Human Diseases
Transmission of Diseases
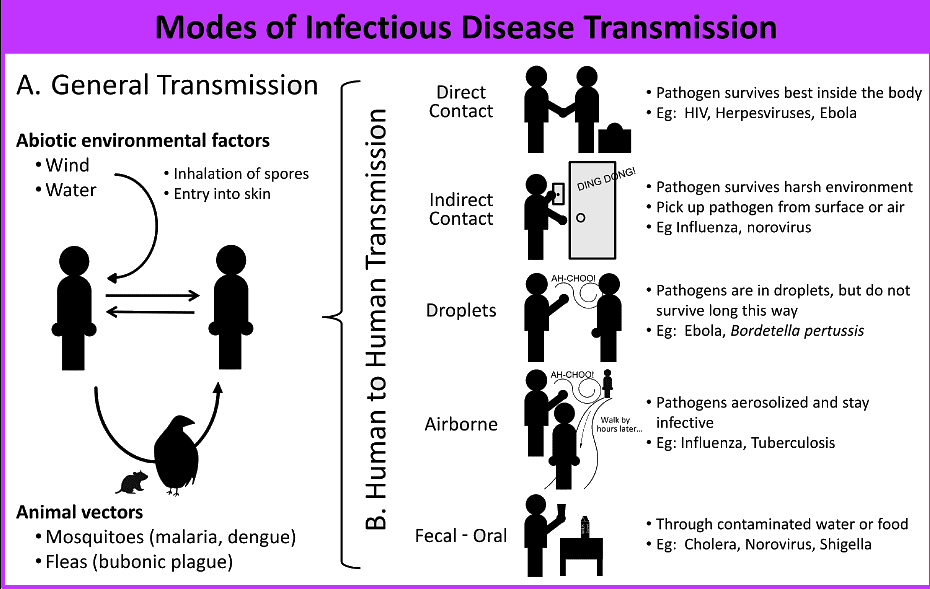
Diseases move from an infected host to a susceptible individual by defined routes. Understanding these routes helps in prevention, control and public-health planning. The four primary routes of transmission are airborne, contact, vehicle and vector-borne transmission.
- Airborne transmission
Pathogens are carried on small particles or droplet nuclei that remain suspended in the air for long periods and can travel distances. Droplet nuclei are small enough to be inhaled deep into the respiratory tract and can remain infectious for hours in dry, enclosed environments. The pathogens themselves do not grow in air but are transported by these particles. Common examples include chickenpox, influenza, measles, mumps, some forms of viral pneumonia, diphtheria, tuberculosis and certain kinds of meningitis. Preventive measures include vaccination where available, good ventilation, respiratory hygiene (covering coughs and sneezes), wearing masks in outbreaks, and isolation of infectious patients.
- Contact transmission
Pathogens spread through direct physical contact between an infected individual and a susceptible person. This includes touching, kissing, sexual contact, and transmission from mother to foetus across the placenta or during childbirth. Examples are herpes infections, skin boils transmitted via secretions or lesions, many staphylococcal infections, and blood-borne infections such as HIV/AIDS and syphilis. Prevention relies on hand hygiene, safe sexual practices, screening of blood and blood products, and infection control in health-care settings.
- Vehicle transmission
Non-living objects or substances (called vehicles) carry infectious agents from source to host. Common vehicles are contaminated food, water, utensils, bedding, surgical instruments and needles. Bacterial causes of foodborne illness include Staphylococcus aureus and Bacillus cereus; waterborne and foodborne pathogens include Escherichia coli, Vibrio cholerae, Salmonella typhi and toxigenic bacteria such as Clostridium difficile in health-care settings. Prevention includes safe food handling, clean water supply, sterilisation of medical instruments, single-use needles, and proper disinfection of fomites (inanimate contaminated objects).
- Vector-borne transmission
A vector is a living organism that carries a pathogen between hosts. Vectors can be vertebrates (for example dogs or bats that carry rabies) or arthropods such as mosquitoes, ticks, fleas and flies. Some vectors transmit pathogens without internal change in the agent (mechanical or harborage transmission); others allow part of the pathogen life cycle to occur inside the vector (biological transmission). For example, flies may mechanically transfer Shigella from faeces to food, while mosquitoes biologically transmit Plasmodium species that cause malaria. Control measures include vector control (insecticides, environmental sanitation), bed nets, vaccination where available and reducing vector breeding sites.
