AIDS & Cancer | Biology Class 12 - NEET PDF Download
AIDS (Aquired Immuno Deficiency Syndrome)
AIDS or Acquired Immune Deficiency Syndrome is a disease caused by the HIV virus. In this condition, a person’s immune system becomes too weak to fight any kind of infection or disease. AIDS is usually the last stage of HIV infection; a stage where the body can no longer defend itself and thus spawns various diseases. AIDS, when untreated, leads to death.

It is not a congenital disease
Characterized by decrease in number of helper T-cells.
Also called slim disease
First detected in homosexual males in USA (1981) at Disease Control Centre Atlanta.
In India first AIDS case was reported in 1986 from Chennai.
Transmission of HIV
(i) Sexual route : due to multiple sex partners, prostetuters, homosexuality, artificial insemination (Probability < 1%).
(ii) Parenteral route : through blood contact due to unscreened blood transfusion, tattoeing, infected, poorly sterlized dental instruments.
(iii) Transplacental route = from mother to fetus = Vertical transmission, by placenta (33%) = From mother to infants = perinatal transmission, by colostrum.
Misconceptions Regarding AIDS
AIDS do not spread through more touch, physical contact, hugging, kissing, sharing meals, shaking hands, mosquito bites, coughing, sneezing looking after AIDS patients.
HIV spreads only through body fluids.
Pathogenicity of HIV
Structure of HIV
- The term HIV stands for human immunodeficiency virus, and the virus is oval in shape.
- The virus has a capsid nucleus, which contains the genetic material and is surrounded by a protein envelope.
- Many glycoprotein spikes are seen on the protein envelope.
- The outer section of a glycoprotein termed gp120 is linked to the inner component of the glycoprotein, gp41.
- Other proteins, such as Human Leucocyte Antigen, are found in the HIV envelope (HLA).
- Two helices of folded RNA molecules make up the HIV genome.
- The reverse transcriptase enzymes are present, and they are in charge of transforming RNA into DNA.
- There is also an enzyme called integrase, which aids in the introduction of the viral genome into the host cell.
Symptom of AIDS
As AIDS is a virus infection, the symptoms related to acute HIV infection can be similar to flu or other viral illnesses, like:
- Fever
- Muscle & Joint Pain
- Chilis
- Headaches
- Sore throat
- Night Sweats
- Red rashes
- Mouth sores
- Tiredness
- Swollen lymph glands
- Weakness
- Weight Loss
- Diarrhoea
Symptoms of late-stage HIV infection may include:
- Blurred vision
- Persistent or Chronic Diarrhea
- Dry cough
- Fever of above 37 degrees Centigrade (100 degrees Fahrenheit)
- Night Sweats
- Permanent tiredness
- Shortness of breath
- Swollen glands lasting for weeks
- Weight loss
- White spots on the tongue or mouth
Investigation of AIDS
Screening test : Enzyme linked immuno sorbent assay (ELISA)
- Confirmatory tests : Western blot test which detects antibodies, in patient's serum.
Treatment of AIDS
(i) Reverse transcriptase inhibitor = Zidovudin (previously called AZT), Stavudin, Trizivir, DDI (Didexymidine), Foscarnet, etc.
(ii) Protease inhibitor = Ritonavir, Nelfinavir, Sequinavir etc.
(iii) HAART (Highly Active Ant Retroviral Therapy) includes both reverse transcriptase inhibitor and protease inhibitor drugs.
Dr. David Ho. – Cocktal treatment of AIDS in 1993 and research in USA 1995, man of the year.
Note: Treatment is only partially effective, only prolong the life of the patients but cant prevent death, which is inevitable.
Prevention of AIDS
1. Education : NACO (National AIDS Control Organisation) has been set up under health family welfare ministry. (NGOs/ Non government organisation also playing their important role)
2. Screening of blood,
3. Ban on prostetution, Safer sex and awareness about to use of condoms.
4. Use of disposables
5. Sterlization of Ragors, blades and dental equipments.
6. AIDS patients need help and sympathy instead of being shunned by society.
It is a malody that can only be tackled by society and medical fraternity acting together to prevent spread of the disease.
Cancer
Uncontrolled, Abnormal and excessive mitotic division of cells is called cancer (Crab = cancer). Study of cancer is called oncology. These abnormal and undifferentiated cells are called cancerous cells.
