Natural Hazards and Disasters- 1 | Geography for UPSC CSE PDF Download
INTRODUCTION
INTRODUCTION
Disruption on a massive scale, either natural or man-made, occurring in short or long periods is termed as Disaster. Disaster management in India has been an important point of discussion owing to frequent natural disasters ranging from earthquakes, floods, drought, etc.
Loss of life and property due to these disasters have been steadily mounting throughout the world due to inadequate technology to combat disasters, rise in population, climate change, and continuing ecological degradation. The global efforts to manage disasters have proven to be insufficient to match the frequency and magnitude of natural disasters.
What is a Disaster?
A disaster is defined as a disruption on a massive scale, either natural or man-made, occurring in short or long periods. Disasters can lead to human, material, economic or environmental hardships, which can be beyond the bearable capacity of the affected society. As per statistics, India as a whole is vulnerable to 30 different types of disasters that will affect the economic, social, and human development potential to such an extent that it will have long-term effects on productivity and macro-economic performance.
The various disaster-prone zones in India can be inferred from the map below:
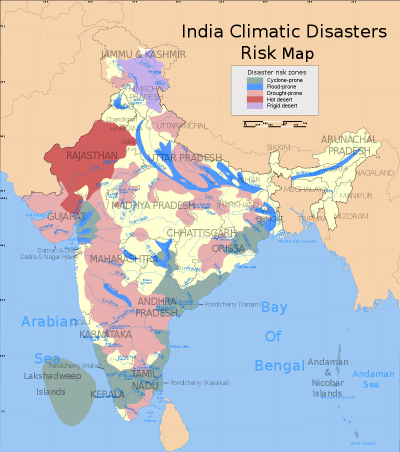
Disasters can be classified into the following categories:
- Water and Climate Disaster: Flood, hail storms, cloudburst, cyclones, heat waves, cold waves, droughts, hurricanes.
- Geological Disaster: Landslides, earthquakes, volcanic eruptions, tornadoes
- Biological Disaster: Viral epidemics, pest attacks, cattle epidemic, and locust plagues
- Industrial Disaster: Chemical and industrial accidents, mine shaft fires, oil spills,
- Nuclear Disasters: Nuclear core meltdowns, radiation poisoning
- Man-made disasters: Urban and forest fires, oil spill, the collapse of huge building structures
What is Disaster Management?
Per the Disaster Management Act of 2005 defines Disaster Management as an integrated process of planning, organizing, coordinating and implementing measures which are necessary for-
1. Prevention of threat of any disaster
2. Reduction of risk of any disaster or its consequences
3. Readiness to deal with any disaster
4. Promptness in dealing with a disaster
5. Assessing the severity of the effects of any disaster
6. Rescue and relief
7. Rehabilitation and Reconstruction
Agencies involved in Disaster Management
- National Disaster Management Authority (NDMA): The National Disaster Management Authority, or the NDMA, is an apex body for disaster management, headed by the Prime Minister of India. It is responsible for the supervision, direction, and control of the National Disaster Response Force (NDRF).
- National Executive Committee (NEC): The NEC is composed of high profile ministerial members from the government of India that include the Union Home Secretary as Chairperson, and the Secretaries to the Government of India (GoI)like Ministries/Departments of Agriculture, Atomic Energy, Defence, Drinking Water Supply, Environment and Forests, etc. The NEC prepares the National Plan for Disaster Management as per the National Policy on Disaster Management.
- State Disaster Management Authority (SDMA): The Chief Minister of the respective state is the head of the SDMA.The State Government has a State Executive Committee (SEC) which assists the State Disaster Management Authority (SDMA) on Disaster Management.
- District Disaster Management Authority (DDMA): The DDMA is headed by the District Collector, Deputy Commissioner or District Magistrate depending on the situation, with the elected representatives of the local authority as the Co-Chairperson. The DDMA ensures that the guidelines framed by the NDMA and the SDMA are followed by all the departments of the State Government at the District level and the local authorities in the District.