Non-Communicable Diseases (NCDs)
Non-communicable diseases are chronic conditions that are not passed from person to person. They arise from a combination of genetic, physiological, environmental and behavioural risk factors and generally progress slowly. The major groups are cardiovascular diseases (heart attacks and strokes), cancers, chronic respiratory diseases (for example chronic obstructive pulmonary disease and asthma), and diabetes. Common risk factors include tobacco use, unhealthy diet, physical inactivity, harmful use of alcohol and air pollution.
Prevention and control of NCDs emphasise population-level interventions (tobacco control, healthy food policies, pollution reduction), early detection (screening), clinical management (medication, lifestyle modification) and rehabilitation. Many NCDs are manageable when detected early and treated appropriately; public awareness and primary-care access are central to reducing their burden.
Classification of Diseases
Diseases are classified in several ways for study and clinical practice. Common approaches are by cause (infectious vs non-infectious), by the organ system involved, or by genetic/chromosomal origin. A concise classification useful for general awareness:
- Diseases caused by microbes
Includes infections produced by protozoa, viruses, fungi and bacteria. Each group has characteristic agents, modes of transmission and prevention strategies such as sanitation, vaccination and antimicrobial therapy.
- Diseases of sex chromosomes and chromosomal disorders
Disorders arising from abnormalities in sex chromosomes (X or Y) or in autosomes; these produce characteristic syndromes and inherited conditions. Examples include Turner syndrome, Klinefelter syndrome, X-linked conditions such as haemophilia and colour blindness, and autosomal trisomies such as Down syndrome (trisomy 21) and Patau syndrome (trisomy 13).
- Diseases of different organ systems
Grouped by the primary organ system affected, for example genetic disorders, nervous system diseases, heart diseases, blood disorders, respiratory disorders, skeletal disorders and kidney diseases. This clinical classification helps diagnosis and treatment planning.
Diseases Caused by Microbes
Protozoan diseases
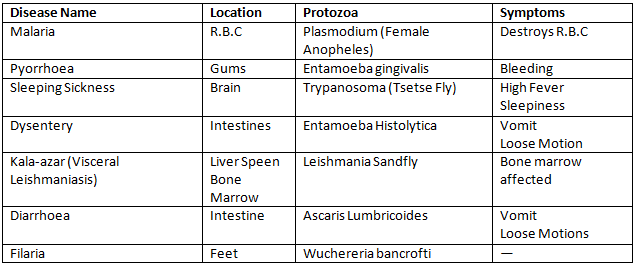
Protozoa are single-celled eukaryotic organisms that can cause human disease. Notable examples are malaria (caused by Plasmodium species, transmitted by Anopheles mosquitoes), amoebiasis (caused by Entamoeba histolytica, transmitted through contaminated food and water) and giardiasis (caused by Giardia lamblia). Control strategies include vector control for malaria, safe water and food, sanitation and targeted drug treatment.
Viral diseases
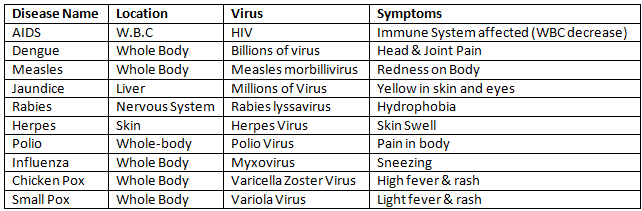
Viruses are submicroscopic infectious agents that require host cells to replicate. Common viral diseases include influenza, chickenpox, measles, mumps, hepatitis, and infections caused by HIV. Vaccination, antiviral drugs where available, infection control and public-health surveillance are the main prevention and control measures.