Tumour or Neoplasm (New growth)
Types of Tumours
(a) Benign Tumour : capsulated, localized to the site of origin & does not spread to another parts of body, it is non metastatic, non-malignant, non-cancerous, Non invasive eg.:-
Bone tumour – Osteoma
Muscle tumour – Myoma
Lymph node tumour – Lymphoma
(b) Malignant Tumour (Malignant = Harmful) : Some of the cancerous cells detach from their origin place and spread to other parts of body by blood and lymph. Now the cancerous cells form fresh colonies there. This is called metastasis or sec. growth. This type of tumour is called metastatic or cancerous tumour. It is Invasive tumour. e.g. All malignant tumour are called cancers.
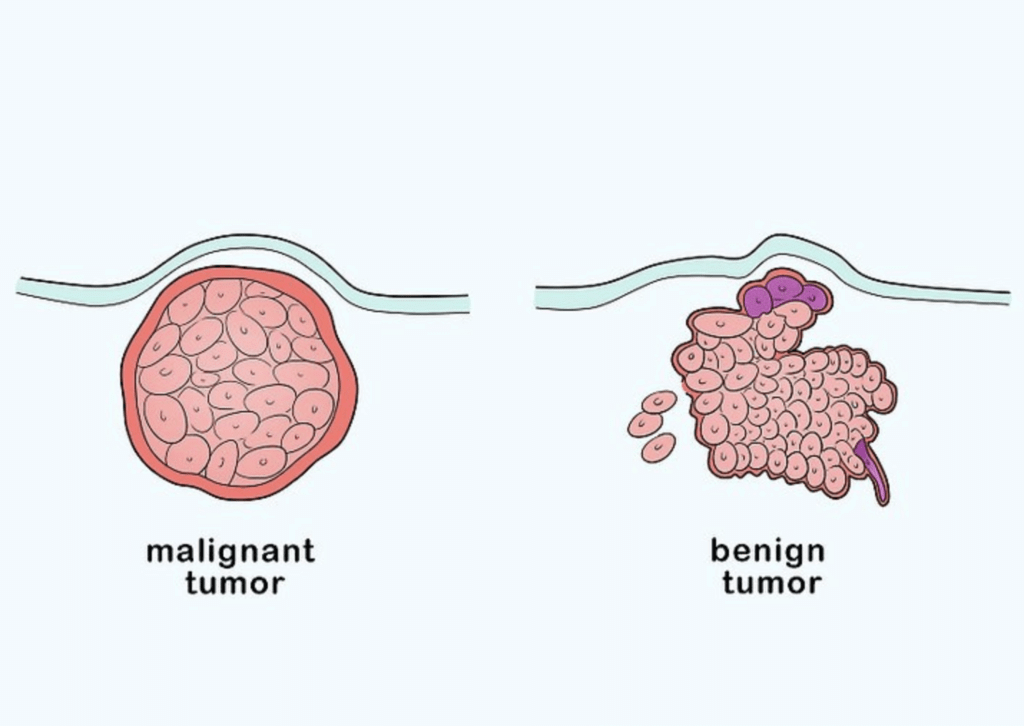
Cancer is Divided into 3 Classes on the Basis of Origin
(i) Carcinoma : This tumour originate from the Skin and epithelial tissue
eg :
(a) Brain carcinoma
(b) Oral carcinoma
(c) Gastric carcinoma
(d) Colon carcinoma
(e) Lung carcinoma
(f) Cervical carcinoma
(g) Adeno carcinona (gland tumour)
(h) Breast carcinoma
Carcinoma is most common type of tumour (85%)
Breast cancer in female and prostate cancer in males are common incidence in world. Lung cancer accounts for 31.1% of all cancer death in men and 25% in women.
Cervical (Uterine Cervix) cancer in females and oral cancer in males are common in India.
Melanoma –It is type of carcinomas. These are cancerous growths of melanocytes (a type of skin cells).
(ii) Sarcoma: This is tumour of mesodermal tissue.
eg.
Bone cancer – Osteosarcoma
Muscle cancer – Myosarcoma
Lymph node cancer – Lymphosarcoma.
(iii) Leukaemia (Leucocyte = W.B.C.) or Blood Cancer : This is cancer of white blood cells (WBC).
Chronic Myelogenous Leukaemia (CML): This fatal cancer occurs mainly due to reciprocal translocation between chromosome-22 (Philadelphia chromosome) and chromosome 9.
Burkitt's Lymphoma : This is a type of leukaemia which is produced due to reciprocal translocation between chromosome-8 and chromosome-14.