- Local Authorities: Local authorities would include Panchayati Raj Institutions (PRI), Municipalities, District and Cantonment 11 Institutional and Legal Arrangements Boards, and Town Planning Authorities which control and manage civic services.
Now let’s have a look at some of the types of disasters and the means to combat them.
Biological Disasters
Definition: The devastating effects caused by an enormous spread of a certain kind of living organism that may spread disease, viruses, or an infestation of plant, animal, or insect life on an epidemic or pandemic level.
- Epidemic Level – Indicates a disaster that affects many people in a given area or community.
- Pandemic Level – Indicates a disaster that affects a much larger region, sometimes an entire continent or even the whole planet. For example, the recent H1N1 or Swine Flu pandemic.
Biological Disasters
1. The nodal agency for handling epidemics – Ministry of Health and Family Welfare
- Decision-making
- Advisory body
- Emergency medical relief providing
2. The primary responsibility of dealing with biological disasters is with the State Governments. (Reason – Health is a State Subject).
3. The nodal agency for investigating outbreaks – National Institute of Communicable Diseases (NICD)
4. Nodal ministry for Biological Warfare – Ministry of Home Affairs (Biological warfare is the use of biological agents as an act of war)
Biological Disasters – Classifications
Charles Baldwin developed the symbol for biohazard in 1966.
The US Centres for Disease Control classifies biohazards into four biosafety levels as follows:
- BSL-1: Bacteria and Viruses including Bacillus subtilis, some cell cultures, canine hepatitis, and non-infectious bacteria. Protection is only facial protection and gloves.
- BSL-2: Bacteria and viruses that cause only mild disease to humans, or are difficult to contract via aerosol in a lab setting such as hepatitis A, B, C, mumps, measles, HIV, etc. Protection – use of autoclaves for sterilizing and biological safety cabinets.
- BSL-3: Bacteria and viruses causing severe to fatal disease in humans. Example: West Nile virus, anthrax, MERS coronavirus. Protection – Stringent safety protocols such as the use of respirators to prevent airborne infection.
- BSL-4: Potentially fatal (to human beings) viruses like Ebola virus, Marburg virus, Lassa fever virus, etc. Protection – use of a positive pressure personnel suit, with a segregated air supply.
Legislations for prevention of Biohazards in India
The following legislations have been enacted in India for the prevention of biohazards and implementation of protective, eradicative and containing measures when there is an outbreak:
- The Water (Prevention and Control of Pollution) Act, 1974
- The Air (Prevention and Control of Pollution) Act, 1981
- The Environmental (Protection) Act, 1986 and the Rules (1986)
- Disaster Management Act 2005, provides for the institutional and operational framework for disaster prevention, mitigation, response, preparedness, and recovery at all levels.
Prevention of Biological Hazards
The basic measure to prevent and control biohazards is the elimination of the source of contamination. Some of the prevention methods are as follows:
Preventive Measures for workers in the field (Medical)
- Engineering controls – to help prevent the spread of such disasters including proper ventilation, installing negative pressure, and usage of UV lamps.
- Personal hygiene – washing hands with liquid soap, proper care for clothes that have been exposed to a probably contaminated environment.
- Personal protection equipment – masks, protective clothing, gloves, face shield, eye shield, shoe covers.
- Sterilization – Using ultra heat or high pressure to eliminate bacteria or using biocide to kill microbes.
- Respiratory protection – surgical masks, respirators, powered air-purifying respirators (PAPR), air-supplying respirators.
Prevention of Biological Hazards (Environmental Management)
Safe water supply, proper maintenance of sewage pipelines – to prevent waterborne diseases such as cholera, typhoid, hepatitis, dysentery, etc.
Awareness of personal hygiene and provision for washing, cleaning, bathing, avoiding overcrowding, etc.
Vector control:
Environmental engineering work and generic integrated vector control measures.