Fungal diseases
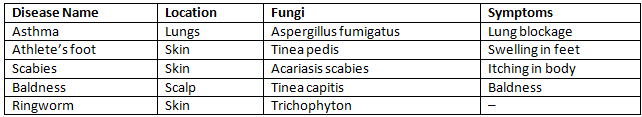
Fungi cause superficial infections (skin, nails), mucosal infections and, less commonly, systemic disease in immunocompromised persons. Examples include athlete's foot, ringworm, and candidiasis. Antifungal medications, good hygiene and treating underlying risk factors form the basis of management.
Bacterial diseases
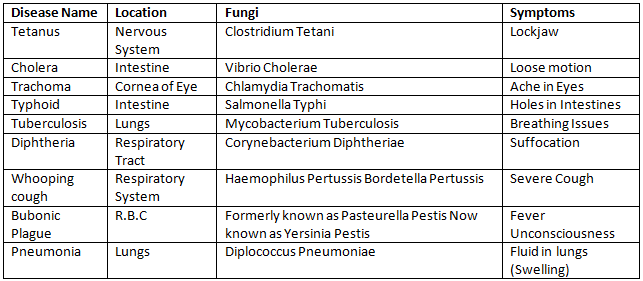
Bacteria are single-celled prokaryotes responsible for many communicable diseases: cholera (Vibrio cholerae), typhoid (Salmonella typhi), tuberculosis (Mycobacterium tuberculosis), staphylococcal skin infections and bacterial pneumonia. Treatment commonly uses antibiotics, but rising antibiotic resistance highlights the need for rational drug use, vaccination (where available), sanitation and infection control in health-care settings.
Diseases of Sex Chromosomes and Chromosomal Disorders
- Turner syndrome
Caused by complete or partial absence of one X chromosome in a female (commonly noted as 45,X). Affected individuals have short stature, gonadal dysgenesis (underdeveloped ovaries) leading to infertility, and may have cardiovascular or renal anomalies. Management focuses on hormone replacement, growth monitoring and supportive care.
- Klinefelter syndrome
Occurs in males with an extra X chromosome (most commonly 47,XXY). Features include small testes, reduced fertility or infertility, taller stature, and sometimes learning difficulties. Management includes endocrinology follow-up and fertility counselling.
- X-linked conditions (examples)
Colour blindness - most commonly red-green colour deficiency due to a gene defect on the X chromosome; more frequent in males. Haemophilia - an X-linked bleeding disorder caused by deficiency of clotting factors (for example factor VIII in haemophilia A), leading to excessive bleeding; treatment is replacement therapy with clotting factor concentrates or plasma.
- Autosomal chromosomal disorders (examples)
Down syndrome (trisomy 21) is caused by an extra copy of chromosome 21 and presents with intellectual disability, characteristic facial features, short stature and variable congenital anomalies. Patau syndrome (trisomy 13) is caused by an extra chromosome 13 and leads to severe intellectual disability, multiple congenital defects (such as cleft lip/palate) and high infant mortality. These are chromosomal disorders affecting autosomes rather than sex chromosomes; care is multidisciplinary and supportive.
Diseases of Different Organ Systems
- Genetic diseases
Inherited conditions caused by changes in DNA. They include chromosomal disorders (numerical or structural abnormalities of chromosomes) and Mendelian single-gene disorders (autosomal dominant, autosomal recessive and X-linked conditions). Diagnosis uses family history, genetic testing and counselling. Examples include cystic fibrosis and thalassemia.
- Nervous system diseases
Disorders affecting the brain, spinal cord and peripheral nerves. Causes may be structural (tumours, trauma), biochemical (neurotransmitter disorders), infectious (meningitis, encephalitis) or degenerative (Parkinson's, Alzheimer's). Presentations include seizures, paralysis, sensory loss and cognitive changes; management depends on the cause and may include medication, surgery and rehabilitation.
- Heart diseases
Includes coronary artery disease, cardiomyopathies, valvular diseases and congenital heart defects. Risk factors include hypertension, smoking, high cholesterol, diabetes, sedentary lifestyle and poor diet. Prevention and treatment use lifestyle modification, medicines, interventional cardiology and surgery.
- Blood diseases
Disorders of blood cells and clotting, for example anaemia, sickle cell anaemia, thalassemia, lymphomas and haemophilia. Diagnosis uses blood counts, haemoglobin studies and bone marrow examination. Treatment varies from nutritional supplementation to transfusions, chelation therapy and specialised medications.