According to a rough estimate about 8 lakhs cases of cancer are detected in India every year out of which 4 lakhs succumb to death.
Normal mechanism of body growth – Normal cell division regulation by proto-oncogenes and it is suppressed by tumour surppressor gene.
Causes of Cancer
Chemical or physical agents that can cause cancer are known as carcinogen. Depending on their mode of action, carcinogens fall into the following main categories :
(i) Agents that can cause alterations in the genetic material (DNA), resulting in oncogenic transformation.
(ii) Agents that promote the proliferation of cells, which have already undergoes genetic alterations responsible for oncogenic transformation. These agents are called tumour promoter e.g. some growth factors and hormones.
(iii) Cancer causing DNA and RNA viruses (tumour viruses) have been shown to be associated with oncogenic transformation.
Transformation of a normal cell into cancer cell if the regulation is upset.
Cancer cells don't show contact inhibition phenomenon which is shown by normal cells (when normal cells contact with other cells they inhibit uncontrolled growth by activation of tumour suppressor gene of cells).
Carcinogen
Causative agent cancer - Carcinogen
(a) Chemical Factor : Tobacco and betal chewing causes oral cancer. Heavy smoking (N–Nitrosodimethylene) causes oral cancer, cancer of larynx and lungs. Combustion product of coal and pesticides, artificial flavour, sweetners, synthetic food, add flavour, hormonal imbalance in body cause cancer.
Hormonal imbalance or estrogen excess causes breast cancer. Urinary bladder cancer is common in dye workers.
Important carcinogens and the organs affected | ||
Carcinogens | Affected Organs | |
1. | Soot | Skin and lungs |
2. | Cigarrete smoke (N-ritrosodimethylene) | Lungs |
3. | Coaltar (3, 4-benzopyrine) | Skin and lungs |
4. | Aflatoxin (metabolic product of fungi) | Liver |
5. | Cadmium oxide | Prostate gland |
6. | Mustard gas (b) | Lungs |
7. | Asbestos | Lungs |
8. | Nickel and Chromium compounds | Lungs, Larynx |
9. | Vinyl chloride | Liver |
10. | Diethy lstebesterol (DES) | Vagina |
11. | Benzene | Blood, Bone marrow |
12. | Arsenic | Liver, lungs, Skin |
(b) Physical Factors : Sharp teeth cause Tongue cancer. Kashmiri people keep 'Kangri' close to skin that cause skin cancer and this skin cancer is called kangri cancer.
(c) Radiation Factors : Cosmic rays, X-rays and U.V. rays cause cancer. There are 5 times more incidence of leukemia in Hiroshima & Nagasaki due to radiation effect of nuclear bombing.
(d) Biological Factors : Oncogenes (cancer producing genes) and on covirus cause cancer (HIV in AIDS.)
Investigation of Cancer
(i) Blood examination : Detection of the abnormal cells or cancerous cell in blood. Detection of the tumour marker like a-feto protein in blood by blood examination.
(ii) Biopsy : Cancerous tissue examination is called biopsy (Karyoplasmic index high).
(iii) F.N.A.C. (Fine needle aspiration cytology) - eg. breast cyst / tumour.
(iv) C–T scan, M.R.I, X-rays- X-ray of breast is called Mamography
(v) Pap smear : It is used for cervical carcinoma and detects cytological character of cancer.
(vi) Modern techniques monitor and detect the molecular changes that occur in cancer cells; this enables an early diagnosis of cancer. Monoclonal antibodies against cancer-specific antigens are coupled to appropriate radioisotopes. These antibodies are then used for detection of cancer.
Treatment of Cancer
(a) Surgery : By removing the entire cancerous tissue and infected lymph nodes.
(b) Radiation : Cobalt therapy (Co–60), X-ray radiations are given. These radiations destroy the rapidly dividing cells.
(c) Chemotherapy : Many anti-cancerous drugs like :-
Drug Mechanism
→ Vincristine (weed – cantharanthus roseus = Vinca rosea)
→ Vinblastin (weed – cantharanthus roseus = Vinca rosea)
→ Cyclophosphamide inhibit the DNA synthesis in cell cycle of cancerous cell but these drugs show many severe side effects.
(d) Immuno Therapy : Monoclonal antibodies and vaccine are given in it.
One of the recent approaches of cancer treatment involves augmentation of natural anti-cancer immunological defence mechanisms. Monoclonal antibodies have been used in various ways, e.g., radio immuno therapy,etc., for treatment of cancer. Research is in progress to develop cancer vaccines.
