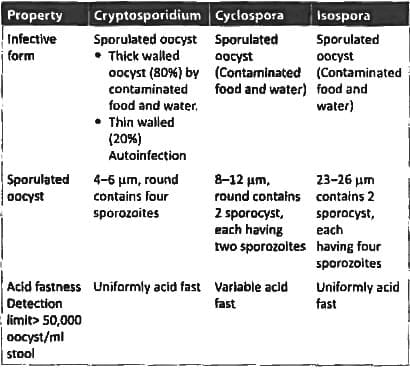
A known HIV positive patient on cART presents with diarrhea of 6 months duration. Stoll microscopy shows cysts of 10-30 um and kinyoun stain positive. What is the probable diagnosis? (AIIMS May 2018)
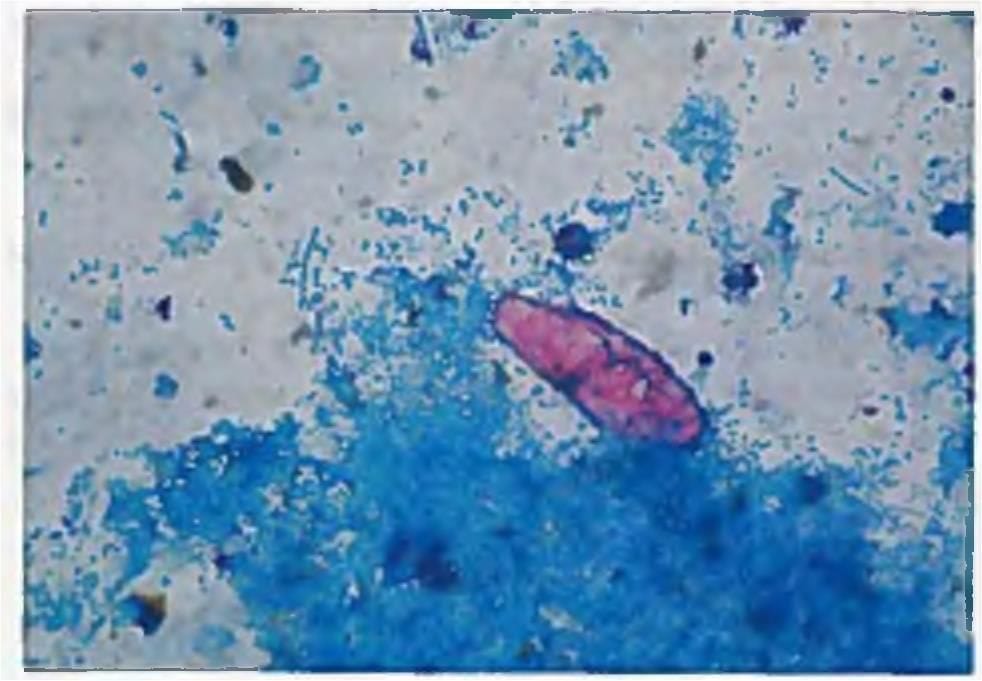

Detailed Solution: Question 14
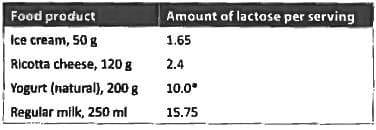
A 22-year old presents with diarrhea and intolerance to dairy products. On investigation he was found to have lactose deficiency. Agent least likely to cause lactose intolerance among these is? (AIIMS May 2018)
Detailed Solution: Question 15
In a hospitalized patient on multiple antibiotics with diarrhea, the best method of diagnosis for Clostridium difficile infection is? (AIIMS Nov 2017)
Detailed Solution: Question 16
All are features of bile acid diarrhoea except? (Recent Question 2016-17)
Detailed Solution: Question 17
All are diagnostic criteria for irritable bowel syndrome except? (Recent Question 2016-17)
Detailed Solution: Question 18
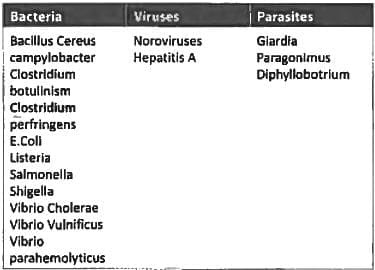
Most common cause for diarrhoea in adults associated with intake of Shell fish? (AIIMS Nov 2015)
Detailed Solution: Question 19
Which diarrhea decreases after prolonged fasting? (Recent 2015-16)
Detailed Solution: Question 20
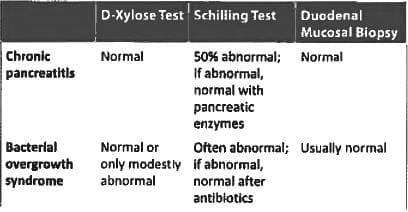
A patient with chronic diarrhoea with abnormal D-xylose & Schilling test. What could be the diagnosis: (Recent Pattern 2014-15)
Detailed Solution: Question 21
Diabetes induced diarrhea is best managed by which of the following? (Recent Pattern 2014-15)
Detailed Solution: Question 22
Patient with congenital lactose deficiency will experience distension, flatulence and diarrhea on ingestion of: (Recent Pattern 2014-15)
Detailed Solution: Question 23
All cause diarrhea except? (Recent Pattern 2014-15)
Detailed Solution: Question 24
30 year male with chronic diarrhoea, anemia. Most likely associated with: (AIIMS May 07)
Detailed Solution: Question 25