Water management, not permitting water to stagnate and collect and other methods to eliminate breeding places for vectors.
Regular spraying of insecticides, outdoor fogging, etc. for controlling vectors.
Controlling the population of rodents.
Post-disaster Epidemics Prevention
The risk of epidemics is increased after any biological disaster.
Integrated Disease Surveillance Systems (IDSS) monitors the sources, modes of diseases spreading, and investigates the epidemics.
Detection and Containment of Outbreaks
This consists of four steps as given under:
1. Recognizing and diagnosing by primary healthcare practitioners.
2. Communicating surveillance information to public health authorities.
3. Epidemiological analysis of surveillance data
4. Public health measures and delivering proper medical treatment.
Legal Framework for Biological Disasters
1. The Epidemic Diseases Act was enacted in the year 1897.
2. This Act does not provide any power to the center to intervene in biological emergencies.
3. It has to be substituted by an Act that takes care of the prevailing and foreseeable public health needs including emergencies such as BT attacks and the use of biological weapons by an adversary, cross-border issues, and international spread of diseases.
4. It should give enough powers to the central and state governments and local authorities to act with impunity, notify affected areas, restrict movement or quarantine the affected area, enter any premises to take samples of suspected materials, and seal them.
5. The Act should also establish controls over biological sample transfer, biosecurity and biosafety of materials/laboratories.
Institutional Framework
In the Ministry of Health & Family Welfare (MoH&FW), public health needs to be accorded high priority with a separate Additional Directorate General of Health and Sanitation (DGHS) for public health. In some states, there is a separate department of public health. States that do not have such arrangements will also have to take initiatives to establish such a department.
Operational Framework
At the national level, there is no policy on biological disasters. The existing contingency plan of MoH&FW is about 10 years old and needs extensive revision. All components related to public health, namely apex institutions, field epidemiology, surveillance, teaching, training, research, etc., need to be strengthened.
At the operational level, Command and Control (C&C) are identifiable clearly at the district level, where the district collector is vested with certain powers to requisition resources, notify a disease, inspect any premises, seek help from the Army, state or center, enforce quarantine, etc. However, there is no concept of an incident command system wherein the entire action is brought under the ambit of an incident commander with support from the disciplines of logistics, finance, and technical teams, etc. There is an urgent need for establishing an incident command system in every district.
There is a shortage of medical and paramedical staff at the district and sub-district levels. There is also an acute shortage of public health specialists, epidemiologists, clinical microbiologists, and virologists.
Biosafety laboratories are required for the prompt diagnosis of the agents for the effective management of biological disasters. There is no BSL-4 laboratory in the human health sector. BSL- 3 laboratories are also limited. Major issues remain regarding biosecurity, the indigenous capability of preparing diagnostic reagents, and quality assurance.
Lack of an Integrated Ambulance Network (IAN). There is no ambulance system with advanced life-support facilities that are capable of working in biological disasters.
State-run hospitals have limited medical supplies. Even in normal situations, a patient has to buy medicines. There is a lack of stockpile of drugs, important vaccines like anthrax vaccine, PPE, or diagnostics for surge capacity. In a crisis, there is further incapacitation due to tedious procurement procedures.
- National Disaster Response Force (NDRF):- The command and supervision of the NDRF would be under the Director-General of Civil Defence and National Disaster Response Force selected by the Central Government. Currently, the NDRF comprises of eight battalions who will be positioned at different locations as per the requirements.
|
175 videos|619 docs|192 tests
|
FAQs on Natural Hazards and Disasters- 1 - Geography for UPSC CSE
| 1. What are natural hazards and disasters? |  |
| 2. How can natural hazards be predicted or detected? |  |
| 3. What are the impacts of natural hazards and disasters? |  |
| 4. How can individuals and communities prepare for natural hazards and disasters? |  |
| 5. What are the measures taken to mitigate the impacts of natural hazards and disasters? |  |
