Most of cancer are treated by combination therapy of surgery, radiation and anti cancerous drug.
Additional Information
BIOMEDICAL TECHNOLOGIES
1. DIAGNOSTIC IMAGES
X-RAY IMAGING :
Introduction : It is one of the oldest method of imaging which began with the accidental discovery of X-ray by Wilhelm Conrad Roentgen, a German physicist, in 1895.
The branch of science that deals with the study of X-ray for detection and treatment of diseases is called radiology.
Principle : High dose X-ray
Uses :
(i) X-ray imaging is usually applied in detecting bone fractures and dislocations. This technique is also advantageous in detecting the diseases of heart and lung.
(ii) Barium meal.
(iii) Barium enema.
Advantage : Cheap and easy procedure
Disadvantage :Harmful to our body (Act as carcinogens)
Digital subtraction angiography (DSA) : DSA is an imaging technique that produces clear views of flowing blood in vessels and indicates the presence of blockages, if any. An angiograph (angeion : vessel, graghein : to record) is taken of the organ, for example, heart and its major blood vessels, and stored in a computer. A second angiograph is taken after a contrast agent containing iodine (I132). which is opaque to X-rays, has been injected into the blood stream. The first image is digitally subtracted from the second, leaving behind a clear outline of the blood flow to heart, brain or kidneys.
C.T. (COMPUTERIZED TOMOGRAPHY) SCAN :
Computerized tomography (CT) is also known as computerized axial tomography (CAT). This technique was invented by English physicist Geoffrey N. Hounsefield in 1972 (Tomo is a greek term 'cut' or 'slice').
Hounsefield is also called father of modern radiology (Nobel Prize in 1978).
The theoretical basis of this technique was provided by the work of the Indian biophysicist, Gopalsamudram N. Ramachandran.
Principal : Low dose X-rays ADVANTAGES :
(i) Improved contrast resolution between tissue not previously on plain radiography, eg.:- liver v/s gall-bladder, etc.
(ii) Ability to display cross-sectional images in the axial plane.
Uses :
CT scans are generally performed of the head and the abdomen. CT is valuable technique commonly used to investigate the brain following a stroke or if a brain tumour is suspected.
DISADVANTAGES :
(i) Expensive
(ii) Ionizing radiation involved.
M.R.I. (MAGNETIC RESONANCE IMAGING)
Given by Bloch + Purcell (N.P. 1952) The technique is based on magnetic resonance generated by the nuclei of hydrogen atoms subjected to an external magnetic field (upto 7–Tesla). It is based on NMR (Nuclear magnetic resonance) because our body cell is having H atom in the form of H2O molecule therefore our body acts as miniature magnet and generated magnetic field.
ADVANTAGES :
(i) No ionising radiation is used.
(ii) Images can be taken in any plane and obtain 3D image in single picture.
(iii) The inherent contrast between various tissues is better than with other modalities.
MRI detects water because it focuses on the behaviour of hydrogen atoms in water molecules. This allows MRI to distinguish between water-poor and water-rich tissues. Teeth and bones, which contain little water, do not appear in MRI. Therefore, tissues surrounded by bones, such as spinal cord, are readily observable in MRI. It is used to examine brain and spinal tissue, joint injuries and slipped disk in the spinal column. MRI can also visualize minute cancerous tumours, since radio frequency absorbed by the hydrogen atoms in such tissues for the same field is different from that for normal tissues.
MRI is superior to CT and PET. because -
(i) CT-scan can obtain only cross-sectional images whereas MRI can obtain images in any plane.
(ii) MRI is applicable in diagnosing tumours, infarctions (muscle cell death), haemorrhage, abnormalities related to spine, myocardial infarction (heart attack), myocardial ischaemia, coronary artery disease, etc. A related technique, called Magnetic Resonance Angiography (MRA), can be used to monitor the flow of blood.
(iii) Nuclear magnetic resonance (NMR) or magnetic resonance imaging (MRI) is a new noninvasive method of mapping the internal structure of the body.
DISADVANTAGES :
(i) Expensive
(ii) Patients with various metallic implants may not be able to undergo MR exams.
(iii) Claustrophobia can lead to inability to examine patients.
POSITRON EMISSION TOMOGRAPHIC SCANNING (PET) Discovered by Louis Sokoloff, 1987
(i) PET is also a computer based imaging technique but differs from CT Scanning. It provides information on the metabolic and physiological processes of the tissues and organs. The CT Scanning, on the other hand, gives only the 'static' anatomical images.