- Respiratory diseases
Range from common infections such as the common cold and bronchitis to chronic conditions like asthma, chronic obstructive pulmonary disease (COPD) and lung cancer. Management includes tobacco control, vaccination, inhaled therapies, pulmonary rehabilitation and, where appropriate, surgery.
- Skeletal diseases
Disorders of bones, joints, cartilage, tendons and ligaments. Examples include osteoporosis (reduced bone density), osteoarthritis, tendinitis and spinal stenosis. Prevention addresses nutrition (calcium and vitamin D), exercise and avoiding risk factors; treatment ranges from physiotherapy to surgical interventions.
- Kidney diseases
The kidneys filter blood and remove waste; dysfunction leads to accumulation of toxins and fluid imbalance. Common disorders include renal hypertension, hydronephrosis, kidney stones and polycystic kidney disease. Management includes treating underlying causes, maintaining fluid and electrolyte balance, dialysis and transplantation in end-stage renal disease.
Cancer
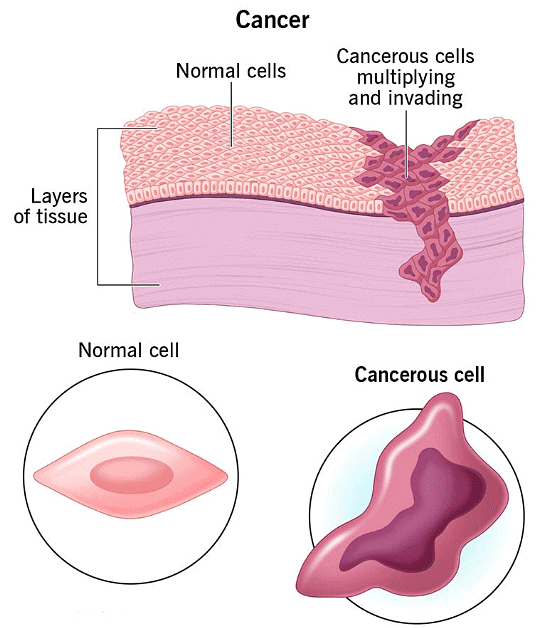
- Types of cancer
Cancer is the uncontrolled growth and spread of abnormal cells. Tumours may be benign (localised, do not invade surrounding tissues) or malignant (capable of invasion and metastasis - spread to distant sites). Cancers are named for the tissue of origin (for example carcinomas from epithelial tissue, sarcomas from connective tissue, leukaemias from blood-forming tissues).
- Causes and treatment
Carcinogenesis is multifactorial: tobacco and alcohol are major avoidable causes (tobacco for lung and oral cancers; alcohol for liver and other cancers); chemical exposures and occupational carcinogens increase risk; radiation and certain viruses (for example HPV, hepatitis B/C) are established causes. Treatments include surgery, chemotherapy, radiotherapy (radioisotopes such as Cobalt-60 are historically used in external beam therapy), hormone therapy, targeted biological therapies and emerging approaches like gene therapy. Choice of therapy depends on cancer type, stage and patient factors.
- Specific cancers and terms
Leukaemia - cancers of the blood-forming tissues resulting in abnormal proliferation of white blood cells. Sarcoma - cancers arising from connective tissues such as bone, cartilage and fat. Oncology is the branch of medicine that studies and treats cancer. Early detection, screening (where evidence supports it), risk-factor reduction and appropriate multidisciplinary treatment improve outcomes.
Summary: A clear understanding of modes of transmission, the distinction between infectious and non-infectious diseases, the role of microbes and genetics, and the principles of prevention and treatment is essential for effective public health and clinical care. Vaccination, sanitation, risk-factor control and timely clinical intervention remain the cornerstones of disease control.
FAQs on Human Diseases
| 1. What are some common examples of non-communicable diseases (NCDs)? |  |
| 2. How are diseases caused by microbes different from non-communicable diseases? |  |
| 3. What are some examples of diseases of sex chromosomes? |  |
| 4. Can you provide some examples of diseases that affect different organ systems in the body? |  |
| 5. How can cancer be classified in terms of its origin and behavior? |  |