(ii) This technique involves the use of positron emitting short life radio isotopes (like 11C, 13N,15O and 18F).
These atoms are first incorporated into bio-molecules (such as glucose, amino acids, carbon dioxide and ammonia) and then injected in very small amounts into or inhaled by the experimental animal or human subjects.
As the radioactive atom decays, it emits a subatomic particle, called positron. Almost immediately, the emitted positron colloids with it antiparticle, i.e., an electron. This collision releases a burst of electromagnetic energy in the form of a pair of γ-radiation. This double emission is the key to the PET scan. These radiations emerge simultaneously in the opposite directions and they strike crystals in a ring of detectors around the patient's head, causing the crystals to light up.
(iii) A computer records the location of each flash and spots the source of radiation, translating that data into a 3D-image.
A metabolically active tissue will receive a greater blood supply than a relatively inactive tissue. Therefore, it will also get a greater supply of radioactive glucose, and would appear as a brighter area in the PET image. For example, the darkened area on the of brain indicates damage from a stroke.
Bright colours in the rest of the brain show normal blood flow. Thus, by tracing the radioactive glucose, a physician can pinpoint the areas of greater brain activity, e.g., the regions of brain involved in a particular function.
This versatile technique is used to study epilepsy schizophrenia, Parkinson's disease and drug addiction.
(iv) Recently, the scientists in U.K. have located the colour processing centres in the human vision cortex with the help of PET-imaging technique.
PET is useful in measuring :
(i) Metabolic rates.
(ii) Regional blood volume and blood flow.
(iii) Areas of abnormalities like disease and defects.
(iv) Identification of specific centres in brain like colour processing in visual cortex of humans.
SONOGRAPHY/ULTRASOUND IMAGING (Olaf von Ramm ; Donald, 1958) It is a noninvasive technique which uses ultrasound for producing images of internal body parts. Ultrasound is 'sound' beyond human hearing power, that is, above 20000 Hz or 20kHz. Diagnostic ultrasound used in sonography has a frequency of 1–15 MHz (MHz = megahertz = 1million oscillations/sec.) Ultrasound is produced through pizoelectric effect. Here, electric potential is applied to crystals of lead zirconate in a transducer. The crystals vibrate and produce ultrasound. Ultrasound is partly reflected as it passes from one layer to another. The reflected waves are picked up by lead zirconate crystals and changed to electrical signals. The latter produce a visual image which is observed over computer screen. Sonography provides images to all those organs or regions which are different or become different in density from surrounding tissues.
Sonography is also called Echography. For clinical examination, a sonographer places a scan head or transducer in contact with the area to be scanned. A layer of aqueous gel is applied between the skin and scan head to ensure that the sound has an air-free path to the object of interest, e.g., a foetus.
Sonography, safer than radiography, is comfortable and inexpensive.
Uses of USG :
It is used to assess foetal growth and to pick up a wide range of abnormalities, such as spinal bifida, and conditions liable to cause difficulty in labour.
Ultrasound imaging is used to investigate the internal organs such as liver, gall bladder, kidney, stomach, uterus, heart, etc.
A related technique, called Doppler Ultrasound Scanning is used to investigate the flow of blood in vessels and for detecting blood clots (Incoming blood – red, out going blood – blue). Sonography is also used to image the adult body. It even provides pictures of blood flow through the beating heart, based on a phenomenon known as Doppler effect.
Echocardiography is sonographic (ultrasound) imaging of heart, great vessels, heart valves, heart walls, etc. to know abnormality. It is also used to record blood flow velocity and blood turbulence.
ADVANTAGES: There is no exposure to radiation. Ultrasound imaging is non-invasive and painless. There is no harmful effects in man. It is less expensive. The images can be obtained in any plane.
DISADVANTAGES: Ultrasound imaging does not penetrate bones and air filled spaces so it is not useful in diagnotic abnormalities in the skull, lungs or intestine. Resolution power of ultrasound imaging is inferior to CT Scan and MRI
|
59 videos|290 docs|168 tests
|
FAQs on AIDS & Cancer - Biology Class 12 - NEET
| 1. What is AIDS and how is it different from cancer? |  |
| 2. Can AIDS lead to cancer? |  |
| 3. Is there a cure for AIDS or cancer? |  |
| 4. Can HIV be transmitted through cancer treatment? |  |
| 5. What are the preventive measures for AIDS and cancer? |  |






















